'COVID Toes': Could skin conditions offer coronavirus clues?
Doctors report frostbite-like skin issues with some positive patients.
Months after the novel coronavirus appeared on the world stage, the deadly disease is still prompting medical mysteries, and doctors have identified another odd potential symptom: skin problems.
A growing number of prominent dermatologists treating suspected and confirmed coronavirus-positive patients are reporting patterns and trends of skin conditions, suggesting the skin could be a kind of window about what may be happening with COVID-19 inside the body.
Italian doctors published a series of cases signaling a trend about the skin in late March. In that study, one in five patients had a skin issue, most commonly a red rash or a hive-like eruption.
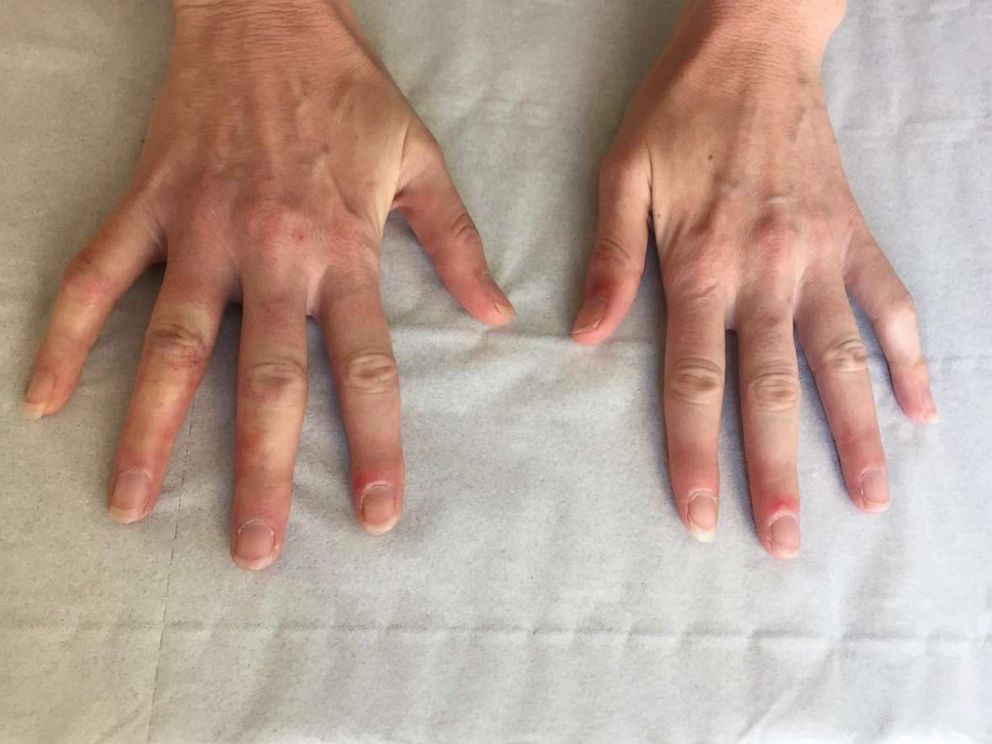
Dubbed “COVID toes” by the dermatology community, frostbite-like areas of typically red or purple discoloration can appear on the feet can also be seen on the fingers as well, according to Dr. Misha Rosenbach, associate professor of Dermatology at the Hospital of the University of Pennsylvania. But the discoloration doesn't appear to have anything to do with the weather.
“What we are seeing tends to be in response to the cold, but we’re seeing it in the middle of spring,” Dr. Amy Paller, chair of dermatology at Northwestern University told ABC News. “And it’s happening in such numbers as is COVID that we have to think there’s a connection.”
Rosenbach said these findings so far have been reported to be seen more in kids and young adults, which is a population that can be asymptomatic or have mild symptoms more frequently than older individuals, though more cases would have to be examined to determine which population is affected by this condition.
There have also been reported cases of skin conditions such as measles-like rashes or hives associated with COVID-19. But, complicating matters, these kinds of rashes are also commonly seen with reactions to medications or in other viral infections.
Rosenbach said because these are indeed common rashes, “there doesn’t seem to be a helpful pattern," meaning it’s harder for doctors to tell whether coronavirus or a more mundane issue is to blame.
Symptoms more commonly associated with coronavirus include fevers, upper respiratory problems like coughing, and fatigue. But more unusual symptoms have been seen in some cases, such as a lost of taste, kidney issues and blood clotting. Experts suggested the blood clotting could be related to the skin issues.
Besides “COVID toes," Rosenbach says dermatologists should be paying attention to a particular skin pattern called livedo reticularis, seen in some hospitalized COVID-19 patients. This appears as a purplish net-like discoloration of the skin and it is often a result of blood clotting abnormalities.
Dr. Joanna Harp, a dermatologist at Weill Cornell Medicine who is on the front lines seeing critically ill coronavirus patients, has seen patients develop such skin conditions, including a pattern of lacy, dusky rashes, some with death of skin cells, on the arms, legs, and buttocks, which are associated with a heightened clotting tendency that some people with COVID-19 develop.
“It is not yet known what causes the clotting tendency in these patients but there is some suggestion that the virus may over-stimulate the immune system in certain patients,” Harp said. “And this overzealous immune response could somehow trigger a downstream clotting tendency."
Last week, to help further define COVID-19 skin findings, the American Academy of Dermatology COVID-19 task force announced an online registry for health care providers around the world to report suspected COVID-19 skin findings.
Dr. Esther Freeman, a dermatologist at Massachusetts General Hospital and a member of the COVID-19 task force which started collecting skin condition cases associated with the coronavirus, said so far about 130 cases have been submitted to the registry.
But one of the biggest challenges for dermatologists is confirming an association between COVID-19 and skin findings is the lack of widespread coronavirus testing.
To know whether the skin signs are part of the active phase of the disease or a late sign, dermatologists believe testing patients with frostbite-like skin lesions is crucial in linking it to the disease.
“It's very hard now when we're short in the field of testing and to get people who are having this but nothing else-- they don’t meet the criteria for COVID-19 testing to be COVID-tested,” Paller said.




