Woman celebrates 1st Mother's Day after giving birth while in coma due to COVID-19
Serena Torres, 29, spent more than four months in the hospital.
Serena Torres says she plans to celebrate Mother's Day this Sunday in a major way because she was not sure if she would live to see it.
Torres, 29, of New York, spent four months hospitalized with COVID-19, including two months in the intensive care unit, during which she experienced heart, lung and kidney failure.
A speech pathologist who works in a preschool for children with special needs, Torres was diagnosed with COVID-19 last October, when she was six months pregnant with her first child.
"It was a really scary and emotional point because there were so many unknowns," said Torres, who believes she contracted COVID-19 from her husband, who was exposed to the virus at his job. "At first I didn't think that COVID was going to hit me as hard as it did because I don't have a complicated medical history."
"I was 28 at the time. I worked out every day at the gym," she told "Good Morning America." "I didn't think I would be as affected as I was."
Torres was hospitalized for several days locally and then in mid-October was transferred to Westchester Medical Center, where she was kept alive first by a ventilator and then an extracorporeal membrane oxygenation, or ECMO, machine, which removes carbon dioxide from the blood and sends back blood with oxygen to the body, allowing the heart and lungs time to rest and heal.
"Serena was certainly among the sickest of the sick," said Dr. Dipak Chandy, chief of critical care medicine at Westchester Medical Center, and a member of Torres' care team. "By the end of October, her lungs had failed, her heart had failed and her kidneys had failed."
On Oct. 20, Torres was in such a deteriorating state that doctors performed an emergency cesarean section to deliver her baby, a girl named Alessandra.
Alessandra was born weighing just 4 pounds and spent one month in the hospital's neonatal intensive care unit because she was born premature. The newborn tested negative for COVID-19 at birth, but tested positive for antibodies, according to Torres and Chandy.
Torres was in a medically induced coma and being kept alive by an ECMO machine at the time of her daughter's birth.
"My health really declined after the C-section, so basically I had been staying alive for her," said Torres. "I don't remember this account but many nurses told me that there was one moment when I woke up from the sedation and I rocked my arm like I was trying to rock a baby, but I couldn't communicate. It was like I was asking, 'Where is my baby?'"
Torres said she was thankful she and her husband Jonathan had spoken briefly when she was first hospitalized about what to do if her health got worse.
"We spoke quickly to decide on a few names and we talked about what he'd do if he had to choose between seeing me or the baby," she said. "I told him to see her because I wanted my baby to know that someone was there for her, that someone who loved her was there, and I knew how important it was for the newborn-parent bond."
In early November, after many medical interventions, including continuous dialysis for kidney failure, Torres' health began to improve.
Around the same time that Alessandra was discharged from the NICU, Torres began to wake up from her coma, which she had been in for six weeks.
"I had muscle tremors and a lot of weakness and a paralyzed vocal cord so I couldn't speak," she said. "I would just hold up a shaky thumbs up to respond how I was doing."
One of the first things Torres asked doctors and nurses about was her baby. Too weak to hold a phone by herself. Torres relied on the help of nurses so that she could see her daughter on video calls.

Nurses also hung a laminated photo of Alessandra in Torres' room, and Jonathan made a photo album of Alessandra so his wife could see their daughter's first months that she missed.
"I kept the book in my room so I could remember that she was healthy and born," recalled Torres.
Once Torres recovered from the coma, she spent another nearly three months in the hospital regaining her strength and recovering from other complications, including blood clots that required all her toes to be amputated. During that time, she was still unable to see Alessandra in person because of COVID-19 restrictions.
"I longed to see her," said Torres. "I think that's what motivated me to fight. I couldn't see her so I was motivated to get better."
In mid-February, four months after giving birth, Torres was able to hold Alessandra for the first time.
"I will never forget that day in my life. I just started to do the ugly cry, when you're so happy that you don't even care," said Torres. "She just looked at me, holding my finger."
"You wait so long. Every single day you're fighting, fighting for that moment, and when that moment comes, you just can't explain it," she said. "I'm tearing up now thinking of the moment."
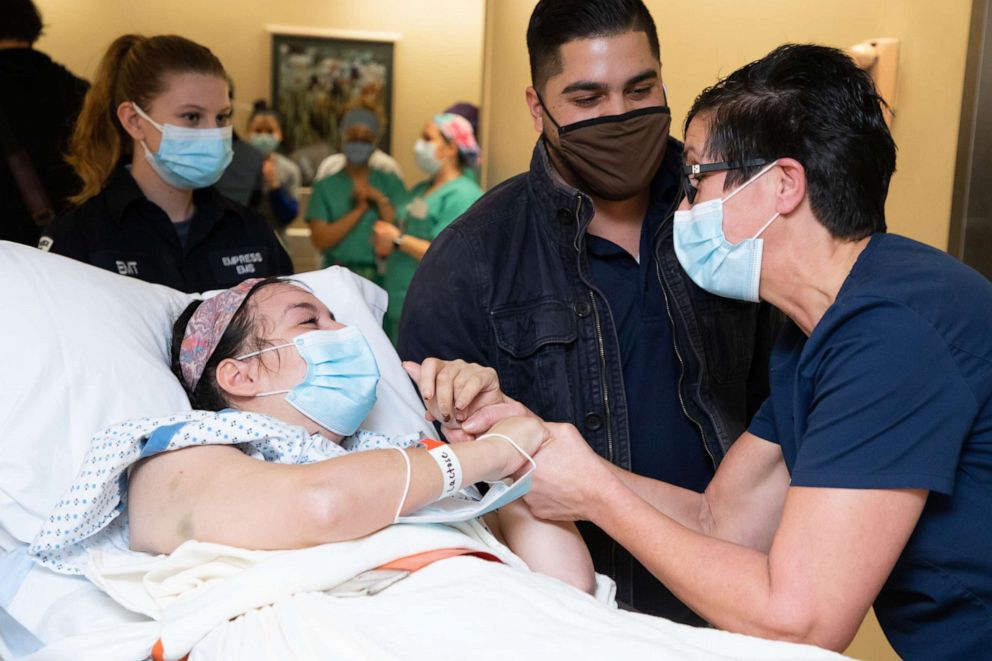
When Torres was discharged from the hospital in February, health care workers at Westchester Medical Center lined the hallways to bid her goodbye and celebrate her miraculous recovery.
"I cannot stress enough how much this means to the ICU team, seeing something like what happened to Serena," said Chandy. "For every person working in the ICU, it's stories like these that make it all somehow meaningful."

Though Torres is now home with her daughter and husband, she said she is still recovering from complications due to the virus.
She has continued neuropathy with weakness in her legs and arms, requiring someone be with her at all times to help with Alessandra. Torres also relies on a wheelchair and is undergoing therapy as she works to regain her balance and strength after her toe amputations.
She said she also has some lingering spinal and thyroid issues, along with the unknown nature of long-term COVID-19 complications, that make her grateful every day to be with Alessandra now.
"I see things differently now and I'm so grateful for every single day," said Torres. "I didn't get to celebrate Thanksgiving, Christmas and New Year's so we're going to celebrate this Mother's Day like it's all the holidays combined."
"But this [Mother's Day] to me feels like most important because, right now, Alessandra has a mom here and that means the world," she added. "I fought so hard to be a mom and to be here home with her."