Latino nurses push through COVID-19 burnout, sleepless nights and lost loved ones
"The death has been … one of the hugest life-changing events for me."
Six months since COVID-19 was declared a national emergency in the United States, Latino health care workers say they’re burned out as new information about the virus changes work protocols, traumatized by the virus’s impact on those they’ve cared for and saddened by the way in which the virus has ravaged their community.
“What I’m seeing now is the patients are coming in sicker and they’re taking longer to recover,” Mary Juarez, a registered nurse in Los Angeles, told ABC News. “It’s generally seen mostly in the Latino population, so of course, I am very, very aware of that. … My anxiety level is 100% more. My anxiety begins a day before going into work.”
Juarez has been working in the cardiology progressive care unit at LA’s Good Samaritan Hospital, which has been turned into a COVID-19 unit. Over the last few months, as California saw cases surge, she says her experience at work has been unlike anything she’s seen in her 20 years of being a nurse.
“The death has been … one of the hugest life-changing events for me,” said Juarez, who is also the union representative for the California Nurses Association at Good Samaritan. “There was a period in this pandemic when we were putting patients in body bags once a shift. Not once every 24 hours, but once a shift. Day shift, night shift."
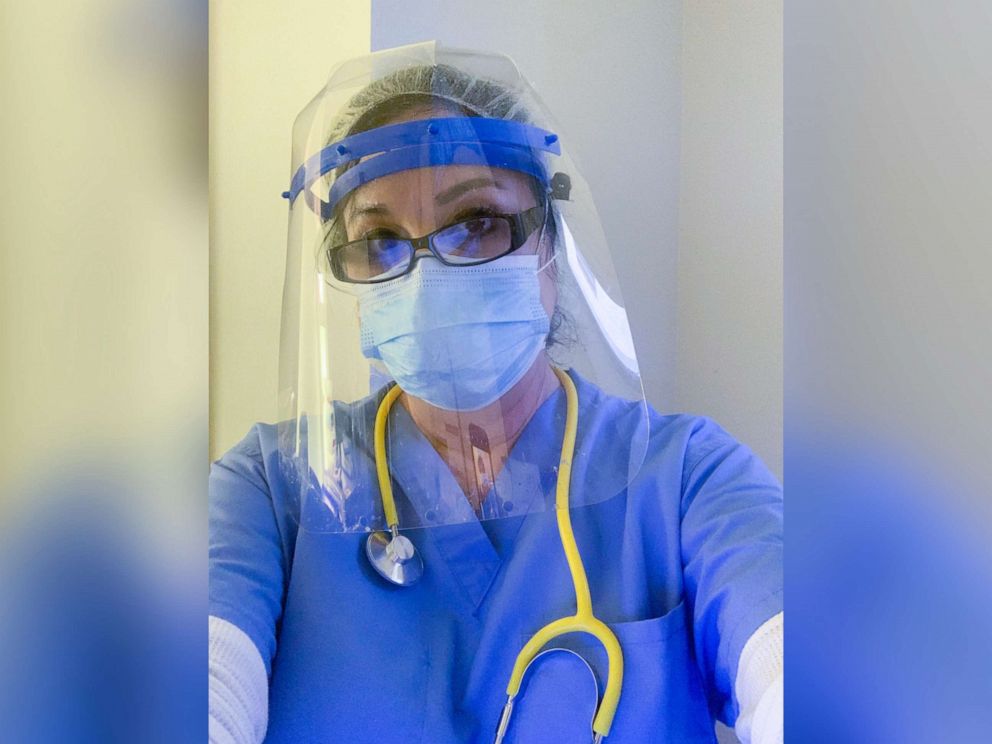
“Oftentimes there was more than one,” she continued. “So to face that as a nurse, having never experienced that before and certainly never expected that before, that is something that’s going to stay with me for the rest of my life.”
Latinos, like other racial and ethnic minorities, have been disproportionately affected by COVID-19 in the United States. They are 2.8 times as likely to be diagnosed with the virus and 4.6 times more likely to be hospitalized, according to the Centers for Disease Control and Prevention (CDC).
But the COVID-19 toll on the Latino population is more than just physical; it’s mental, too.
A CDC survey from last month found Hispanics reported more symptoms of anxiety, depressive disorder, suicidal ideation and increased substance abuse to cope with their pandemic-related stress. These symptoms were more prevalent among essential workers, unpaid caregivers for adults and those with pre-existing mental health conditions.
Since the beginning of the pandemic, Nadine Kaslow, Ph.D., a professor in the Department of Psychiatry and Behavioral Sciences at Emory University School of Medicine, has been supporting front-line workers by going into the intensive care units (ICUs) where COVID-19 patients are being treated. She says the staff she’s spoken to have entered somewhat of a “disillusionment phase.”
“People are really tired. They’re exhausted. … The uncertainty, unpredictability, and the sense that there’s no end in sight. People [are] not getting their normal breaks they would get over the summer to travel and do things like that. I think that’s really added to the stress and sense of burnout,” Kaslow, who is also a former president of the American Psychological Association, told ABC News.
She said that with restrictions around visitors in hospitals, Latino health care providers have taken on the role of being patients’ advocates, helping to translate and explain things to family members. Having family members around, she says, is a key to the healing process for many patients.
Stephanie Perez is a pediatric ICU nurse at a hospital in New York City whose unit began admitting 20- and 30-year-old COVID-19 patients at the height of the pandemic, when people of all ages -- not just the elderly -- began getting sick. She saw the healing power of family firsthand with a patient who had been placed on life support. She said he was constantly concerned about his family.
“We ended up finding out that he had a newborn at home, so we just tried to console him, like, ‘Your daughter is fine. You’re OK,’” she said. “When his wife would call, he would ask how everything is there. … and we would see his numbers and his vital signs get better.”

To date, the United States has been hit harder than any other country by the pandemic, with more than 6.5 million diagnosed cases and at least 193,976 deaths.
New York City hit its peak in April, with a seven-day average of 5,305 cases per day, according to the New York City Department of Health and Mental Hygiene. Now long past its peak and with new cases of COVID-19 continuing to drop, Perez no longer cares for COVID-19 patients. However, the pandemic continues to affect her.
Perez said she and her boyfriend, Greg Rousseau, a medical ICU nurse in New York City, are used to traveling during the summer, yet neither of them has been able to go on vacation. As the city reopens, even everyday forms of releasing stress have been difficult for Perez to partake in without feeling guilty.
“There’s this expectation that you’re here to serve the community; you can’t live your life or enjoy yourself,” she said. “Obviously, restaurants -- all these public places -- are now under serious precautions. . . . [So] you’re already dealing with it 24/7 at work and doing all those precautions there and you don’t have an outlet really to even go and enjoy yourself without feeling like you’re letting your unit down, letting your coworkers down.”
"You can only really just do two things," Rousseau added. "It’s just work and go home, work and go home. So, you know, that sort of cycle is a bit taxing at times. But just staying the course and trying to stay strong, thinking that there are better days ahead is what’s most encouraging at times."

Perez and Rousseau were living with their families in March when COVID-19 surged in New York City -- he was in Brooklyn and she was in the Bronx. Both Perez’s father and Rousseau became ill with COVID-19 around the same time. Rousseau was moved to a hotel 10 minutes away from Perez so that she could take care of him. She also quarantined her father in her parents’ bedroom while she slept with her mother, a breast cancer survivor with a compromised immune system, in her own bedroom.
“I was bouncing between taking care of [my father], taking care of Greg, going to work, trying to be superclean and then dealing with my mom, who was going crazy in the house with her anxiety,” Perez said. “It’s a lot.”
Rousseau and Perez’s father were both able to recover from the virus, and the couple has since bought a house together and moved out of their families’ homes.
All the while dealing with COVID-19 in New York City, Perez and Rousseau were also watching the outrage grow over the death of George Floyd, which sparked months of nationwide protests against police brutality.
Perez and Rousseau, who is Haitian American, joined these protests, and the weight of social injustice was added to the burden they already carried as front-line workers.
“I started to eat, sleep, breathe [Black Lives Matter]. It sucked, drilling into Greg’s head that he could be fighting the pandemic one minute, literally saving lives like Breonna Taylor, and [then] someone could turn around and take his life in the blink of an eye,” Perez said. “It was and still is so stressful.”

The rise of anxiety and depression symptoms among Latinos is the cumulative result of a number of factors converging, Kaslow says.
“I think a lot depends on one’s own personal experience. How personally you were touched both at your job and in your personal life,” she said. “We certainly have health care workers that have lost family and friends and lots of patients. I think that the grief of that is just tremendous and there’s no time to heal from the grief.”
For Rosario Salazar, an emergency room nurse at an LA hospital, there were stressful moments in her personal life and at work. Her godmother, the mother of six of her cousins and a stage 4 cancer patient, died from COVID-19.
Salazar said the virus spread through her godmother’s household soon after her cousin called her to say she had been diagnosed and that she was afraid she’d spread it to the rest of the family. Salazar said that within days, all six of her godmother’s children became ill. They called Salazar and asked her to come and check up on their mother.
“I kind of had a feeling that she wasn’t going to make it out of this one,” Salazar said. “Based on what I was seeing, based on what I knew: she’s stage 4 cancer. She gets this cough. It’ll just start developing into something else.”
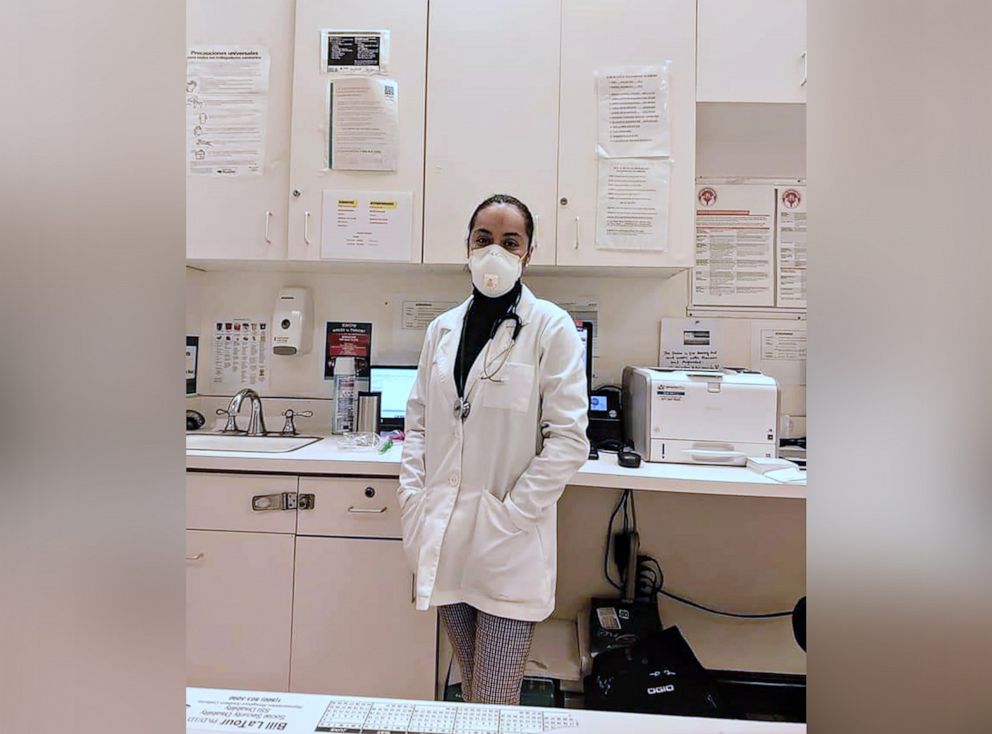
Salazar said her godmother went to the hospital a day later and that “her oxygen levels were really low.” Being a medical provider, she said she was able to gain visitation access to see her godmother, but her cousins could not.
“So I had to call [them]. I was in the room for two hours in my full gear … and I had each one of her kids call and say their goodbyes. Even though she wasn’t very coherent, that gave them closure,” Salazar said. “She passed away a day later.”
As an ER nurse, Salazar says she feels that she and her colleagues are expected to deal with worst-case scenarios on a regular basis.
“I think it was just a matter of, you know, we're all a team. We have to deal with it the way we can. And we could deal with this,” she said.
Salazar says that personally, being a front-line worker during the pandemic hasn’t been traumatizing. She expressed appreciation for the job she has and the “nice home” she can return to, where her ER doctor husband and her children remain healthy. She also said she doesn’t consider herself a hero.

“To me, it’s just my job, and my job was to protect myself and other patients,” Salazar said. “I felt more for the overall people that were suffering from it, and mainly for the people of low socioeconomic status not being able to go to work.”
Salazar, who is in graduate school to become a nurse practitioner, has been doing clinical rotations at a community health clinic where she says many Latino patients who’ve lost their jobs come in.
“I think what made it mentally taxing for me was hearing the patients; hearing their stress and how vulnerable they were during this time,” said Salazar. “You know, the stress of losing their jobs and worrying about how they were going to feed their families. Hearing that, I think, put a little stress on me.”
There’s been uncertainty with regard to the use and availability of personal protective equipment (PPE) for each of the health care workers ABC News spoke to at different stages of the pandemic.
Juarez says she hasn’t been protected enough by her hospital in LA. Even today, she says her colleagues are still given only one single-use N95 mask to wear throughout the day -- they can ask for a second one if it becomes soiled -- and that they wear surgical masks and donated face masks on top of them to keep them as clean as possible.
“It causes me great concern because I need to know that as a nurse I’m going to be protected enough to go into these rooms and take care of these patients who are sicker,” she said.

Even having the one mask per shift was a “fight for our rights” to have the proper PPE, Juarez said.
“Even after everything that had happened in New York in the beginning, we were told not even to wear a mask, not even a simple surgical face mask, by our administration,” she said, adding that this happened in March when there were no protective guidelines in place. “So that was a huge deal for us because all we wanted to do was wear a mask when these patients came in.”
In a statement, Good Samaritan Hospital said it has followed PPE guidelines from the CDC and the California Department of Public Health, including for “the use of masks throughout the coronavirus pandemic. We have maintained a high supply of masks and continue to provide appropriate masks for our physicians, nurses, staff, patients and visitors at all times.”
Health care workers who aren't directly working with COVID-19 patients are also feeling the fatigue of new processes implemented to protect them and prevent the transmission of the virus throughout their facilities.
Betsy Arlene Tirado, a pediatric cardiac ICU nurse manager in Miami, says they're "very lucky in the pediatric world because we were not hit with the same intensity and the same volume as adult facilities."
Only 7.3% of COVID-19 cases in the U.S. have been in children, according to the CDC, which says hospitalizations rates are also much lower than in adults. Still, even with a low percentage of COVID-19 patients, she says they’re treating “everybody like they have COVID.”
“So before, we would wear maybe a mask if we thought the kid was infected,” she said. “Now, it doesn’t matter. … You always wear a mask. You always wear face shields. You always wear full PPE with the possible exception of an N95,” she said. “Those can be reserved for COVID patients or patients you suspect are positive.”

Keeping up with the new processes her facility has implemented, however, has been tiring and she says the pandemic has “without question” been traumatizing.
“It’s been a lot of sleepless nights. … With the process changes, especially to the extent that we’ve made them, there’s always questions. You always find holes, room for improvement,” said Tirado, who is also the secretary for the Miami chapter of the National Association of Hispanic Nurses. “So it’s been a struggle and it’s going to be a struggle for quite a while.”
“You’re constantly living in fear, because there were not consistent answers from guiding entities, especially in the very early phase of this,” she added.
Before the pandemic, many hospitals were also already facing or bracing for nurse shortages. Juarez says her unit hasn’t been adequately staffed to care for the amount of COVID-19 patients they’re seeing.
“It goes full circle here,” Juarez said. “We’re short-staffed because the staff that we do have is burnt out. They’re overwhelmed, and the fact that we’re not getting more staff to help us, it just goes round and round in a full circle. So yes, some nurses have retired. Some nurses have left. … There’s nurses that are on medical leave because it’s just sheer exhaustion.”

In its statement, Good Samaritan said it “faced an increase in staff sick calls during the peak of the coronavirus pandemic. To maintain appropriate staffing ratios, we called in additional staff to float from other units as well as registry nurses to support staff on those units with increased absenteeism.”
Despite their struggles, each of these health care workers expressed great pride in their work. Salazar said it’s “rewarding” seeing how her work benefits patients and that she derives strength from it.
“During this pandemic, I get to work in a field where I’m actually helping or contributing to someone’s improvement in health, or helping the vulnerable populations. Anything I can do, that keeps me strong,” she said.
Still, Juarez says it’s important for all nurses to get the support they need to do their jobs successfully. Juarez said she “feels strongly” that the mental health of those on the front lines has not been addressed, “and it’s a very real issue for us.”

“Unless you are in it, you have no idea what it’s like. You have no idea what it’s like to feel that emotion and that attachment that you do to our patients and then knowing there’s only so much you could do for them,” she said.
“I didn’t sign up for this,” Juarez continued, referring to the pandemic. “I signed up to take care of patients; to do my best. . . . You know, I’m [of] service to others.”




