New traumatic brain injury test is 'game-changing,' concussion experts say
There are millions of TBI hospitalizations and deaths each year.
In a world first, a newly authorized handheld device will allow doctors to detect traumatic brain injuries (TBIs) in under 15 minutes, potentially saving lives by dramatically shortening the time it takes to properly diagnose the issue.
The device is made by Abbott, a medical device company based in the United States.
“This is a huge milestone that has never been done before -- a blood test for the brain,” said Dr. Beth McQuiston, medical director for Abbott’s diagnostic businesses. “Until now, health care providers have needed to rely on subjective measurements for TBIs, but we finally have a more objective tool to help evaluate patients.”
Independent experts interviewed by ABC News agreed that this test for the brain may chart a new era in medical care for patients with TBI.
“I think this is groundbreaking. The first time we are able to assess brain health using a blood test,” said Dr. Frederick Korley, an associate professor of emergency medicine at the University of Michigan Medical School and a Michigan Concussion Center faculty member.
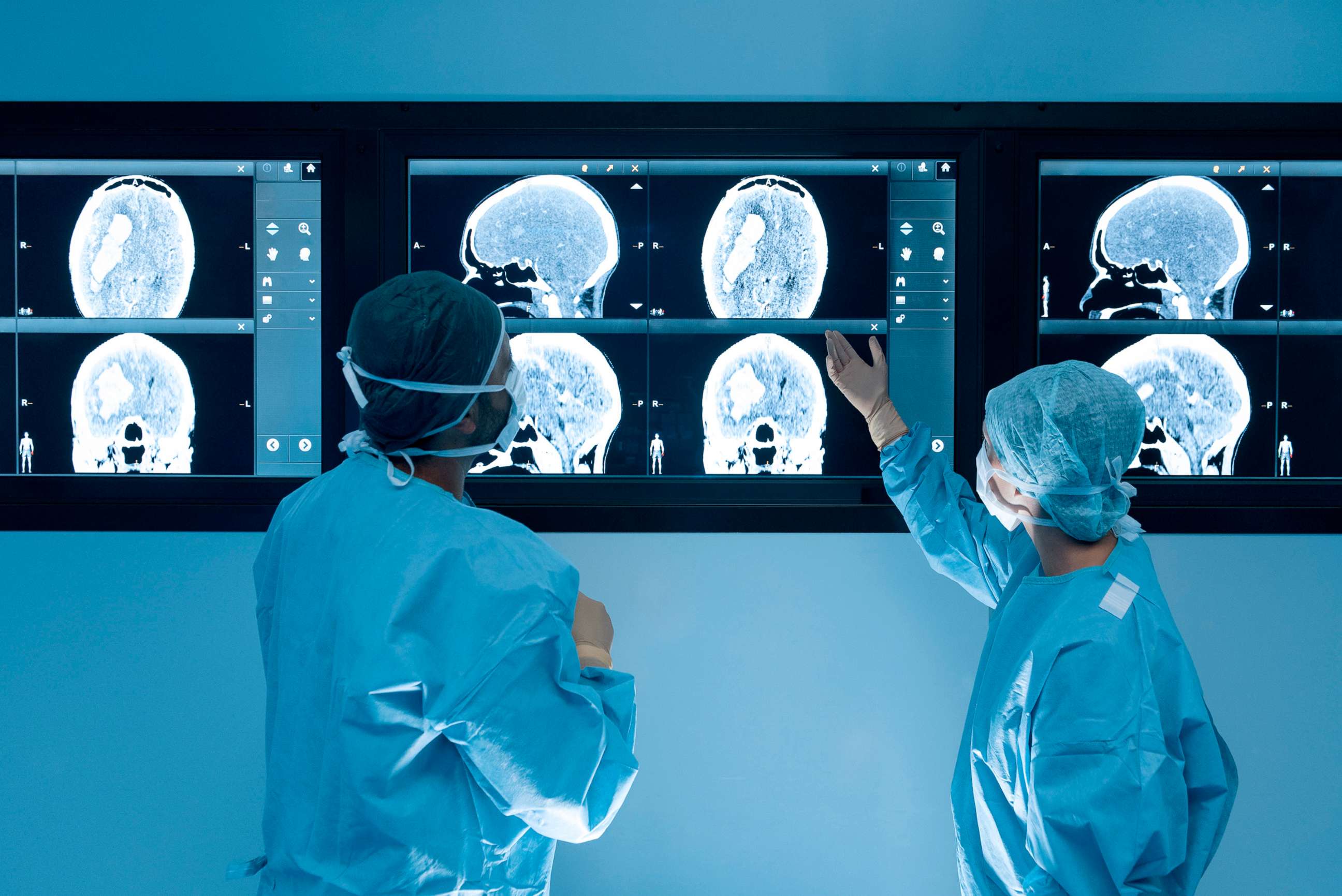
TBI is a disruption in normal brain function caused by a blow or jolt to the head. A concussion is the mildest form of TBI, but patients may suffer a constellation of physical, cognitive, emotional and sleep symptoms. Some of the most common signs include confusion, headaches, blurry or double vision, dizziness, fatigue, memory loss, difficulties with concentration and insomnia.
TBI is a major cause of death and disability in the U.S. There were 2.87 million TBI-related emergency department visits, hospitalizations and deaths in 2014, according to the Centers for Disease Control and Prevention. Athletes and older people are the most at-risk of TBIs.
Unfortunately, many patients with mild TBI struggle to get an accurate and timely diagnosis, even as they grapple with ongoing symptoms. This ultimately results in delayed treatment.
Doctors often use a series of screening questionnaires, physical examinations and CT scans to take pictures of the brain in order to evaluate TBI. However, experts agree these techniques aren’t perfect and there is no objective way to reliably evaluate TBI.
“One of the most challenging aspects of diagnosing concussion today is there are no objective tests,” said Dr. Farng-Yang Foo, a neurologist at NYU Langone Health's Concussion Center. “Currently, much of the diagnosis is by self-report of the patient, what the patient tells us. This makes it hard to make a diagnosis.”
Abbott’s new blood test may serve as an objective tool to help doctors triage TBI patients, because it relies on molecular signatures in the blood rather than on murkier clues, such as patient interviews.
The test requires a small blood sample drawn from the arm, from which plasma is extracted and inserted into the handheld instrument.
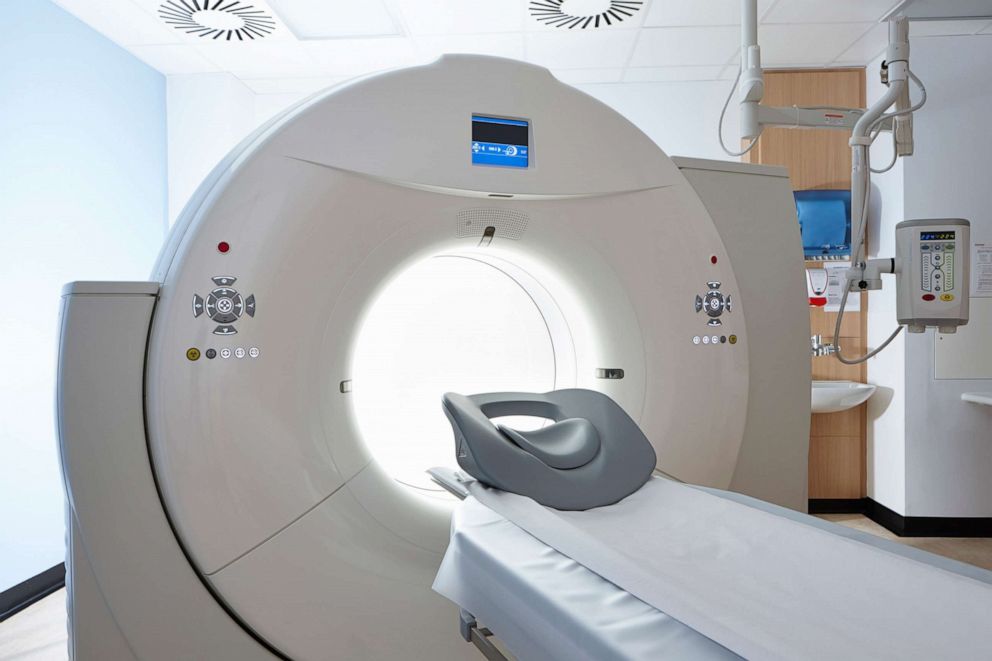
“The real value is in helping to guide emergency room and urgent care medical providers. The test will help them decide who needs to get a CT or MRI and who does not,” said Dr. Steven Flanagan, chair of rehabilitation medicine and co-director of the Concussion Center at NYU Langone Health.
The test was developed in collaboration with the Transforming Research and Clinical Knowledge in Traumatic Brain Injury (TRACK-TBI) research team and the U.S. Department of Defense. Dr. Geoffrey Manley, chief of neurosurgery at San Francisco General Hospital and principal investigator of TRACK-TBI, told ABC News this new test will improve patient flow in busy emergency rooms.
“I’m hoping there will be widespread adoption of this tool because it will facilitate getting people through the system quicker, getting people out of the emergency department that don’t need to sit there for 3 hours waiting for a head CT,” he said.
Preventing people from undergoing unnecessary CT scans can have far-reaching implications. Aside from reducing health care costs, it can save people from unnecessary radiation that has been shown to increase the risk of cancer.
“So many times people have to wait for these scans, causing longer lengths of stay in the ER, which is especially problematic in the COVID era,” Korley, the University of Michigan Medical School professor, said.
Despite the benefits, experts agree that physicians cannot rely entirely on this diagnostic test, stating it will only serve to supplement clinical judgment.
“You have to ultimately rely on clinical judgment. There’s always false negatives. You have to be cautious with that. The levels of GFAP and ubiquitin will never trump the judgment of an emergency room physician that someone really needs a CT scan,” Flanagan pointed out.
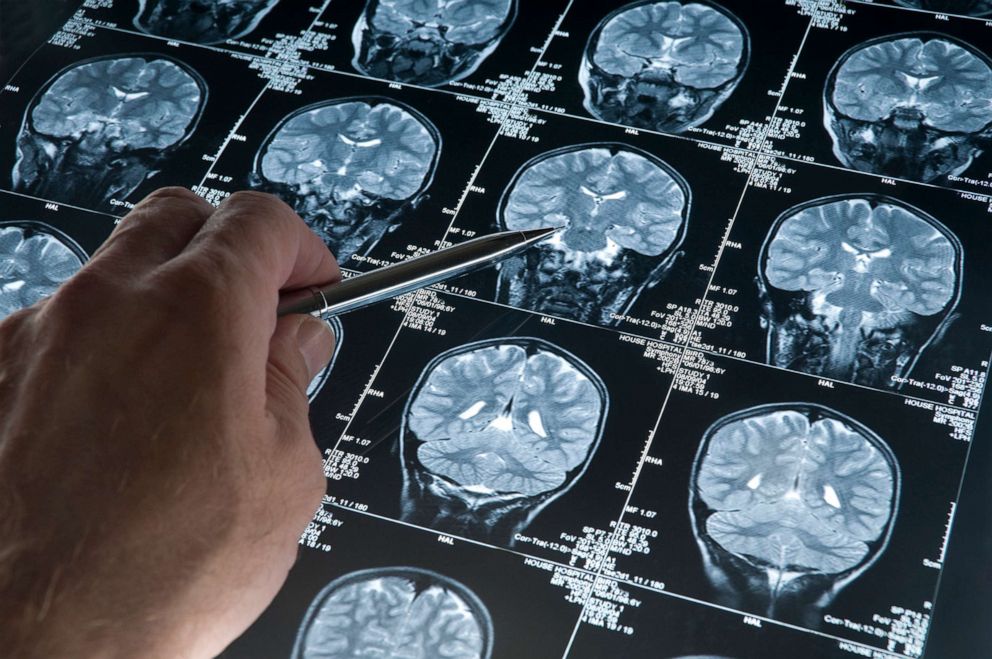
But the benefits of this test could reach beyond the emergency room. For example, it could be used on the sidelines of sporting events.
“It would enable us to be able to quickly diagnose a concussion and to make quick clinical decisions such as pull an athlete out of a game or send them for imaging,” Foo added.
According to the CDC, 50% of concussions go unreported or undetected.
“We were missing 50% of people that had TBI in the emergency department," Manley said. "The game-changing innovation of having a tool like this is that, as it becomes more widely used, I believe we will identify more people with TBI that’s more subtle, that could be life-altering."
Mishal Reja, M.D. is an incoming gastroenterology fellow at SUNY Downstate, and Leah Croll, M.D. is a neurology resident at NYU Langone Health. Both are contributors to the ABC News Medical Unit.