New antibody therapies may cut deaths, reduce exposure to COVID-19, data shows
The lab-created monoclonal antibodies could be a promising treatment for COVID.
While the push to get Americans vaccinated continues across the country, preliminary data has emerged that lab-created monoclonal antibodies could be a treatment for COVID-19.
The pharmaceutical company Regeneron said Wednesday its antibody cocktail appears to hold up against the U.K. and South African variants.
Researchers at Columbia University and Regeneron scientists each independently confirmed in tests the antibodies' success in neutralizing both variants.
The data is still preliminary and under peer review but could signal a useful tool as new mutations of the virus emerge.
Regeneron's antibodies have not been tested against the Brazilian viral variant yet, but the company said it expects the cocktail to remain "similarly potent."
Eli Lilly on Tuesday said its combination of two antibodies were effective in COVID-19 patients at high risk of severe infection, reducing the risk of hospitalization and death by 70%, according to results of a final-stage trial.
That same day, Regeneron announced that its monoclonal cocktail had shown positive initial results in being used prophylactically, helping ward off the virus in those who may have been exposed to the virus. Regeneron Chief Scientific Officer Dr. George Yancopoulos said he hopes the drug "may be able to help break this chain" of active infection and transmission.
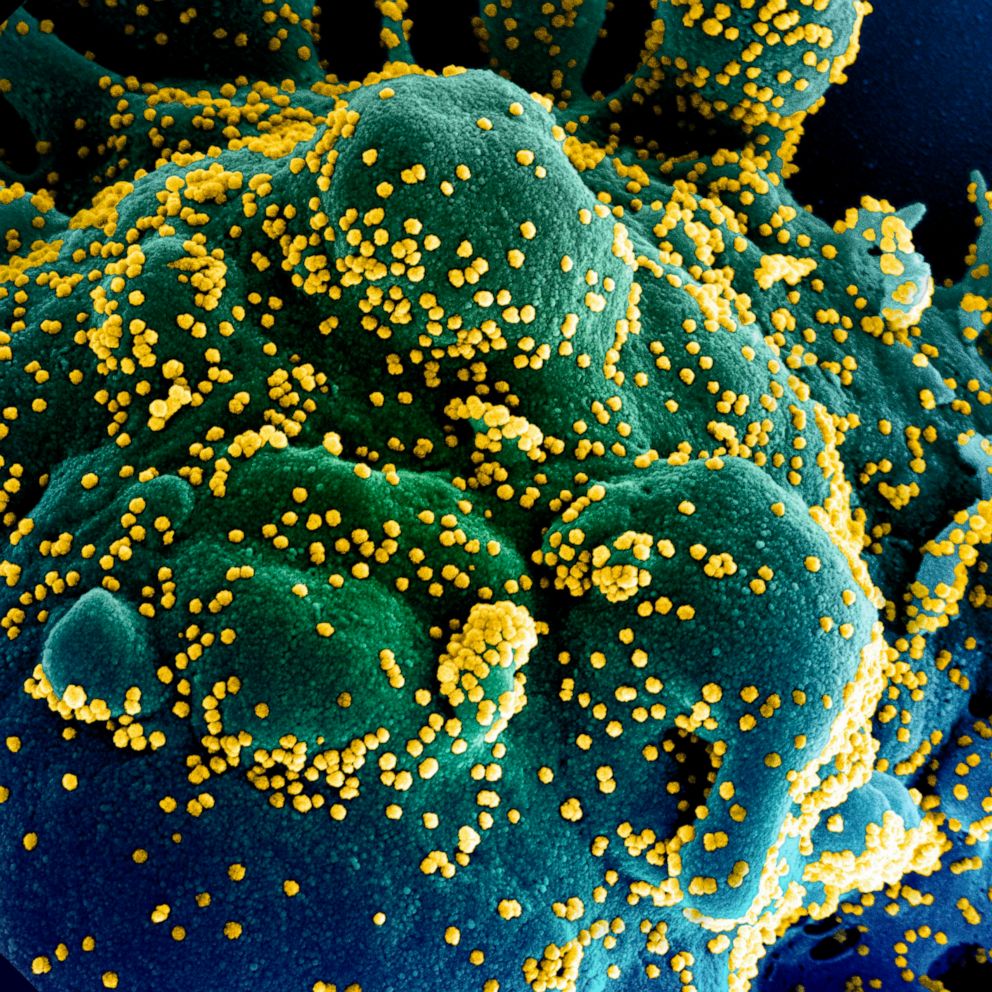
Eli Lilly also released data last week showing its antibodies may help prevent disease and stop outbreaks among nursing homes.
Currently, Regeneron's cocktail of casirivimab and imdevimab, and Eli Lilly's single bamlanivimab, have received emergency authorization from the Food and Drug Administration. They are meant to be used in the early stages of infection for non-hospitalized patients 65 and older and for those at high risk of severe illness to help keep them out of the hospital. The cocktails must be administered within days of diagnosis and are only for those with moderate to severe symptoms.
The government spent millions of dollars to make doses available to anyone who qualifies for it.
Such therapies could be an important tool in mitigating severe cases while also alleviating some of the pressure on strained health care systems.
Eli Lilly's news may signal one important mile marker: Combined antibodies bamlanivimab and etesevimab, working in tandem, may prove effective against a "broader range" of COVID-19 variants, company representatives said. This could be an essential tool as mutant strains continue to emerge.
With the new data in hand, Eli Lilly said it intends to begin global submissions for its combination therapy and request emergency authorization to use the single antibody bamlanivimab as a post-exposure "passive vaccine" treatment in nursing homes.
The "passive vaccine" use of monoclonals could offer stopgap protection, which works immediately against the virus, until enough of the population receives the vaccine required to reach herd immunity.
The FDA must still review last week's developments from both Eli Lilly and Regeneron to determine if the companies can bring these drugs to market for these new purposes and in these new forms.
The limited authorization under which Eli Lilly and Regeneron currently operate has rolled out in infusion centers across the country, with the Department of Health and Human Services building an interactive, national map tool to help locate where monoclonal antibody therapeutics have been recently received and are available for use.
Yet despite their availability and encouraging safety and effectiveness profiles, uptake of the therapies has been sluggish and "disappointing" in the U.S. -- as of the end of 2020, just 20-25% of supply had been used.
Besides lack of public awareness, an arduous infusion process, and staffing, have been a barrier to higher use of the therapies: health care systems are "crashing," Dr. Janet Woodcock, therapeutics lead for Operation Warp Speed, said in mid-January. Meanwhile, medical personnel are needed to help administer infusions even as ICU's desperately need them, too.
ABC News' Sony Salzman and Eric M. Strauss contributed to this report.




