Health officials plan for updated vaccines with an eye on COVID’s unpredictability
Scientists caution that planning ahead in this pandemic is challenging.
Updated COVID-19 vaccines that could better match the more recent variants are on the way.
On Tuesday, the U.S. Food and Drug Administration's committee of independent advisors met and recommended that the vaccines should target the latest omicron variant, kicking off the process for distribution of the new vaccines this fall.
That could be good news for the fight against the virus. But the next few months hold a lot of uncertainty.
Many vaccine scientists agree that as the virus evolves, vaccines should be updated along with it. But scientists caution that planning ahead in this pandemic is challenging. A new variant could emerge by the fall, rendering even new vaccines old by then.

There's also a question of how many people will get the shot -- both because the government doesn't have enough funding to secure vaccines for everyone, and because less than half of eligible Americans have received their first booster shots.
That said, the vaccine companies have been testing different strategies for a new-and-improved booster shot.
On Tuesday, the FDA's advisers reviewed the data and favored a bivalent vaccine -- a type of vaccine that targets two strains of virus in the same shot. They recommended that it include the latest omicron subvariant and the original strain, generally supporting it because it could protect more broadly against future variants.
FDA leadership will announce the final decision sometime in early July, incorporating the advisers' discussion from Tuesday.
Health officials are aiming to roll out the newly designed vaccines in early October, said Dr. Peter Marks, who oversees the FDA's vaccine department.
The goal is to get ahead of a potential surge next winter.
"That combination of waning immunity, combined with the potential emergence of novel variants during a time this winter when we will move inside as a population, increases our risk of a major COVID-19 outbreak," Marks said.
"And for that reason, we have to give serious consideration to a booster campaign this fall to help protect us during this period from another COVID-19 surge," he said.
How much better will the new vaccines be?
Scientists cautioned that existing vaccines are still working well to prevent severe illness.
And while newer shots will help, they might not be significantly better at preventing more mild breakthrough illness.
"It will be better than what we have now, but I don't think we are going to see 94% again," said Dr. Paul Goepfert, professor of medicine at the University of Alabama at Birmingham.
The current vaccines, designed to match the original Wuhan virus, initially showed efficacy of 94% -- but that's now thought to be an untenable goal because of rapidly-evolving new variants, Goepfert said.
"It's essentially an arms race," said Dr. Dan Barouch, author on the recent study and director of the Center for Virology and Vaccine Research at Beth Israel Deaconess Medical Center in Boston. "As the population becomes more immune, the virus becomes more and more immune evasive."
Updated vaccines "will be helpful," Barouch said, but are unlikely to be a "game changer" that end the need for future boosters.
The political snag getting in the way
The other major caveat to the rollout of new vaccines this fall is funding -- the battle over which has been stuck in a stalemate on Capitol Hill since the winter.
The White House has since pulled funds out of COVID test manufacturing and put it toward contract negotiations for the newest vaccines, but the decision leaves the US vulnerable to a testing shortage, and still doesn't fully do the job.
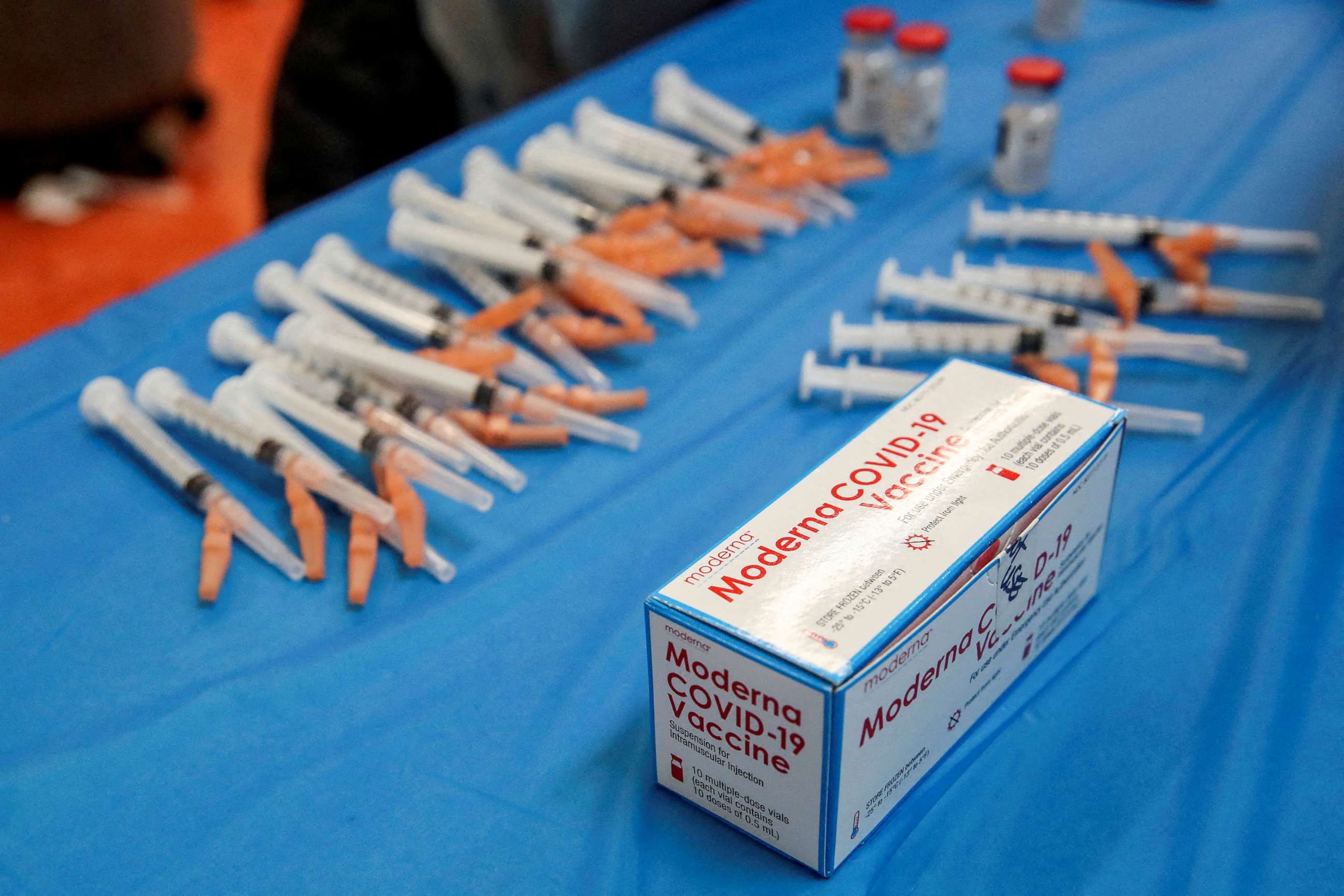
"It's very clear we're not going to have enough vaccines for every adult who wants one," Dr. Ashish Jha, the White House's COVID coordinator, said last week.
Jha called the decision to move money away from testing "incredibly painful," but necessary to avoid missing out on orders entirely as other countries placed theirs.
"Contract negotiators on behalf of the US government are going to enter into contract negotiations with Moderna and Pfizer with the resources that we've been able to … cobble together for vaccines for the fall," Jha said.
The government will purchase enough for high-risk Americans to get the latest vaccines, Jha said.
But it's unclear how the rest of the population will get access to the vaccines. On one hand, demand for vaccines has continued to drop since the initial doses. If that trend continues and fewer people want a vaccine, it's possible that the government's smaller order could still cover people who want one.
And some experts don't think everyone will need a booster in the fall, like Dr. Paul Offitt, the director of the Vaccine Education Center at Children's Hospital of Philadelphia, who said he thinks re-upping antibody levels ahead of a likely winter surge would be beneficial for high-risk groups, but not necessary for everybody.
Another option is for insurance companies to step in and cover vaccines, rather than the government distributing them for free. Jha dismissed this option, though, calling it too soon to switch to the private market because there's still too much competition for ordering doses among countries and insurance companies wouldn't have enough leverage.
"There is not a commercialization plan that somehow would be ready in time for this fall and winter," Jha said.
Yet vaccine companies have indicated that they're ready to distribute their vaccines through insurance companies and won't leave the American market behind.
Though it's still months away, both the White House and the vaccine companies have committed to devising a plan as fall draws closer.




