‘They are terrified’: Fearing coronavirus, people with potentially fatal conditions avoid emergency care
Doctors say a crisis within a crisis is brewing as the sick stay home.
“Stay home.” That’s the message public health experts and political leaders have foisted onto Americans in recent weeks, and that was the message ringing in Alan Phenix’s mind when the pain crept into his abdomen earlier this month.
“We followed all the guidance very well and we were sheltering in place, basically isolated,” Phenix said of his Los Angeles-based family. “So there was this concern that by going to the hospital I would expose myself to the risk of infection.”
With an immunocompromised wife at home, Phenix, 62, waited five days after symptoms emerged before seeking treatment for what turned out to be appendicitis. By the time he received medical care, his appendix had ruptured and an infection had set in.
Weeks on, lingering stomach discomfort and an ongoing antibiotic regimen stand as a reminder of what should have been a simple surgical procedure if he had not hesitated to go to the hospital immediately. In hindsight, he said, fears of contracting the coronavirus, at least weighed against the pain he was experiencing, were exaggerated. A diligent UCLA Medical Center staff had taken “every reasonable caution” to prevent the spread, he said.
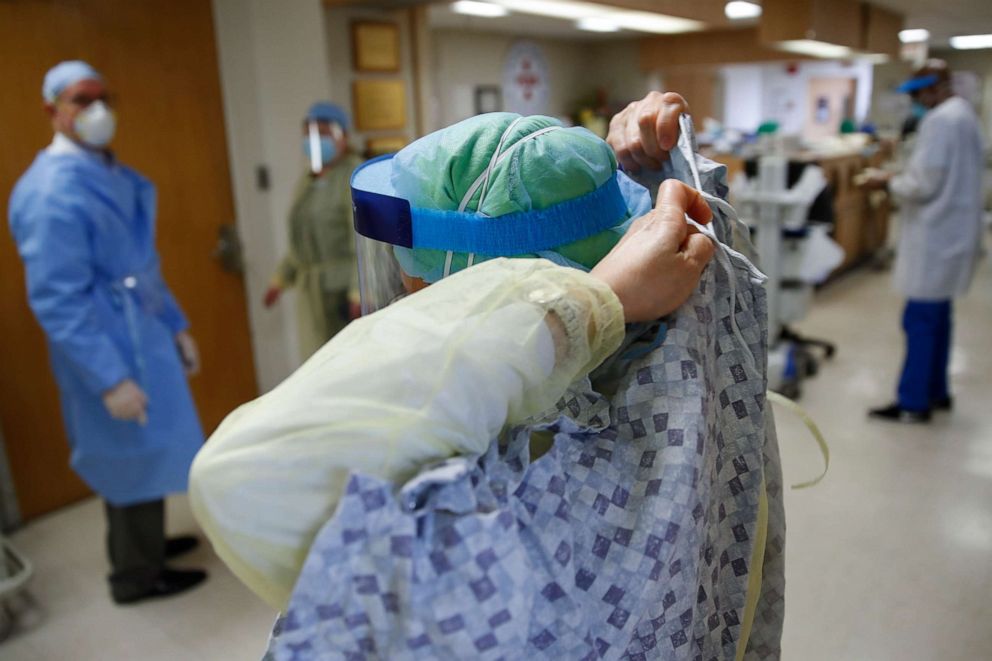
Medical professionals are sounding the alarm on what some have characterized as a silent storm brewing and a crisis within a crisis – patients with critical ailments and symptoms staying home for fear of going to an emergency room and contracting the coronavirus.
“What we’re seeing is people staying at home and hoping they get better instead of seeking treatment – and they’re dying,” said Dr. Eric Snyder, the medical director at Providence Cedars-Sinai Tarzana Medical Center in California.
One physician on the West Coast who asked to remain unidentified because he was not authorized to speak to the media lamented members of his own family hesitating to visit their doctor.
“I couldn’t even get my mother to seek care when experiencing serious symptoms -- and her fear of being exposed to coronavirus led to delay in being seen and a subsequent stroke," the physician said.
Phenix’s case serves as a cautionary tale – but countless others who hesitated to seek treatment have fared worse, some doctors suggest, leaving some in the medical community to wonder whether the “stay home” sentiment has actually endangered some who should seek emergency help.

Dr. Bill Jaquis, the president of the American College of Emergency Medicine, said Americans who pushed off visiting an emergency room because of the “stay home” messaging “have taken it too far.”
Jaquis suggested that emergency department visits in some part of the country are down by as much as 50%.
The novel coronavirus has now taken the lives of some 46,000 people in the United States, according to Johns Hopkins University. But the death toll for those who have stayed home despite showing symptoms remains unknown. Anecdotes from physicians on the front lines suggest that number could be staggering.
“Our hospital has had one COVID-related death,” Snyder said. “But I would estimate we have had at least 15 deaths not related to COVID that could have otherwise been preventable due to people staying home, medically isolating.”
The rate of emergency room visits per 100,000 people reached a 10-year high in 2015 for all age groups, but those patients aged 45-64 years had the largest increase.
In emergency rooms across the country and around the world, beds now filled with COVID-19 patients have left doctors wondering where patients with traditional medical emergencies – heart attacks, strokes, abdominal conditions, and bladder infections – are going.

"What we've seen over the course of the last six to eight weeks is that there are decreasing numbers of heart attacks and strokes showing up at U.S. hospitals,” said Dr. Robert Harrington, interventional cardiologist and president of the American Heart Association in a statement issued Wednesday. “That has also been reported in other places around the globe that have experienced Covid-19 epidemic.”
In Spain, one of Europe’s hardest hit countries, researchers have found that the number of heart attack patients treated in healthcare facilities has plummeted by 40% since the onset of the virus. A separate group of researchers in Hong Kong found something similar.
The crisis within a crisis is, like the coronavirus, also likely to disproportionately affect minorities, who already faced a disparity in care in parts of the country.
“Even before COVID-19, we knew there were patients we do not see, whether because of financial barriers, racism, fear related to immigration status, or social isolation," Dr. Dave Chokshi, a top heath officer and an internist at Bellevue hospital New York City, the city that is the current epicenter of the coronavirus crisis.
"But now, that is compounded by additional barriers to seeking care, which span physical and technological challenges as well as concern about becoming infected with COVID-19,” Chokshi added. “I am worried about hidden illness due to foregone care, and how this might contribute to a 'second wave' related to this pandemic.”
The biggest concern among some doctors from these two trends is that the damage from other illnesses can be irreversible. It is therefore crucial that patients identify key symptoms early and call 911 as soon as possible, regardless of the pandemic situation, doctors say.
“They are terrified … and it’s incredibly sad to watch my fellow residents sit at home and die slowly. As a medical professional it’s painful to watch,” said Snyder. “I’m here to care for them and they’re not giving me a chance.”
Jay Bhatt, a practicing internist and Aspen Health Innovators Fellow, is an ABC News contributor. ABC News contributor Dr. Vinayak Kumar contributed to this report.



