Burying Ebola Victims in Liberia
Dr. Richard Besser reports from Monrovia.

MONROVIA, Liberia — -- Matthew Lincoln died last night. He was one of two patients to die at the Bong County Ebola Treatment Unit on Saturday.
When Lincoln died, I was embedded with a group of aid workers tracking down Ebola patients. We were on our way to the center with his 23-year-old wife, Garmai and their 11-month-old son, Freeman, both of whom are believed to be infected with Ebola. We picked up Garmai and Freeman in the small village of Mahwa, but instead of traveling directly to the clinic, we detoured to pick up another suspected Ebola patient. A four-hour trip stretched to six, and by the time we reached our destination, Matthew was dead.
There was no chance for his wife to say goodbye.
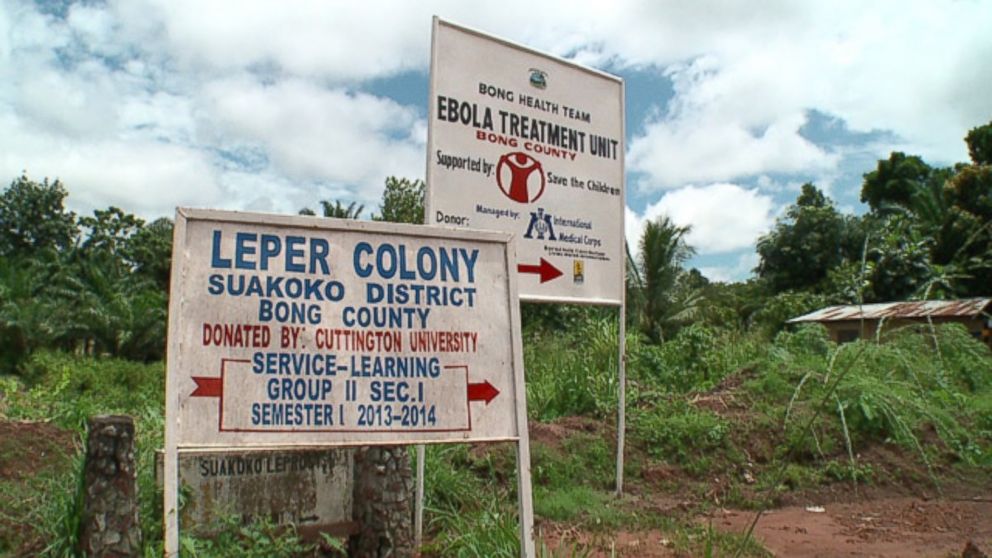
Bong County Ebola Treatment Unit is run by the International Medical Corps. It was built by Save the Children and is funded by USAID. It sits on top of a forested hill a couple miles from the main road on property that used to be a leper colony, according to a large sign that hangs by the road.
Eventually the facility will house 52 Ebola patients, but it opened just 13 days ago as part of the increased American support coming into Liberia to fight the outbreak. Now, it can only handle 22 patients.
Taking care of Ebola patients requires meticulous attention to detail; one small mistake and a health care worker can become infected. As a result, new centers scale up slowly, working out there systems with a small number of patients at first.
Chasing Ebola Patients in Liberia
Dr. Besser Chats With Relief Workers Headed to Ebola Hot Zone
Dr. Besser Gets Tips Before Heading to Ebola Hot Zone
This morning, we attended Matthew's funeral. No prayers, no remembrances, no loved ones at the grave site. There was just a small procession: the burial team, health care workers, and a small group from USAID.
A narrow trail snaked through the jungle leading from the treatment compound to the burial site. Vines hung down and tangled in our hair and roots tripped our feet as we followed the two yellow-suited members of the burial team carrying Matthew's body in a white body bag on an orange canvas stretcher. We filmed them from the front, walking backwards, slowing their progress with the body.
"Hurry, hurry," they said. "He's getting heavy."
We stepped aside to let them pass and filmed them from behind.
Seven mounds of freshly filled graves stood side-by-side, each with a little white sign bearing the carefully written name of the deceased. Stretching past these filled graves were 19 empty ones. It was a horrifying sight.
In the short time the treatment unit has been open, they've buried seven victims and have two more waiting to go into the ground. There were more empty graves than there were living patients being treated here for Ebola.

"We have to plan ahead," Dr. Pranav Shetty, director of the unit explained, adding that they have a team of nine gravediggers who can dig three graves a day. "It's important that they stay ahead of our needs."