Children of color disproportionately impacted by severe COVID-19 and related illness, data reveals
Racial disparities in COVID-19 also extend to children.
Since the onset of the coronavirus pandemic, the nation's health inequalities have become even more glaring, with millions of Americans of color, Black and Latino in particular, experiencing more severe illness and death due to COVID-19 than white Americans.
New data now reveals that the same racial and ethnic disparities which have affected adults throughout the pandemic, also extend to children of color. Black and Latino children have been affected by more COVID-19 related illness and death than other children.
More than 3.1 million children have tested positive for coronavirus since the onset of the pandemic, accounting for approximately 13.1% of all cases in states reporting cases by age, according to a weekly report from the American Academy of Pediatrics and the Children's Hospital Association.
At this time, severe illness due to COVID-19 remains rare among children. Between 0.1%-2.2% of all child COVID-19 cases have resulted in hospitalization, and children currently account for 0.00%-0.4% of all COVID-19 deaths.
The rate of coronavirus cases among children roughly matches with their demographics in this country. According to the Annie E. Casey Foundation, about 25% of children in the U.S. are Hispanic or Latino, and 14% Black or African American. In children between the ages of 0 and 17, Latino children represent nearly 30% of cases, and Black, non-Hispanic children, represent 12.6% of cases according to the CDC.
However, when it comes to severe illness and deaths from the virus, children of color bear a disproportionate burden. Several studies -- and the CDC's database -- reveal that Black and Hispanic children are more likely to die of the disease.
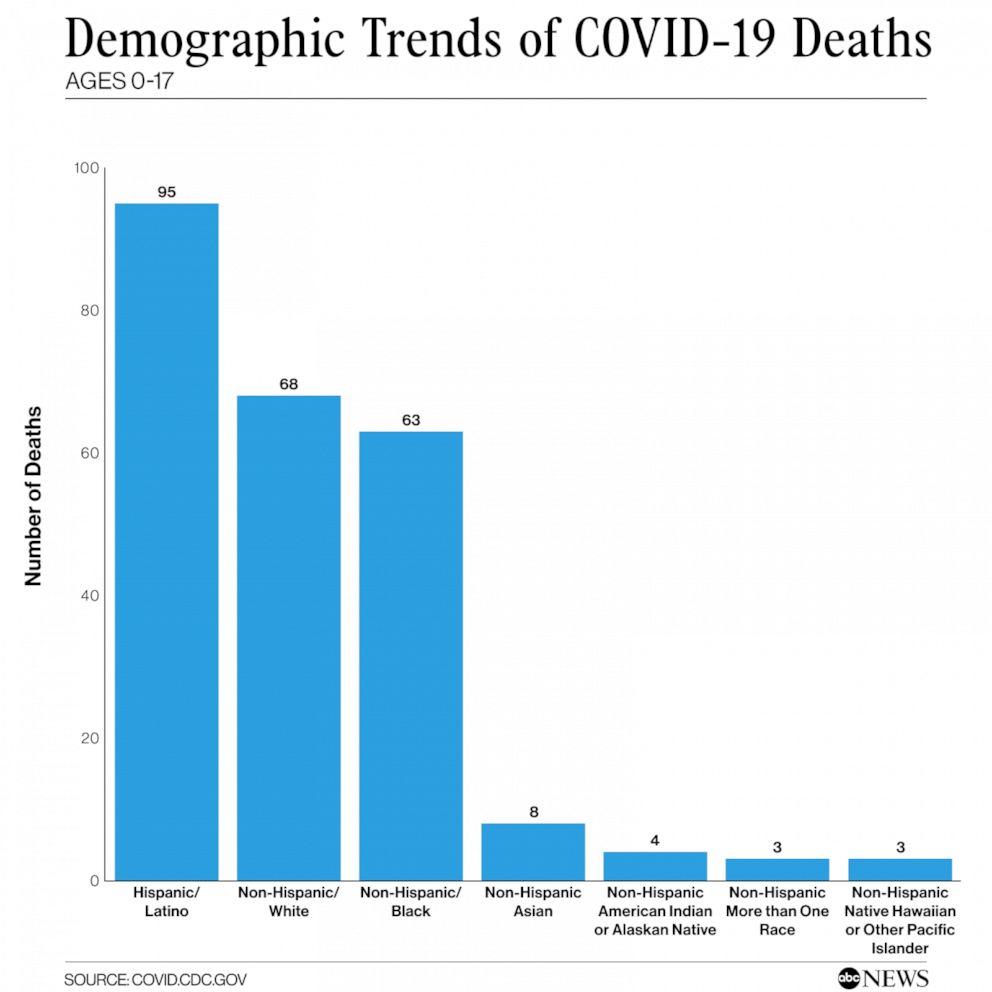
Overall, at least 244 children have died of COVID-19, according to the CDC. Latino and Black children currently represent approximately 65% of these deaths, according to CDC data.
Additionally, children of color are more likely to experience a severe COVID-related inflammatory illness called MIS-C. So far, 2,060 U.S. children have been diagnosed with MIS-C. The rare and extreme immune system response is linked to COVID-19, with 30 MIS-C pediatric deaths through Feb. 8, according to the C.D.C.
And at least 69% of reported MIS-C cases have occurred in children who are Hispanic or Latino or Black, non-Hispanic.
A recent study by Yale researchers, published in the Journal of Pediatrics, also found that the majority of pediatric patients, ages 1-17, who were hospitalized with SARS-CoV-2 infection or MIS-C, were Hispanic (51%) or non-Hispanic Black (23%).
"These data clearly highlight that the incredible disparities we have witnessed throughout this pandemic are consistent across all age groups," said Dr. John Brownstein, chief innovation officer at Boston Children's Hospital and an ABC News contributor. "The impact of COVID in pediatric populations mirror racial disparities in the adult population, with both cases and deaths seen more frequently among Black and Latino children." That includes both severe illness and death happening more frequently in black and Latino children says Brownstein.
A wide range of factors may be driving the racial-ethnic disparities in COVID-19 impact among children.
The majority of cases in children of color come from exposure to the virus within their household or their communities, according to Dr. Kristin Moffitt, an infectious disease specialist at Boston Children's Hospital.
Thus, "the disproportionately high case rates in Black and Latino children largely reflect how the adults in their lives have been impacted. Affected families are more likely to include essential workers who have had to risk exposures in order to do their jobs. They are also more likely to live in multigenerational homes or more crowded conditions that make distancing or isolating difficult," Moffitt told ABC News.
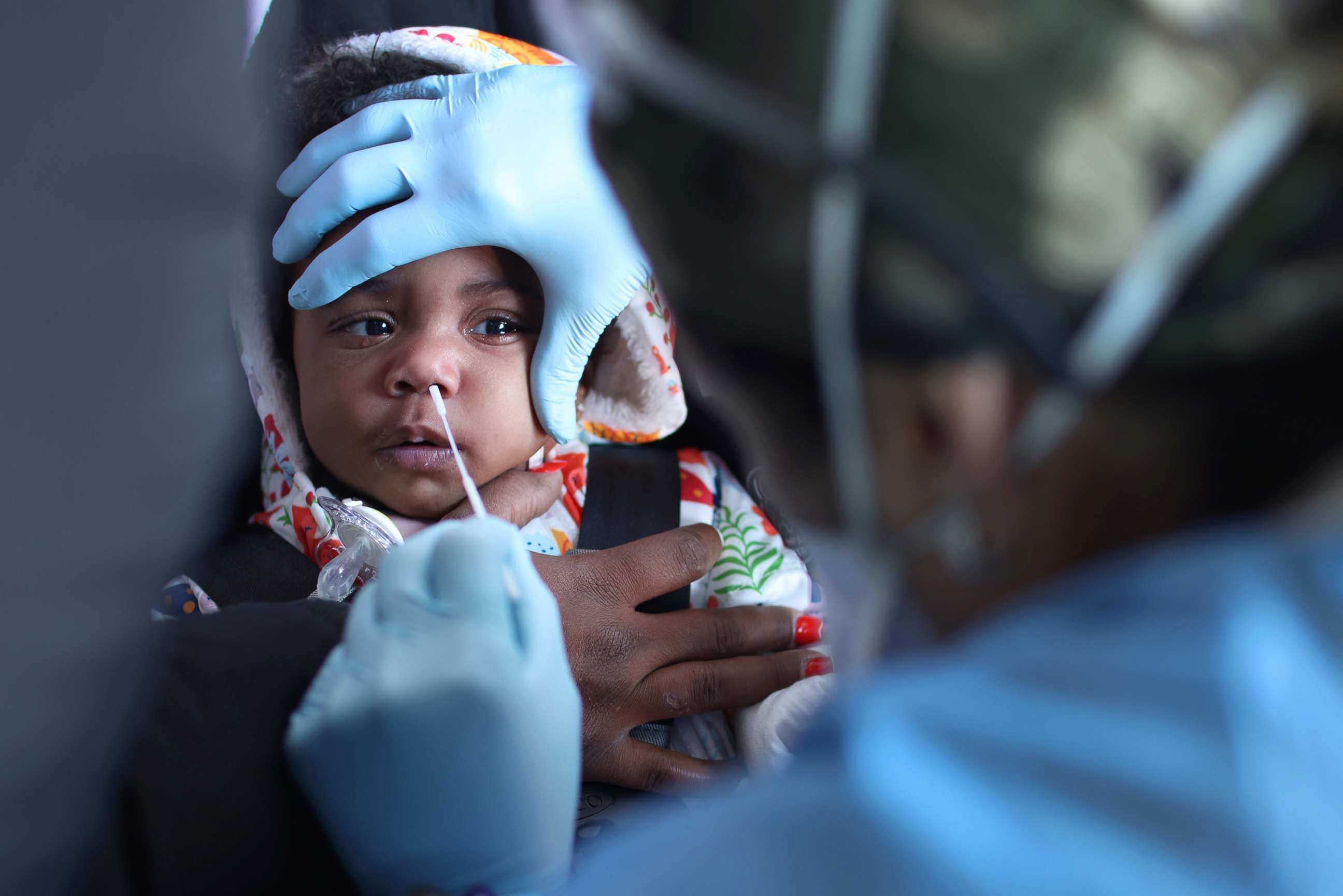
Further, communities of color are more likely to experience barriers to high-quality health care and testing, or to face cultural or language challenges in having access to this health care, experts say.
Underlying chronic health conditions that occur in minority youths can worsen the course of COVID-19 infection, added Brownstein.
Experts are still struggling to understand the extent of this problem, with race data only available for 74% of the country's confirmed COVID-19-related deaths, and 52% of the U.S.' coronavirus-related cases.
"We have a lot of work to do in reducing health disparities across a number of factors; these include race (and) ethnicity, but also geographic factor(s), rural versus urban, access to medical care, and socioeconomic status," said C. Buddy Creech, director of the Vanderbilt Vaccine Research Program and associate professor of pediatric infectious diseases.
"While these descriptive data help highlight uneven COVID burden on certain populations, significant work remains to determine how race, ethnicity and underlying socioeconomic status play into the trends we are seeing in children," Brownstein added.
Although 71,000 child COVID-19 cases were reported last week, this week marked the fifth consecutive week of declining new cases for children, reflecting the overall national decline in COVID-19 cases.
However, both American Academy of Pediatrics and the Children's Hospital Association warn that there is an urgent need to collect more data on longer-term impacts of the pandemic on children, including ways that the virus may harm the long-term physical health of infected children, as well as its emotional and mental health effects.
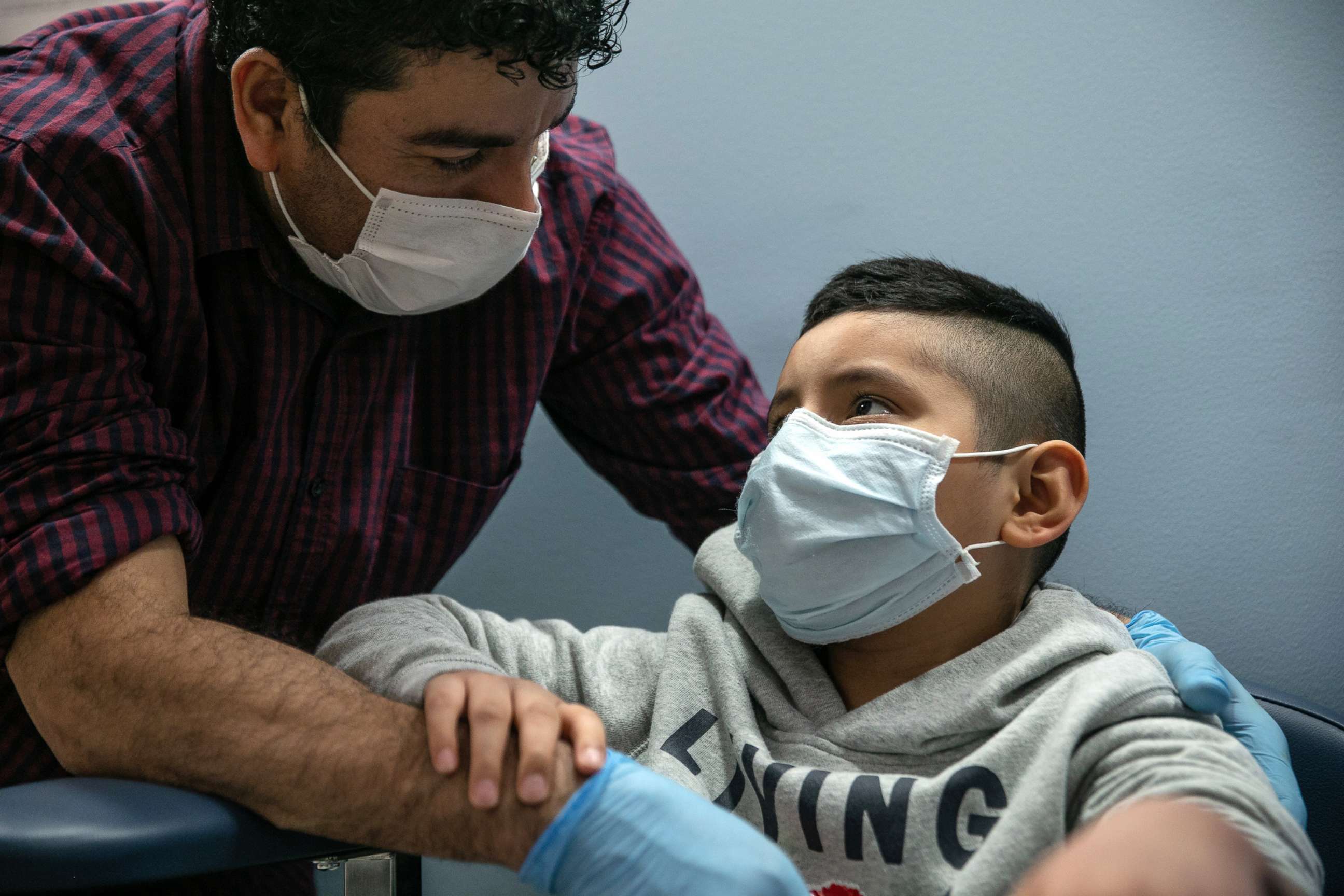
Experts are also reporting that it is increasingly urgent to authorize a COVID-19 vaccine for children, in an effort to curb the infection rate.
"If you wipe out the infection in the younger children, they don't spread it to the adults, and so then, you can get a big handle on disease just by targeting the younger children and getting the infection out of that age group," Dr. Robert Frenck, lead investigator of the COVID-19 vaccine trials at Cincinnati Children's Hospital, explained during a briefing earlier this month.
According to White House chief medical adviser Dr. Anthony Fauci, children as young as 6 years old are expected to participate in coronavirus vaccine trials this year, in an effort to have vaccines ready for some age groups by the time school starts in September.
However, experts remain deeply concerned by the racial and socioeconomic differences among children affected by the pandemic, and its consequences for the future.
"So many of the factors driving these disparities are the result of chronic inequities in the determinants of health such as access to secure income, housing, education and health care. There is cause for serious concern that the disproportionate impacts of this pandemic on minority communities will only widen these gaps," Moffit said. "Equitable vaccine distribution, improvements in health care access, funding of public schools in these communities to allow safe return to in-class learning will all help to narrow this gap."
This story has been updated to clarify that children of color disproportionately suffer from severe illness and deaths, rather than a disproportionate number of cases. The story has also been updated to reflect the latest statistics provided by the Centers for Disease Control and Prevention.
Editor's Note: This story has been updated to clarify that children of color disproportionately suffer from severe illness and deaths, according to a Yale University study and data from the Centers for Disease Control, rather than a disproportionate number of cases. The story has also been updated to reflect the latest statistics also provided by the CDC.




