The COVID-19 effects hospitals didn't foresee: Financial distress
U.S. hospitals with at least 100 beds are losing billions of dollars.
Dr. Bill O'Callahan, an emergency physician, rested his elbows on his desk, his head in his hands.
Despite his whirlwind thoughts -- a recent COVID-19 patient with failing lungs, a 30% pay cut, the dangers he faced on a daily basis -- he still counted himself among the fortunate. He was healthy, and he still had a job -- for now.
A staggering number of hospital employees have been laid off or furloughed -- sent home without pay, waiting to hear whether they can return to work. Now, a fresh look at what lies ahead for hospitals post-pandemic reveals some may not recover from a COVID-19 patient surge that never came.
Toward the beginning of the pandemic, initial worries included health systems being overwhelmed. But for most hospitals, novel coronavirus-related admissions have been more than offset by declines in unexpected areas. While fewer outpatient services and elective surgeries were expected, few hospitals anticipated steep declines in emergency room visits and in-hospital stays.

With the exceptions of New York and San Francisco, almost every other U.S. hospital has experienced unforeseen declines in patient volume. From March 1 to April 15, health systems in the U S. saw average declines in emergency visits and in-hospital stays of approximately 30% to 50%.
O'Callahan, who works just outside of Boston, said the volume of patients at his hospital dropped dramatically since the start of the pandemic, jeopardizing the hospital's revenue stream. Rather than furloughing staff, his hospital cut hours, cut salaries and ended retirement contributions.
"We did this to avoid letting anyone go, as our volume dropped to just over 50% of our typical volume," he said.
Hospitals across the country have been hemorrhaging money. According to a study by Crowe LLP that included data from about 1,500 hospitals and 100,000 physicians, U.S. hospitals were losing a combined $1.44 billion every day.
Recent data from the U.S. Bureau of Labor Statistics shows that even with so many in health care working tirelessly to combat COVID-19, job losses in health care are second only to the leisure and hospitality sector. U.S. unemployment numbers because of the pandemic now rival those of the Great Depression.
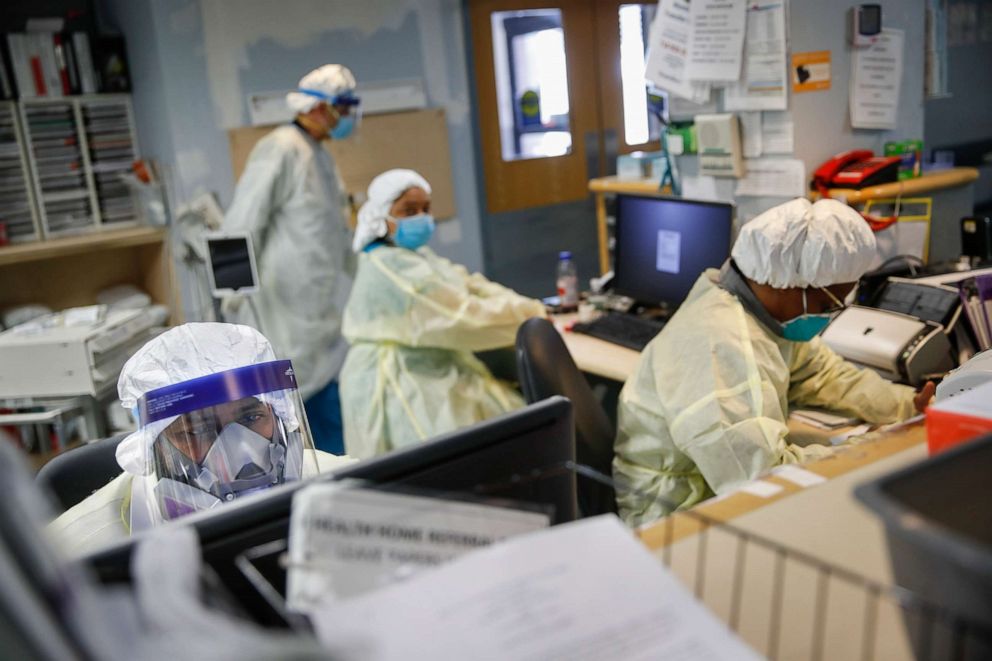
With millions of Americans losing their jobs, they're losing their health care. Self-payers have increased 8.4%, and hospitals are bracing for more lost revenue as bad debts and charity write-offs increase.
Many hospitals have received government bailouts, but Michigan Hospital Association spokesperson Ruthanne Sudderth said it's hardly enough. Last month, two of Michigan's largest health systems, Beaumont Health and Henry Ford Health System, announced they would lay off thousands.
"The CARES Act funding and some state funding we've received have been very helpful and timely, but it's kind of a drop in the bucket," Sudderth said, referring to the $100 billion in federal stimulus money allocated for hospitals. With such a drastic drop in revenue the current situation is "a huge financial strain on hospitals of all sizes."
Some frustrated Americans have pointed fingers at CEOs and health system leadership for the devastating job cuts, but health care analyst Seth Denson said it's really just "basic economics."
"When it comes to the layoffs and furloughs of health care employees, it's easy to point fingers at the 'villainous' hospitals," he said. "But with no money, comes no paycheck. With no paycheck, comes no staff. And even if you can keep the staff, with no money, comes no supplies."
The economic issues may be basic. The solution will be anything but.
Although each hospital will need a unique solution, the analysis by Crowe showed that an average hospital would need to run at 110% capacity for six months to recover -- a seemingly impossible feat.
Furloughed health care employees probably won't return all at once, and many may not return for a very long time -- or at all. Those fortunate enough to keep their jobs but at lower salaries may not return to their previous wages anytime soon.
Outside of Boston, O'Callahan said he's now the sole breadwinner in his family. His wife, also a physician, was furloughed weeks ago.
Nancy A. Anoruo, M.D., M.P.H., an internal medicine resident with a focus on public health at the University of Massachusetts, is a contributor to the ABC News Medical Unit. ABC News' Soo Rin Kim and Dr. Heather Kagan contributed to this report.




