Dr. Phil's App Lets You Visit Your Doctor Virtually
Phil McGraw's "Doctor on Demand" app teams up with UnitedHealthcare insurer.
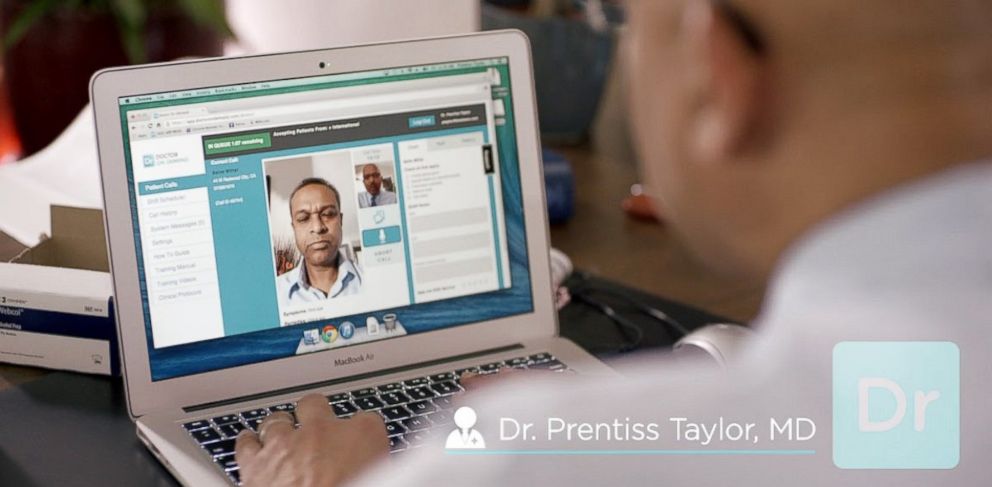
— -- Psychologist Phil McGraw from the television show "Dr. Phil" wants your next doctor visit to be as easy as ordering take-out on your smartphone. McGraw is backing a video-based app for virtual doctor visits that just got a major boost from a big health insurer.
Doctor on Demand, which recently raised $21 million, announced today that it is partnering with insurance provider UnitedHealthcare. The app connects patients with board-certified doctors, psychologists and lactation consultants 24 hours a day from a pool of about 11,000 professionals. McGraw, his son, Jay, and co-founder Adam Jackson started the company in 2012 in San Francisco.
McGraw said the app will let you bypass a lot of typical headaches when you need to see a doctor.
"You've got to get in your car, you might have to get your children covered with some kind of child care, you’ve got to take off work, you’ve got to drive down there -- that’s gas, parking, all of this," he said. "Or [with the app] ... you can get on your smart phone, your tablet or your laptop, your desktop, hit a button and, usually within about 30 seconds, you’re face to face with a board-certified physician."

The website lists conditions that Doctor on Demand doesn't treat, including cancer and chronic conditions.
"For more serious or chronic conditions, a visit to a doctor or hospital is important and necessary," the website states.
Arthur Caplan, head of NYU School of Medicine's Division of Medical Ethics, cautioned that telemed apps are useful, "but not a substitute for primary care visits."
"It isn't clear if they can protect your privacy, liability for errors is murky, and quality control over providers remains uncertain," Caplan told ABC News.
Dr. Seth Bokser, associate chief medical information officer for UCSF Benioff Children's Hospital, advises patients and families "whether it's through virtual technology or coming into clinic," not to see a different doctor every time an issue arises -- "but to engage in continuous and trusted relationships with their physicians and care team."
"With that said, most traditional providers would envy the app store reviews that some of these services get from users because patient convenience is such a vital and historically undervalued part of that patient-doctor relationship," Bokser said. "And from a system perspective, there is tremendous value associated with keeping otherwise healthy patients out of emergency rooms with minor complaints like pink eye or hives."
Bokser said UCSF Benioff Children's Hospital is using telehealth technology to extend existing relationships with known patients. For example, after an inpatient stay or clinic visit, patients and families in the hospital's pain and palliative care program have a virtual telemedicine appointment with a physician to manage symptoms and medications.
McGraw said the app has been described as a "disruptive force, which is apparently the highest praise," upending what can be a wait to see a doctor.
UnitedHealthcare is also partnering with two other telemedicine companies, NowClinic and American Well, to provide the service to their 45 million customers with health benefits.
Unlike other virtual doctor services that require a monthly subscription or another upfront cost, users only pay for Doctor on Demand when they are connected to a health care provider. The app is available for free in the Apple App Store and Google Play store for Android devices.
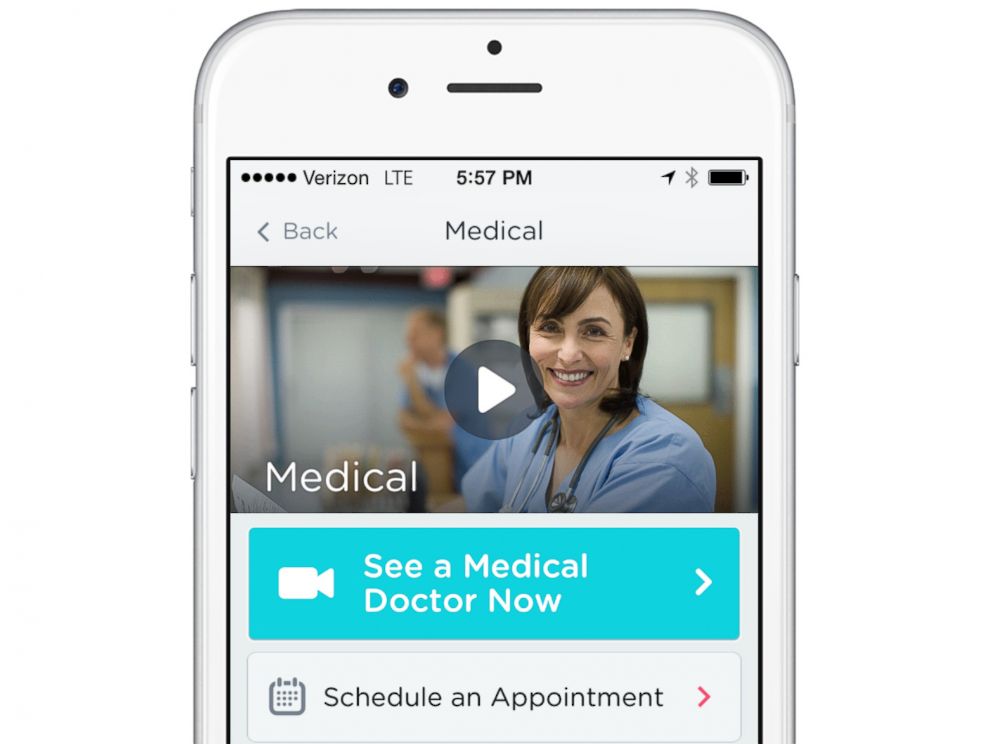
After users download the app, they provide a list of their symptoms then start their "video visit."
The cost of a video-based virtual visit starts at $40, which, according to UnitedHealthcare, is less than the price of minor medical needs treated at a doctor’s office visit ($80), urgent care visit ($160) or emergency-room visit ($650). The insurer said participants pay a portion of the visit cost, subject to deductibles, co-payments and out-of-pocket expenses based on their health plans. A session with a psychologist starts at $50 for 25 minutes while the same amount of time with a lactation consultant is $40.
"Over 80 percent of doctor visits end without hospitalization, which means you didn’t need to go, because you weren’t going to be hospitalized," McGraw said. "And most of those things can be handled with this virtual visit. And we have the ability for you to take a picture of your ear, or your throat, or your rash, or your finger, or your thumbs, and transmit it during the visit [to] where they can blow it up and take a look at it."