COVID-19 vaccine may be less effective in obese people, experts warn
Vaccines have a history of performing poorly in those who are overweight.
As the world waits for a COVID-19 vaccine, concerns are already rising that it may not work in obese patients, arguably one of the groups that needs it most.
More than 1 in 3 Americans is obese, and the Centers for Disease Control and Prevention has said that obese people are among the groups more likely to get sick and die of COVID-19.
"We know from other vaccines that have been tested in obese populations that these individuals don't respond as well to these vaccines," said Dr. Matthew B. Laurens, a lead investigator at the University of Maryland School of Medicine for one of the United States' most advanced coronavirus vaccine trials by Moderna Therapeutics.
Research has long shown that vaccines against viruses like influenza and hepatitis B, as well as other disease-causing organisms like tetanus and rabies, are not as effective in obese adults compared to their thinner peers.
Evidence of this phenomenon goes as far back as 1985, when hundreds of hospital employees in North Carolina were vaccinated against hepatitis B and then studied to see how their immune systems responded. Researchers found that the vaccine was twice as likely to fail -- meaning it did not provide adequate protection against hepatitis B -- in employees with a higher body mass index compared to their colleagues with lower BMIs.
In 2017, researchers at the University of North Carolina, Chapel Hill reported similar findings in patients getting their yearly flu shot. In their study of over 1,000 participants, they found that obese adults were twice as likely to develop influenza or an influenza-like illness -- despite having been vaccinated against the virus -- compared to non-obese adults.
With 42.4% of the American population being classified as obese, and research identifying obesity as a major risk factor for COVID-19 infection and severe complications from the disease, this is giving some experts reason for pause.
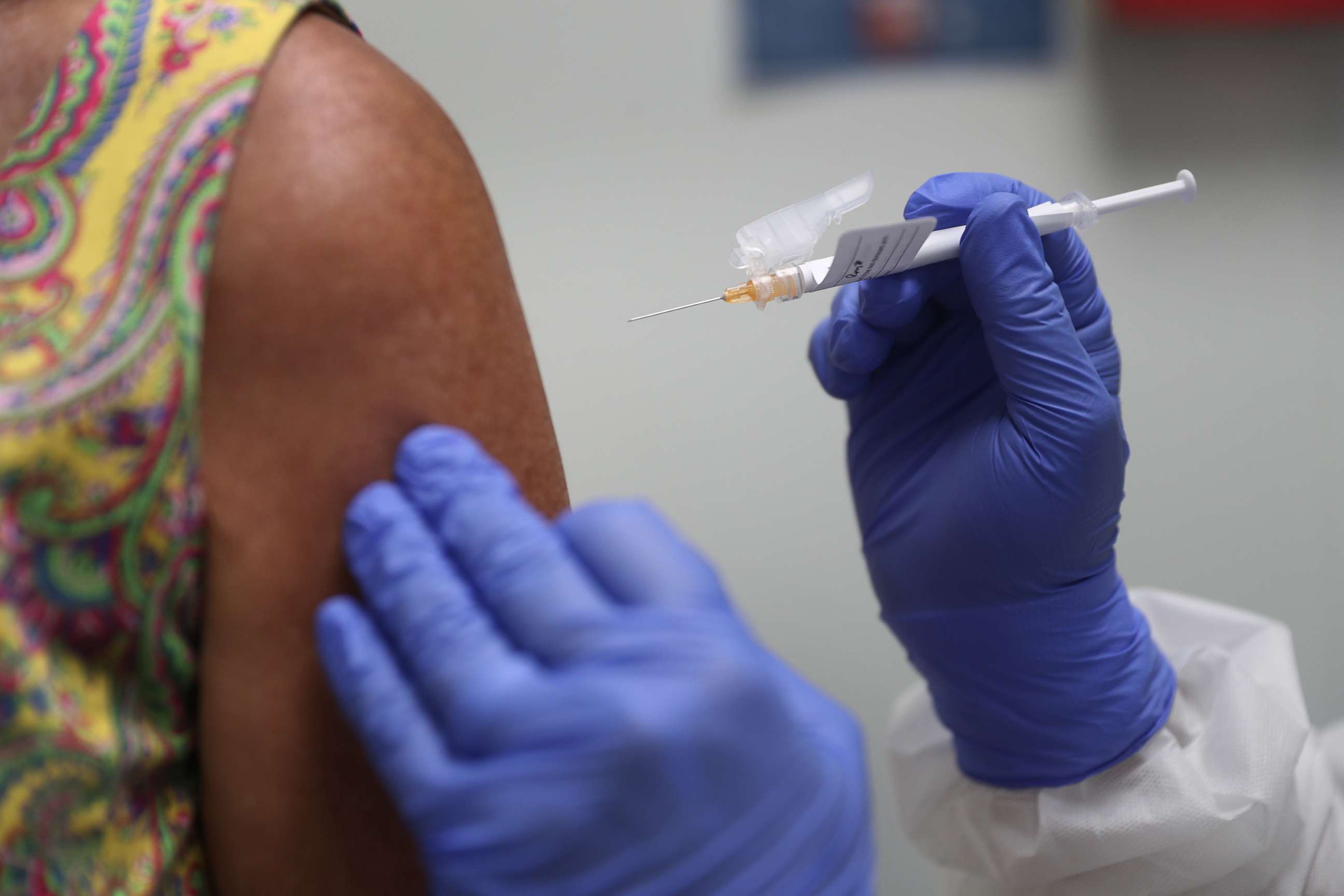
"We recognize that while we're developing a vaccine for COVID-19, it might not work in all populations, including those who are obese. So that's a concern," said Laurens.
It's not entirely clear to experts why vaccines don't seem to work as well in obese patients, but there are a number of theories.
One thought is that the typical one-inch needle routinely used for immunizations is not long enough for use in obese adults. This is because the fat layer under the skin may be thick enough that the needle can't reach the underlying shoulder muscle, where the vaccine liquid needs to be deposited to have its best shot at working.
Another theory is that obese adults, because of their increased body mass, may actually need a bigger dose -- or even a booster dose -- of the vaccine to properly ready their immune system to fight off the virus.
A third theory has to do with how obese patients' immune systems work.
According to Dr. Leonard Friedland, the vice president and director of Scientific Affairs and Public Health for GlaxoSmithKline Vaccines, "Obesity triggers a chronic inflammatory state in humans." This constant, low-level inflammation could be what's blocking some vaccines from working as well as they do in thinner patients.
"It's a real issue," said Friedland.
But could the coronavirus vaccine be different and provide equal protection for both the obese and the non-obese?
"We don't know. I think you could say it's possible. The new technology is different," said Laurens, referring to the novel mRNA technology being used in the coronavirus vaccine trial he's currently spearheading.
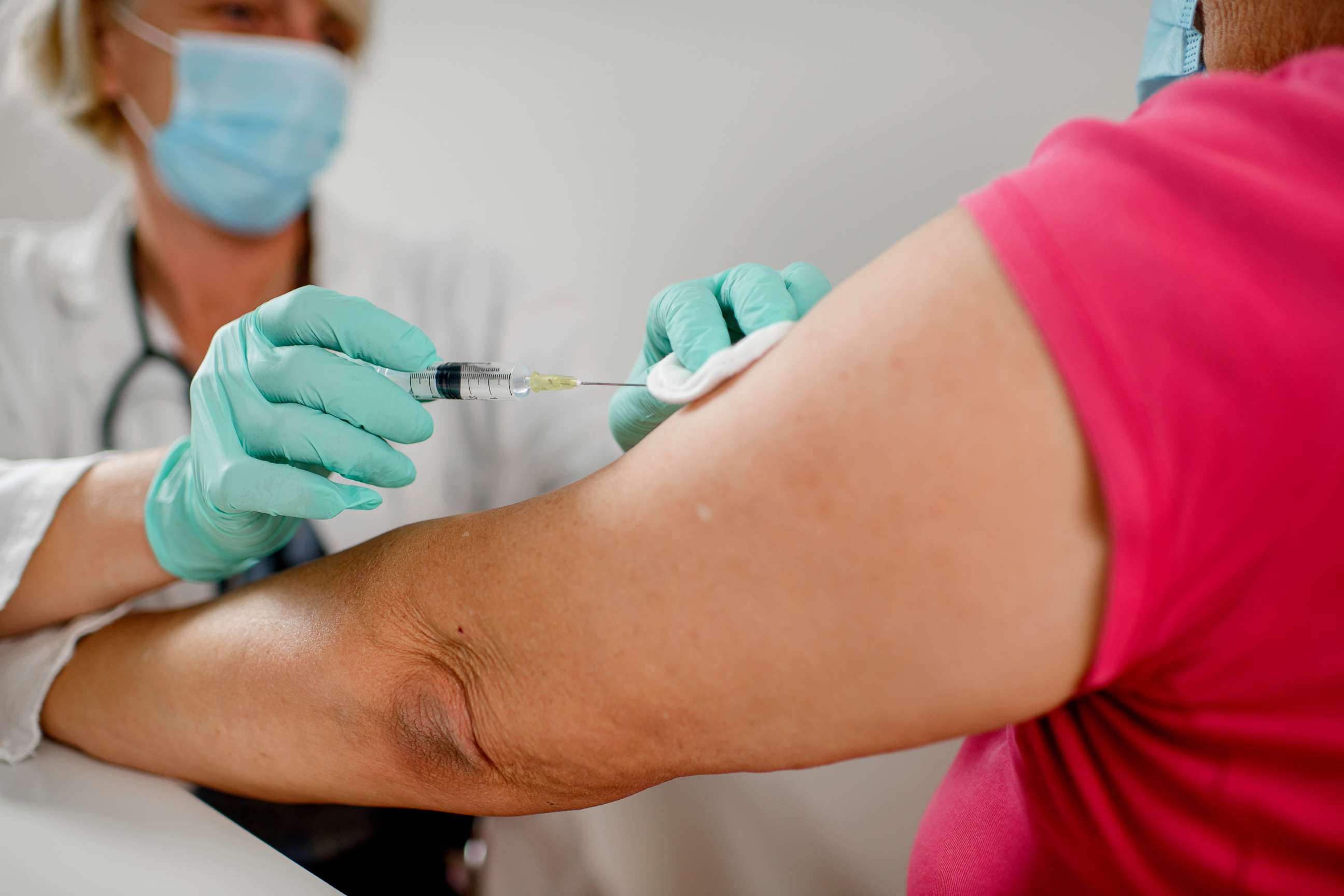
For now, perhaps the only way to know for sure whether the vaccine will work in the obese is to include them in large phase 3 trials -- the last step before authorization from the Food and Drug Administration.
"It's important to enroll obese people, because they are likely to have associated chronic illnesses, and you really get to see if the vaccine helps those highly at-risk people," said Dr. Arthur L. Caplan, the Drs. William F. and Virginia Connolly Mitty professor of bioethics at the New York University Langone Medical Center.
Historically, obese people have been largely excluded from vaccine trials, because of these chronic illnesses, like diabetes and high blood pressure.
Coronavirus vaccine developers, however, are now attempting to combat this disparity by actively enrolling obese patients in their clinical trials.
"We think it's important to develop a vaccine that is going to work for everyone," said Laurens. "That's why we're trying to be as inclusive as possible in the phase 3 studies -- so that we can learn more about how to protect particularly the vulnerable populations, including the obese."
Nate Wood, M.D., is an internal medicine/primary care resident at Yale New Haven Hospital and a contributor to the ABC News Medical Unit.




