Health care providers less likely to offer HPV vaccination to teenage boys, study suggests
Skipping the vaccine could potentially be putting them at risk of cancer.
A new study has revealed that health care providers may be failing to routinely offer the HPV vaccine to boys, potentially putting them at risk of cancer later in life.
Infection with human papillomavirus (HPV) is associated with cervical, vaginal, anal, mouth and throat cancers. The U.S. Centers for Disease Control and Prevention (CDC) recommends that all boys and girls aged 11 to 12 should receive the HPV vaccine to reduce this risk.
However, the most recent statistics from 2016 show that while around 65 percent of girls had started the vaccine course, only 56 percent of boys had.
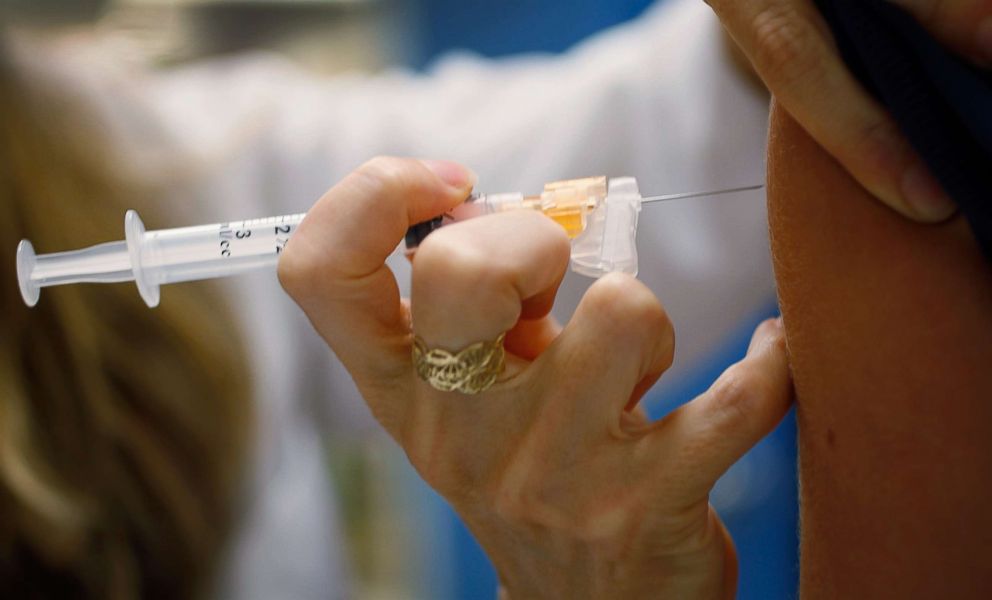
The study provides some insight into why. The researchers analyzed a national survey from 2015 that asked parents why their children didn’t receive the vaccine. In particular, they compared the reasons provided by parents of boys and girls to learn more about the gender difference in vaccination rates.
Parents of boys were more likely to suggest that their child had not been recommended the vaccine by health care providers. Almost 20 percent of boys' parents cited this reason compared to about 10 percent of girls' parents, suggesting health care providers are less likely to offer the vaccines to boys.
Among both genders, the most common reason for not starting vaccination was the belief that it wasn't necessary, as 21 percent of girls' parents and 22 percent of boys' parents said this.
Dr. Anna Beavis, one of the researchers who conducted the study, said it's "clear that physicians need to give a strong recommendation to both parents of boys and girls. They also need to remind parents of the importance of getting all doses, which makes the vaccine the most effective in preventing HPV."
In the United States, the HPV vaccine was approved by the FDA for use in girls in 2006 and boys in 2009. In Australia, which has vaccination rates of 78.6% for 15-year old girls and 72.9% for 15-year old boys, the vaccine has been linked to a decline in the rates of HPV diagnoses.
These findings were presented at an Annual Meeting of the Society of Gynecologic Oncology in New Orleans on March 24. The data was taken from NIS-Teen, a national survey which collects data from parents of adolescents aged 13 to 17 years old in order to track vaccination rates in the United States.
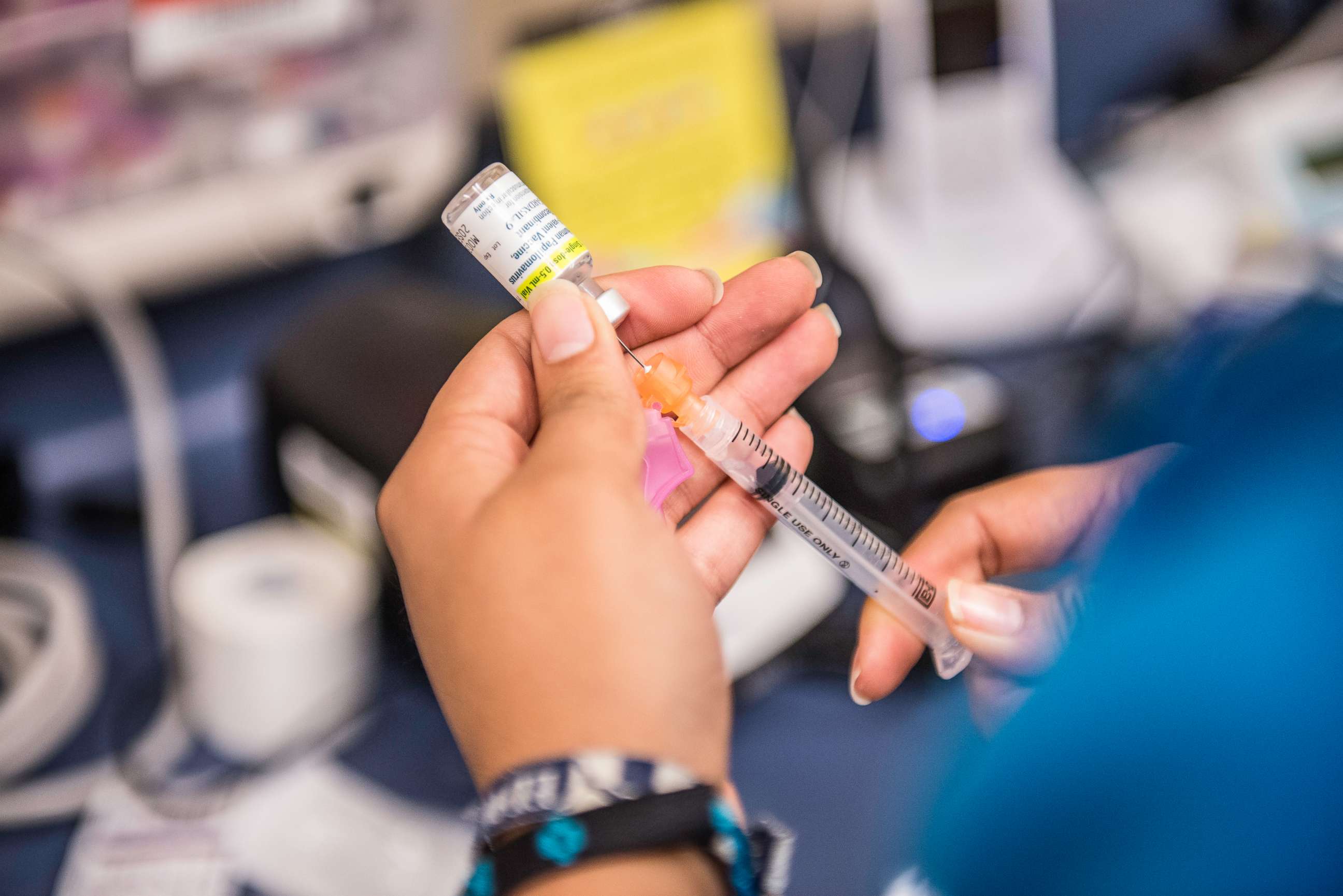
Answers to common questions about the HPV vaccine:
How common is HPV?
The CDC estimates that HPV is so common that "nearly all men and women will get at least one type of HPV at some point in their lives." Approximately 14 million people in the United States become newly infected each year.
Why is the vaccine recommended for both boys and girls?
While the virus often resolves without symptoms, in some cases it can cause a number of different cancers in later life, including cervical, vaginal, anal, mouth and throat cancers.
How is HPV transmitted?
HPV is usually transmitted via intimate sexual contact and most people don't know when they’ve become infected. Less commonly, it can be transmitted from a mother to their baby during childbirth.
What does the HPV vaccine involve?
If started before the age of 15, the vaccine can be given in a course of two doses, at least six months apart. For individuals older than 15, three doses are recommended. The vaccine is administered as an injection.
Is the vaccine safe?
According to the National Cancer Institute, no serious adverse effects have been shown to result from the vaccine to date. Mild side effects include soreness at the injection site, which is also commonly experienced with other vaccines.
Should older children and adults receive the vaccine?
The HPV vaccine is recommended for young women up until the age of 26, and young men until the age of 21, or 26 if they identify as gay or bisexual.




