Nurse who lost her baby after contracting COVID-19 urges pregnant women to get vaccinated
Vanessa Alfermann was just 22 weeks pregnant when she gave birth.
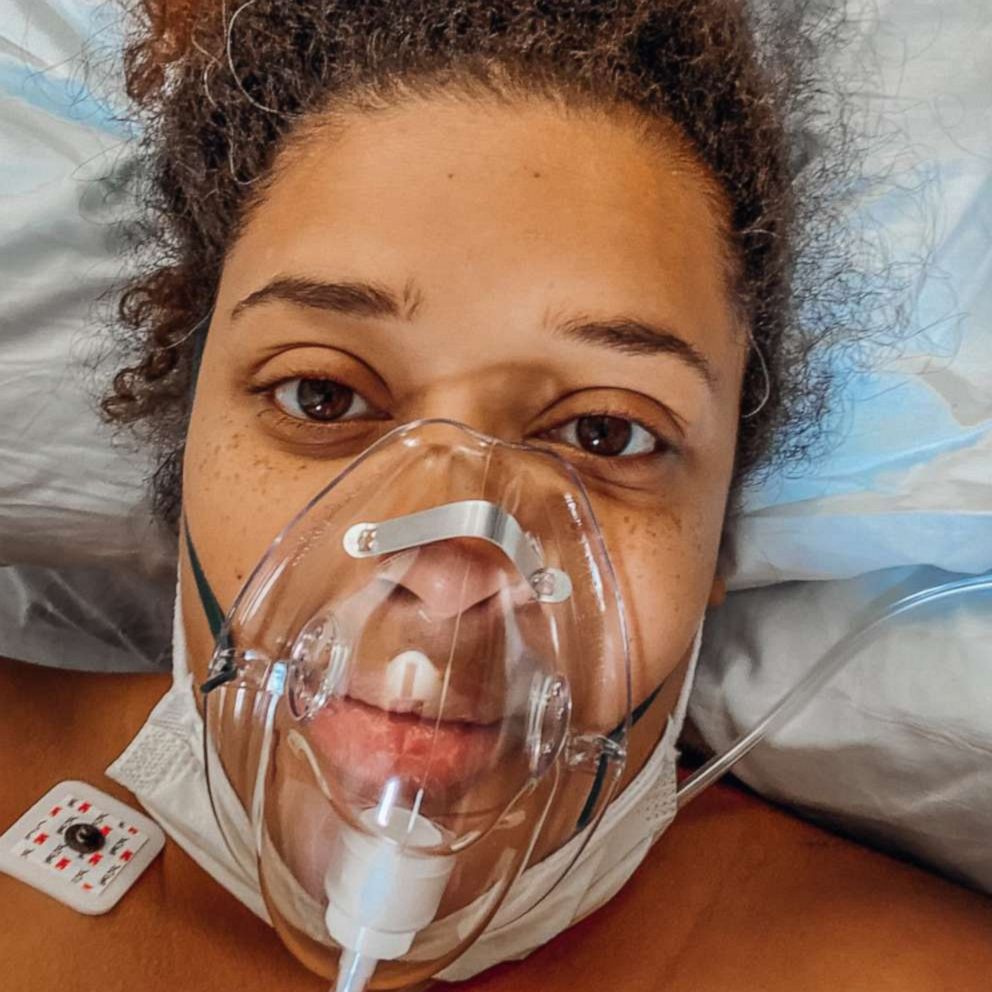
A Missouri mom whose newborn son passed away after she gave birth to him while battling COVID-19 is speaking out in order to urge pregnant women to get vaccinated.
Vanessa Alfermann, a registered nurse from Franklin County, says she was 22 weeks pregnant with her second child when she contracted COVID-19 in November, before the first COVID-19 vaccine received emergency authorization from the Food and Drug Administration (FDA).
"My husband had symptoms and he tested positive and the next day I also tested positive," Alfermann, 33, told "Good Morning America." "I never had shortness of breath but was just really tired."
Alfermann said she had more symptoms of COVID-19, like a loss of taste and smell and headaches, but never experienced the more serious complications she sees COVID-infected patients suffer from at the hospital, Missouri Baptist Sullivan, where she works.
Around 10 days after she first tested positive for COVID-19 though, Alfermann began experiencing back pain and cramps and went to see her OBGYN.
"The baby was fine [in an ultrasound] but my white blood cells were really high and they said I had an infection from COVID and gave me an antibiotic and some muscle relaxers to go home with," she recalled. "The next morning at about 1:30 I got up and realized I was in labor."
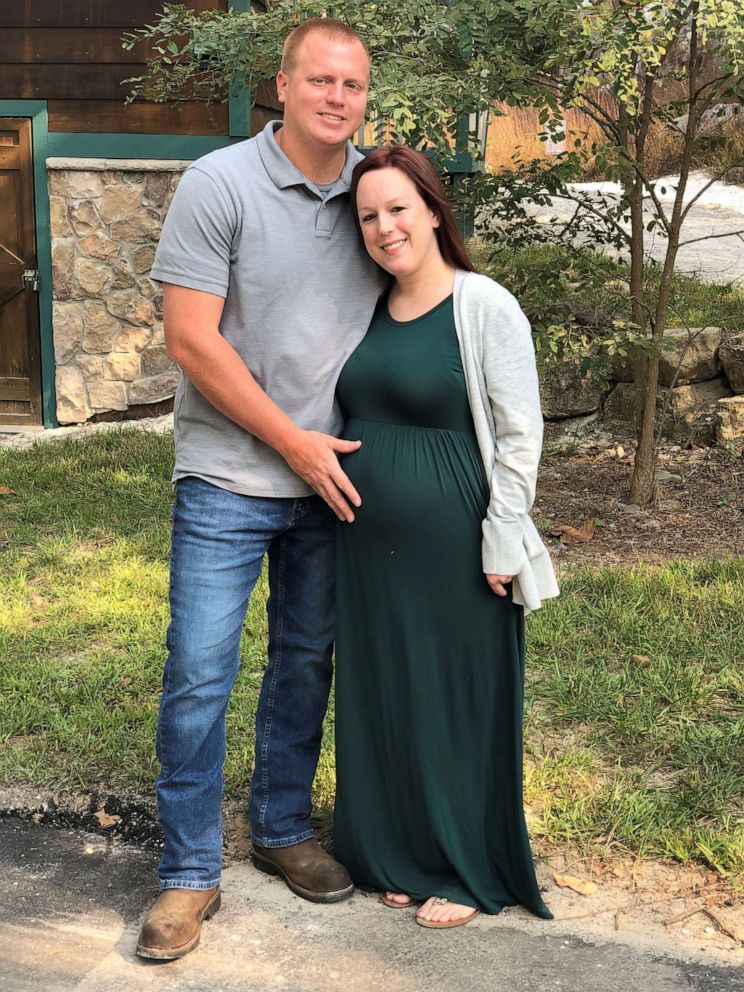
Because her husband was still isolating due to his own COVID-19 diagnosis, Alfermann's mother-in-law drove her to Mercy Hospital in St. Louis, where she would quickly give birth to her son, whom she named Axel.
I didn’t even get to hold him.
"Within a half hour from me getting there and getting up to the [labor and delivery] floor, Axel was born," said Alfermann. "I didn’t even get to hold him. The NICU people held him and he took his breath with them and then he passed away."
Alfermann said doctors told her she suffered a placental abruption, a pregnancy complication that happens when the placenta separates from the uterus. In her case, the abruption was caused by blood clots in the placenta due to COVID-19.
"It was mind-blowing because don’t think you’re going to get a blood clot on your placenta. [You think] you’re going to be put on a ventilator because you can’t breathe," Alfermann said, referring to respiratory problems that were the most well-known COVID-19 complication at the time. "I went through all of these emotions but I also thought if this is what’s coming, what COVID does, it just scared me."

Placental abruption can be a deadly complication for the mother. Alfermann said she is thankful she survived and is able to still be here for her family, including her husband, son and stepdaughter.
As she continues to walk through the grief of losing a child, Alfermann said she is sharing her story to help encourage pregnant people to get vaccinated against COVID-19.
There’s so much misinformation out there that’s killing people and it’s frustrating.
"There’s so much misinformation out there that’s killing people and it’s frustrating," she said. "I speak out about this for Axel’s legacy ... because there shouldn’t be another Vanessa or Axel."
Alfermann, who was vaccinated against COVID-19 in December, said she thinks about how her life may be different if the vaccine had been available during her pregnancy.
Describing the moment she received her first vaccine shot in December, Alfermann said, "I was so happy because I was protecting everybody else but I went upstairs to our bathroom and just cried because I thought 'what if.' What if five or six weeks earlier I could have gotten the shot? I could still be waiting to have my baby boy."
"It’s very bittersweet," she said.

Earlier this month, the Centers for Disease Control and Prevention (CDC) strengthened its recommendation for COVID-19 vaccination during pregnancy, stating that all women who are pregnant, breastfeeding or trying to get pregnant now or might become pregnant in the future should get a COVID-19 vaccine.
Still, 3 out of 4 four pregnant women in the U.S. have not yet received a COVID-19 vaccine, according to new data from the CDC.
The low vaccination rate among pregnant women combined with the more infectious delta variant spreading in the U.S. has led to an increase in hospitalizations among pregnant women, including in the St. Louis-based healthcare system where Alfermann works.
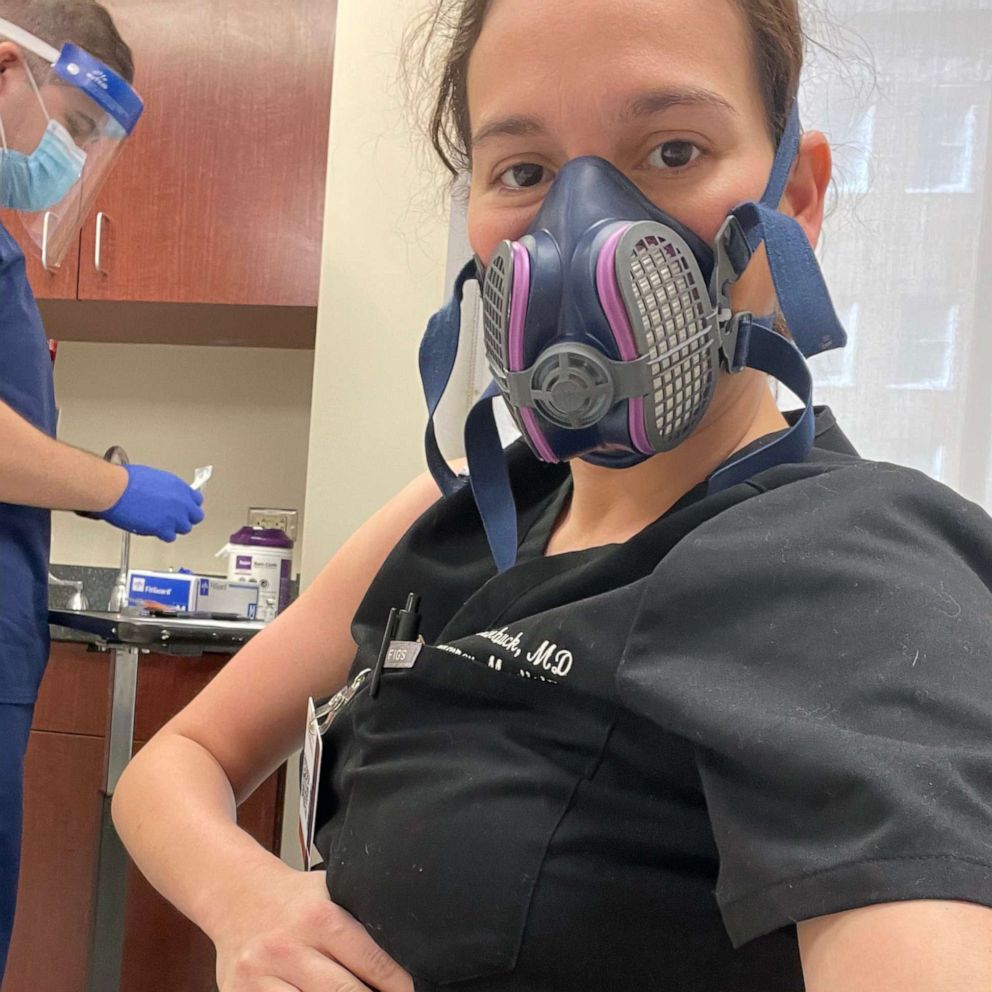
"We’re getting pretty desperate," said Dr. Jeannie Kelly, a Washington University obstetrician at Barnes-Jewish Hospital in St. Louis, part of the BJC HealthCare system. "We have had to say no to transfers because we are completely full and that in my eyes is just unacceptable for American medicine in 2021 and it’s infuriating that we’re here at this point."
All of us who are taking care of pregnant patients at this point are really worried.
"I think all of us who are taking care of pregnant patients at this point are really worried, are really concerned and are really scared," she said. "It’s a really hard situation for a pregnant person who is in the ICU with a baby who is also sick because mom is so sick."
Dr. Laura Vricella, a maternal fetal medicine physician at Mercy Hospital, where Alfermann was treated, said the hospital is also seeing record number of COVID-positive pregnant patients.
"In the past month we have seen the largest amount of pregnant people being hospitalized with COVID, and be critically ill with COVID, than we did at any time last year, said Vricella. "We have eight [pregnant people with COVID-19] in the hospital now, five are critically ill and virtually all are unvaccinated."
Vricella, who was not involved in Alfermann's care, said doctors and researchers are learning more and more now, as the pandemic continues, about the negative effects COVID may have on pregnant people.
"What we’re seeing right now is that COVID-19 seems to be much more dangerous for pregnant people than what we were seeing in the spring," she said. "This is why the three national bodies [the CDC, the American College of Obstetricians and Gynecologists (ACOG) and the Society for Maternal-Fetal Medicine (SMFM)] are now recommending the vaccine in pregnancy regardless of timing."
COVID-19 is especially dangerous in pregnant people because their immune systems are already less active in order to support their growing fetus and their hearts and kidneys are already working harder during pregnancy to support the fetus, according to Vricella.
Pregnant people must also keep their oxygen levels higher in general to support their fetus, which can be a herculean task to do when COVID-19 is in the body, according to Vricella.
And in addition to pregnant people with COVID-19 being more likely to deliver prematurely, Vricella said her hospital is also seeing more COVID-positive pregnant patients deliver stillbirths, even with mild COVID cases.
"COVID-19 begins as a respiratory illness but can affect the entire body and also seems to increase the risk of thrombosis or blood clots," she said. "We suspect that this decreased oxygen to the fetus may be responsible for the stillbirths that we are seeing, though we need further research."
Just as doctors are learning more about the complications of COVID-19 in pregnant women, they are also seeing more data about the safety of the vaccines, according to Vricella.
The overwhelming evidence indicates that the vaccine is safe.
"The risks of COVID are much, much greater than the theoretical risks of the vaccine," she said. "The overwhelming evidence indicates that the vaccine is safe."
When the CDC strengthened its recommendation for COVID-19 vaccination during pregnancy this month, it did so citing new evidence of safety with the vaccines, a point that Kelly also stressed.
"I tell my patients that at this point, the [COVID-19] vaccine is one of the most studied medications, or interventions, during pregnancy," said Kelly, noting that over 140,000 pregnant people have been vaccinated and doctors now have nearly nine months of data pointing to the vaccine's success. "During pregnancy, we’re pretty excited when we see a study come out with a couple thousand women enrolled in it, and now we’re talking so many more numbers than we typically see for any other type of research in pregnancy."
What the FDA’s approval of the Pfizer COVID-19 vaccine means
Both the Pfizer and Moderna vaccines also use mRNA technology, which doesn't enter the nucleus of the cells and doesn't alter human DNA. The two COVID-19 vaccines are the first mRNA vaccines, which are theoretically safe during pregnancy, because they do not contain a live virus.
"It's never too late and it's never too early," Vricella said of when pregnant women should get vaccinated. "I think the fall could be a really terrifying time for pregnant people if we don’t increase their vaccination rates quickly."