Fears of COVID-19 resurgence in the US grow as officials warn of potential upticks
Over the last week, virus-related hospitalizations in the U.S. have plateaued.
Amid a growing COVID-19 surge occurring overseas, there are renewed concerns among health officials in the United States that the spread of the highly transmissible omicron subvariant BA.2, combined with waning vaccine immunity and the decision to end masking recommendations, could cause the country to face yet another viral resurgence.
"What we're seeing in Europe, and particularly in the U.K., is something we really need to pay attention to because they are starting to see a reversal and a resurgence of cases," Dr. Anthony Fauci, chief medical adviser to the White House, told "GMA3" on Friday. "So even though our cases are continuing to come down, I would not be surprised if in the next couple of weeks ... that we might well see an increase in cases."
The Centers for Disease Control and Prevention estimate that 23.1% of new cases in the U.S. are BA.2. Studies estimate that BA.2 is between 30% and 80% more infectious than the original strain, and federal data shows its presence in the U.S. is nearly doubling every week.
There are already initial indicators that the nation may be on the brink of an uptick as the nation begins to see a plateau in infection and hospitalization rates, which were previously declining.
Earlier this week, wastewater data shared by the CDC revealed that between Feb. 24 and March 10, 37% of wastewater sites monitored by the CDC have seen an increase of 100% or more of the presence of the COVID-19 virus in their wastewater. Approximately 30% of these sites have seen an increase of 1,000% or more
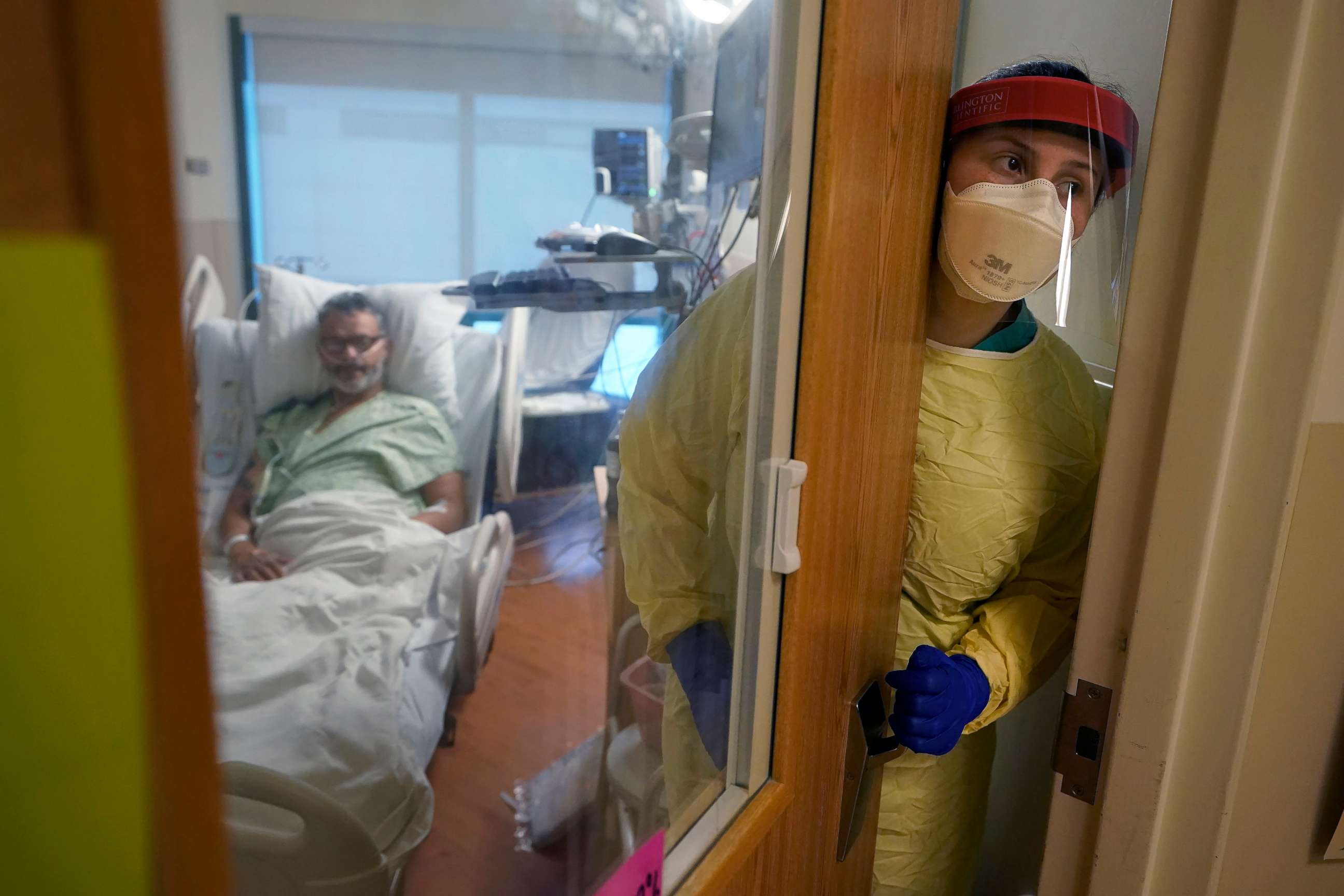
Nationwide, new data shows that COVID-19-related hospitalizations appear to also be plateauing following weeks of steady decline. Over the last two months, hospitalization levels had been dramatically falling, but over the last week those daily declines have become steadily smaller.
Virus-related hospitalizations now stand at about 23,000 patients, according to federal data.
"You just got over a wave of the most transmissible #SARSCoV2 variant the world has seen, with the highest level of hospitalizations in the pandemic," Dr. Eric Topol, professor of molecular medicine at Scripps Research, said in a tweet on Thursday. "Now you are facing a variant [with] 30% more transmissibility, [without] mitigation measures, low [vaccination] coverage, and gutting funding."
CDC Director Dr. Rochelle Walensky said Thursday that she too anticipates there could be an increase in new virus cases in the U.S. as BA.2 spreads, warning that it is "certainly ... possible" that mask recommendations will have to be reimplemented.
"We want to make sure that people have an opportunity to relax their mitigation strategies when things are good, as they are right now," Walensky said during a panel discussion with the Bipartisan Policy Center.

"But then, they should put that mask in a drawer, because if we have more cases that occur in the winter time, if we have more cases that occur because of a new variant, we want to make sure that people have the opportunity to take those masks off, so that we can re-implement them and protect people, should we need them again," she added.
Officials are closely monitoring the viral resurgence occurring overseas, Walensky said, and looking for clues as to what it might foreshadow for the crisis in the U.S.
However, overseas, similar to the previous omicron surge, there are hopeful signs that should there be a resurgence, intensive care units and morgues will not be as overwhelmed as in past surges. In the U.K., ICU capacity has yet to see a notable increase, which experts say could ultimately prevent a significant spike in virus-related deaths.
"Their intensive care bed usage is not going up, which means they're not seeing a blip up of severe disease," Fauci told ABC News' Brad Mielke on the podcast "Start Here," in an interview that aired Friday, adding that officials in the U.K. have not reported an increase in severity due to the BA.2 subvariant.
The best way to evade a significant surge will be to get vaccinated and boosted, Fauci said.
Earlier this week, the CDC released data showing that vaccines are still dramatically reducing the risk of hospitalization or dying from COVID-19.
In January, unvaccinated adults were nine times more likely to die of COVID-19, compared to vaccinated individuals, and six times more likely to require hospitalization. Unvaccinated adults were about 21 times more likely to die of COVID-19 in January, and 12 times more likely to require hospitalization, compared to fully vaccinated and boosted adults.
Although breakthrough COVID-19 infections surged during the omicron wave in February, unvaccinated adults were still 2.8 times more likely to test positive for COVID-19 compared to fully vaccinated individuals, and 3.2 times more likely to test positive compared to fully vaccinated and boosted adults.
Experts say Americans must be flexible and willing to take on the future challenges that may present themselves as we move into the next phase of the pandemic.
"We're not done with this pandemic as much as we all wish. We are not," newly named White House COVID-19 coordinator Dr. Ashish Jha said during an appearance on "Good Morning America" Friday. "Whatever the pandemic throws at us, we have got to be ready for it."




