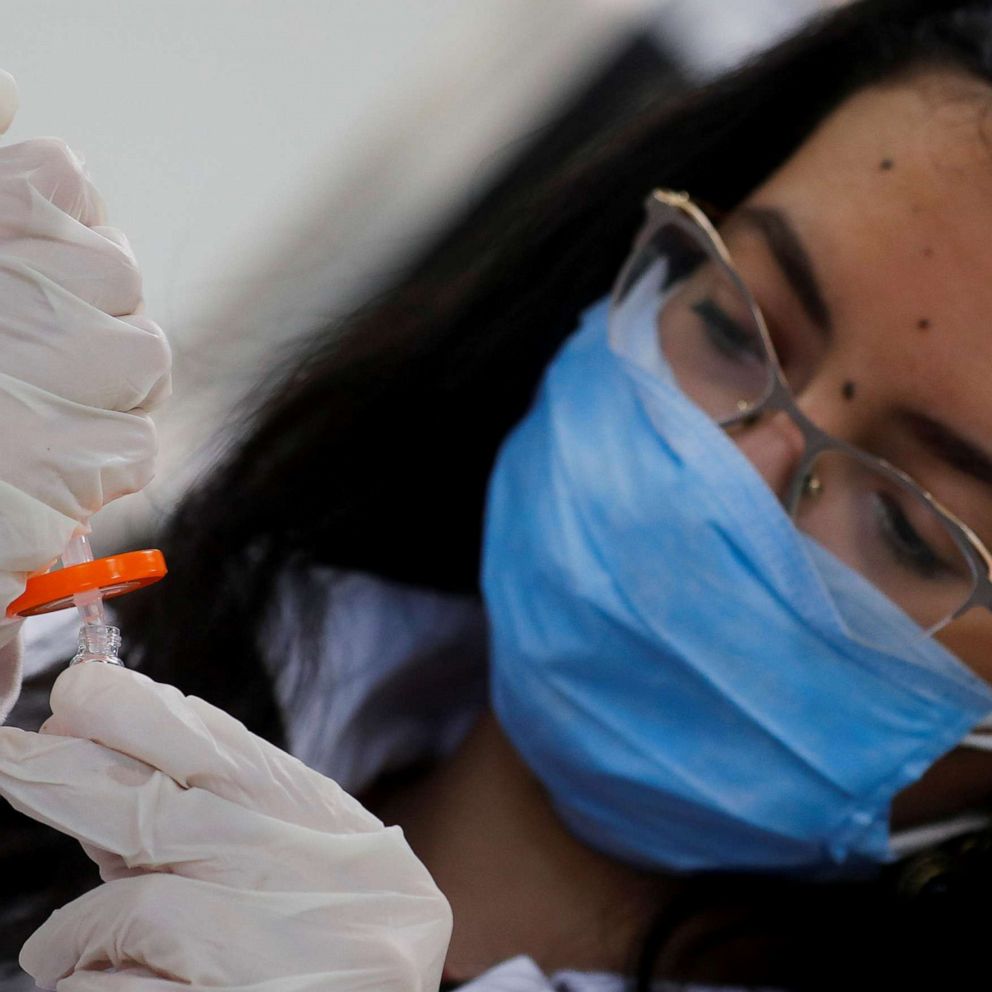
Doctors working to crack the mystery of 'long haul' COVID-19 sufferers
Experts are seeing persistent symptoms in some people recovering from COVID-19.
Lisa Fitzgerald and her husband Chip came down with COVID-19 at around the same time. Both experienced those telltale symptoms like shortness of breath and fatigue, and both tested positive for the virus in July. But even as Chip began to recover from the illness, Lisa experienced persistent symptoms.
Her fatigue got worse, and she even started to lose her hair.
"My symptoms started pretty mild at first," recalled Lisa, a counselor in Chicago. "Even after the 14 days of staying isolated, I was feeling it in my chest, almost in a different way, almost like I have been in a smoke-filled room long after those first couple of weeks."
Today, she says, the lingering effects are taking a toll on her daily life.
"I can still function, but I feel markedly more tired at the end of the day," she said. "By 5 or 6 in the evening, I'm ready for bed."
Some COVID-19 patients are paying for something they didn't ask for: a long-term illness that affects their day-to-day life. These COVID-19 sufferers, dubbed "long-haulers," experience a multitude of long-term symptoms, which has created a new unknown for doctors trying to combat the virus -- and new challenges for patients trying to return to work or school, or just live their lives in a normal fashion.
In a multi-state survey report from the CDC, 35% of patients who tested positive for COVID-19 with symptoms had not returned to their usual state of health when interviewed two to three weeks after testing. Experts don't yet know the exact percentage of people who are likely to suffer these long-term effects, or how long the symptoms last.
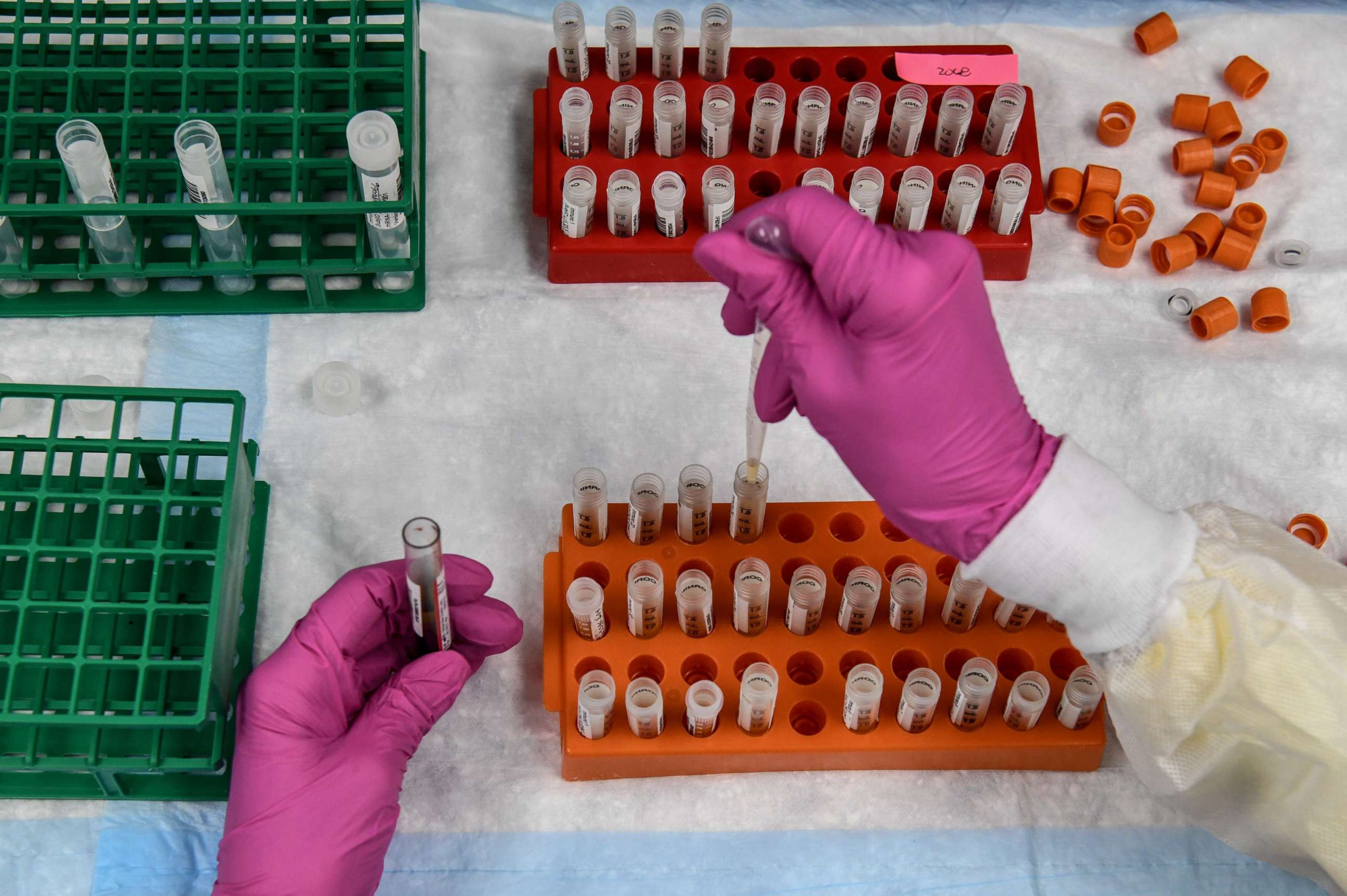
According to a survey conducted by the British Medical Association (BMA) and reported in the BMJ, one-third of the 3,729 doctors surveyed have treated patients with long-term COVID-19 symptoms, including chronic fatigue and loss of the sense of smell.
"I would probably see a patient who has complaints of an atypical story of COVID, which is now becoming typical," said ABC News Medical Contributor and board-certified ER physician Dr. Darien Sutton, who served on the front lines of the COVID-19 pandemic in New York City. "The symptoms that bring them is shortness of breath. Patients don't seem to get back to normal."
"The common symptoms are lethargy and chronic fatigue," explained Sutton. But the problem, he said, is that the medical community still doesn't understand why this happens to some patients and not others, and how long it might last.
"We don't have enough cases to develop a trend and don't have enough research to develop a fact," Sutton said.
In addition to fatigue, some of the common symptoms that patients have experienced during their recovery from COVID-19 include muscle weakness, loss of sense of smell, and concentration difficulties. But experts say it's too soon to know if some people will have persistent symptoms that last for months or years, because the pandemic is only about six months old.
Sutton is hopeful that eventually, even long-haulers with persistent symptoms will recover.
"Some people have a longer story than others," he said. "I don't think this is something that is permanent. I think this is something they have longer than others."
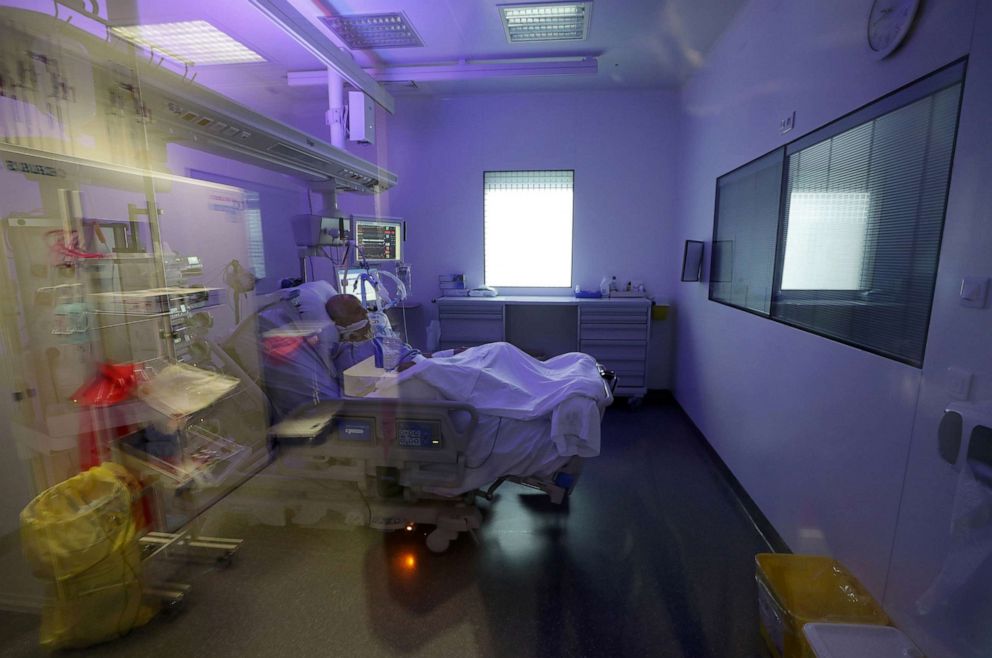
Other doctors are less optimistic, saying COVID-19 might cause permanent damage in some people.
"The important thing to note is that statistically, long haulers may be charted as folks who have recovered from the illness -- but in reality, their life is forever changed and they will likely never be the same," said Dr. Sunny Jha, an anesthesiologist caring for COVID-19 patients in a special hospital in Los Angeles.
Some universities are creating clinics and centers to assist and monitor patients with symptoms persisting after COVID-19. For instance, the University of Miami's Dr. Raul Mitrani, a cardiologist who specializes in electrophysiology, created a post-COVID-19 cardiac clinic to screen patients for residual heart problems. A center for post COVID-19 care was also created at Mount Sinai in New York City.
In today's new normal of interacting with friends and family, as well as returning to work or school, experts are grappling with the question of how to treat people who persistently experience symptoms. Dr. Rebekah Gee, clinical associate professor at the LSU Schools of Public Health & Medicine, says doctors need to support those in recovery from the virus.
Health authorities outside the United States are also taking notice. Last month, LongCovidSOS, a patient advocacy group composed of long-haulers in the UK, had an invitation-only meeting with top officials from the World Health Organization (WHO). Earlier this spring, scientists met with WHO and Centers for Disease Control officials to discuss how to help long-haulers lead healthier lives.
For Lisa Fitzgerald, who does not have any underlying medical conditions, it was confusing to experience COVID-19 symptoms that lingered for months after her diagnosis.
"The one thing for me was trusting your instinct about what's going on in your own body," she said.
For now, doctors are continuing to monitor Lisa and people like her to see if they can learn more about the long-haul phenomenon. They're hoping people who experience long-term symptoms will eventually recover, and that eventually there might be new treatments for people who continue to feel sick months later.
"Even though it's improved and I can function and get through my day, I do worry about the long-term damage," said Lisa. "It's a little stressful worrying about that."
Alexis E. Carrington, M.D., is a dermatology research fellow at the University of California, Davis and a contributor to the ABC News Medical Unit. Jay Bhatt, D.O., is an internist, adjunct faculty at the UIC School of Public Health, and ABC News Contributor.