Doctors' Hand Hygiene Plummets Unless They Know They're Being Watched, Study Finds
Without supervision, doctors' hand-cleaning compliance plummets, study finds
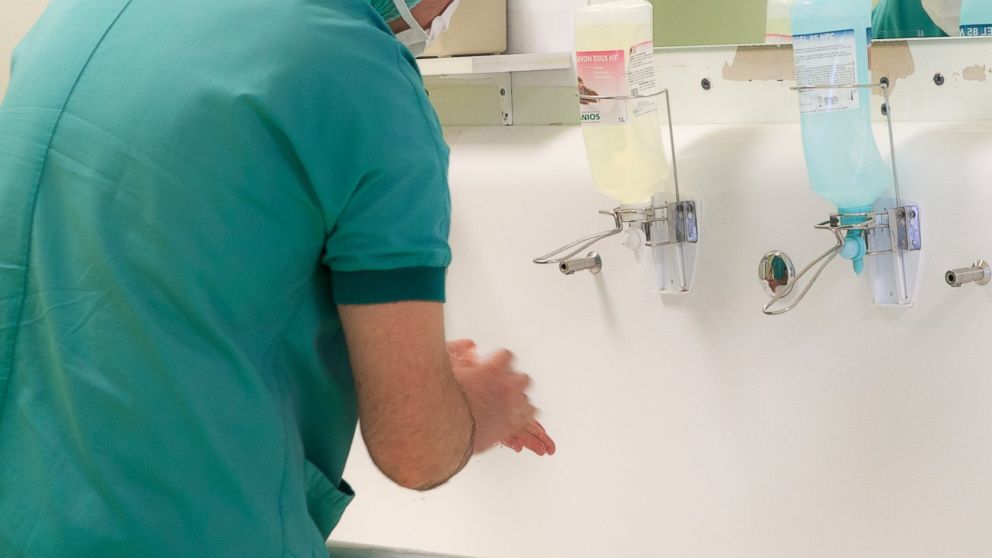
— -- For doctors and nurses, hand hygiene is supposed to be as intuitive as breathing. But is this behavior really second-nature, or do health care workers need supervision to keep their hand cleaning habits on target?
A new study out of Santa Clara Valley Medical Center (SCVMC) in San Jose, California, suggests that even doctors may fall prey to what is known as the “Hawthorne Effect” -- whereby people change their behavior when they know they’re being watched.
The study, being presented this weekend at the Association for Professionals in Infection Control and Epidemiology (APIC) conference in North Carolina, found that hand hygiene compliance at SCVMC differed dramatically when health professionals knew they were being evaluated, versus when they did not.
Because infection-causing bacteria are often carried from patient to patient on the hands of health care workers, breaking this chain of transmission is a top priority in hospitals nationwide. But this study -- and many others -- indicate that while the principle of hand hygiene is simple, human behavior is one of the hardest things to change.
Hidden Observers
The researchers at SCVMC had two types of auditors assessing hand hygiene: Infection Prevention (IP) nurses, who everyone in the hospital recognized as the hygiene patrol, so to speak, and high-school and college-aged volunteers who were trained to perform the exact same assessments, but who were not consistently recognized as such by hospital staff.
As the study progressed, one pattern grabbed the researchers' attention.
“[We noticed] a very consistent trend that our Infection Prevention nurses were seeing something different than what volunteers were seeing,” Maricris Niles, an infection prevention analyst at SCVMC, told ABC News. Specifically, the IP nurses noted much higher compliance rates.
The researchers wondered whether it could be that compliance was being recorded differently by different observers. Extra measures were taken to ensure that this was not the case. What it came down to, it seemed, was the Hawthorne Effect.
“When we would come on the floor, I would notice that the nurses or providers were not using the alcohol,” Lisa Hansford, one of the recognizable IP nurses at SCVMC, told ABC News. “Then they would glance up and see me and bend over backwards to lather up.”
The investigators found the hand hygiene compliance rate observed by IP nurses was about 57 percent, while hospital volunteers -- who tended to blend in and not be recognized as hygiene auditors -- recorded rates of about 22 percent. While this phenomenon has been noted before, the team at SCVMC was surprised by the stark gap--and they have launched a series of interventions to try and drive their compliance rates higher and higher.
Health workers "make the decision [about hand-washing] in the moment -- and sometimes they get so wrapped up in what they’re doing that they need to be reminded,” SCVMC infection prevention manager Nancy Johnson told ABC News. “This is a reminder that they need to make that choice to wash their hands.”
Clean Hands Count
Poor adherence to hand hygiene has been a longstanding issue. According to the U.S. Centers for Disease Control and Prevention, health providers clean their hands less than half of the time they should, and the World Health Organization reports averages as low as 40 percent.
How much hand hygiene is enough? Guidelines vary, but according to Dr. Clifford McDonald, associate director for science at the CDC, nurses or doctors in the intensive care unit may have to clean their hands over 100 times in an eight-hour shift.
SCVMC and many other hospitals are working on ways to increase compliance. One strategy involves publicizing compliance data -- apparently, some hospital departments enjoy some healthy competition.
Another study being presented at APIC from the Henry Ford Health System in Detroit found that hand-washing rates improved after hospital staff members were shown images of millions of bacteria found on common surfaces. Appealing to human emotions -- like disgust -- seems to have had a meaningful impact.
On May 5, the CDC launched a “Clean Hands Count Campaign” to promote hand hygiene adherence in hospitals. Part of their mission is to empower patients to hold healthcare workers accountable for cleaning their hands.
McDonald encourages patients to remind doctors and nurses to sanitize their hands -- even though it might feel like an uncomfortable shift in the traditional power dynamic.
“If we can get the patients more involved in that -- and get them to be able to speak up, that is really the main thing,” he said. “A lot of patients are nervous about that kind of thing -- that’s another culture we’re trying to change.”
‘No System Is Perfect’
McDonald noted that -- except in specific environments where soap and water are required -- alcohol rubs are the preferred mode for hand-cleaning: they are more effective at destroying bacteria, and less aggravating to skin.
Some hospitals are experimenting with electronic monitoring techniques where alcohol dispensing stations keep track of how often healthcare workers lather up.
But Dr. Sharon Wright, hospital epidemiologist at Beth Israel Deaconness Medical Center, pointed out that “no measure of hand hygiene is perfect.”
For example, with electronic monitoring, you lose the ability to give specific feedback on how individual workers can improve their practices. But on the other hand, direct human observation is more labor-intensive, and may inflate overall compliance results.
After working on these issues for 16 years, Wright hopes to see a more robust culture shift in the near future.
“I wonder why it is that we’re still working on it,” she said. “My hope is that for younger clinicians when you pass [an alcohol] dispenser you feel funny if you don’t hit it -- like putting on a seat belt when you get in a vehicle.”



