Woman's blood literally turns blue from common pain medication
"I'm weak and I'm blue," the patient told the ER doctors.
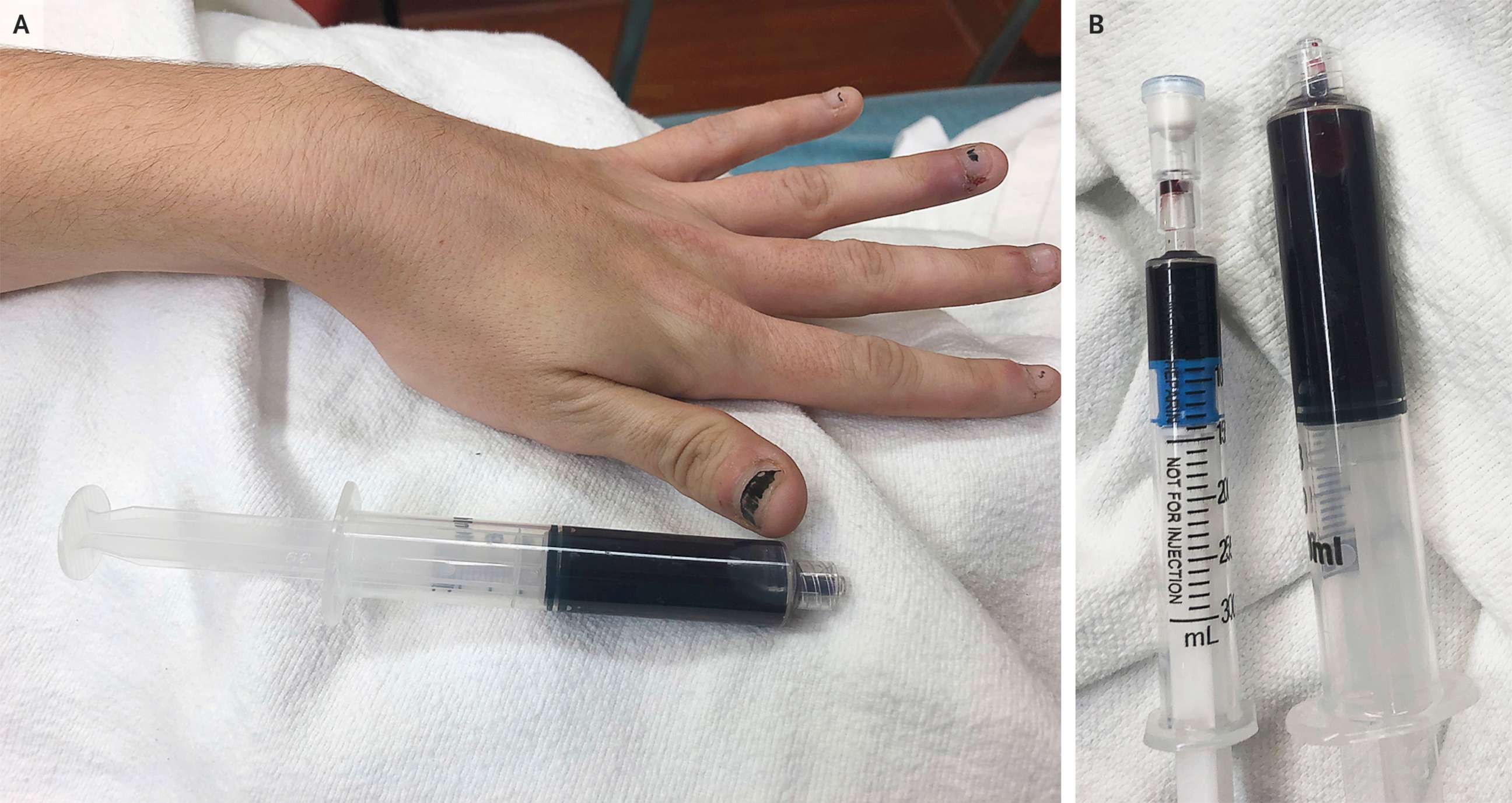
The term "blue blood" took on a new meaning for a 25-year-old woman who checked into a Rhode Island emergency room with complaints of fatigue and shortness of breath, as well as a more unusual symptom: her blood was turned navy blue.
The patient, whose account was documented in a New England Journal of Medicine case study, told doctors she had used an over-the-counter medication to treat a toothache.
"I'm weak and I'm blue," she told the ER doctors.
Dr. Otis Warren, the ER doctor on duty at Miriam hospital that night, diagnosed the woman with "acquired methemoglobinemia," a rare blood disorder in which the body isn't getting enough oxygen. While the disorder can sometimes be genetic, in the case of the Rhode Island patient it was triggered by taking large amounts of a medication containing benzocaine, a common ingredient in topical pain relievers and cough drops.
In 2018, the Food and Drug Administration issued a warning about benzocaine, advising that children younger than 2 should not take products that contained it. The agency also cautioned adults that benzocaine could cause methemoglobinemia, which can be "life-threatening and result in death."
There have been over 400 cases of benzocaine-related methemoglobinemia since 1971, according to the FDA.
After running tests, doctors found that the Rhode Island patient's hemoglobin and blood oxygen levels were low, which can put patients at risk for heart failure, coma or death. Doctors subsequently administered an antidote called methylene blue, which improved her breathing and bluish skin tone. By the time she left the hospital, her symptoms had completely subsided.




