'A horrible way to go': The pandemic's toll on nursing home residents and their families
Some have turned their efforts to increasing access for essential caregivers.
In May, Robin Taylor and her family visited her father, Bobby Rorer, at his veterans home. They participated in a car parade.
"They brought all the residents outside and had them sitting out there in front, and then all the families had the cars all decorated. We drove around the building honking the horns and acting goofy for the guys," Taylor told ABC News. "That was the last time any of us really got to see him."

Rorer is one of over 110,000 lives lost due to COVID-19 in long-term care facilities, based on a tally by The COVID Tracking Project. The World War II veteran died at the age of 96 after contracting the virus in early October, amid an outbreak that killed 26 other veterans in his Kentucky facility.
Long-term care facilities like nursing homes are especially vulnerable to COVID-19 outbreaks, given their congregate settings and high-risk populations. As of Dec. 10, they have accounted for 39% of COVID-19 deaths in the U.S. -- despite representing only 1% of the population, according to The COVID Tracking Project.
Measures to protect residents have often meant that people have been unable to see or provide care for their family members for months on end, speaking via Zoom, over the phone or through window panes. Residents and staff of long-term care facilities will likely be among the first, along with health care workers, to have access to a COVID-19 vaccine. But for many, it's too late.

In the last days of her father's life, Taylor would call her father's facility so that a nurse could hold the phone up in his room.
"We never really knew if he knew it was us, if he could understand that we were there," she said. "He lived a good long life, don't get me wrong. He had a great life. But it's such a horrible way to go when you've got all this loving family, but yet none of them are with you at the end. It's really sad."
'Safe and reasonable' access
As COVID-19 cases have surged across the country, it's become harder for long-term care facilities to keep the virus out. On Dec. 10, The COVID Tracking Project reported the highest number of weekly new cases in long-term care facilities since it started collecting the data in May.
Mary Nichols' mother, Martha, has been in the COVID-19 wing of her Texas nursing home since testing positive for the virus last month.
Nichols told ABC News her mother has a camera in the room, and she watches her mother sleep most nights because the Alzheimer's patient regularly chokes. Since the door to her mother's room is closed due to her diagnosis, the staff may not hear her struggle to breathe, so Nichols calls the facility if her mother needs suctioning.
"It's about a 15- to 20-minute nightmare when my mom does that," Nichols said. "I am trying to keep her comfortable for whatever amount of life she has left, and her laying and choking for 20 minutes is not keeping her comfortable."
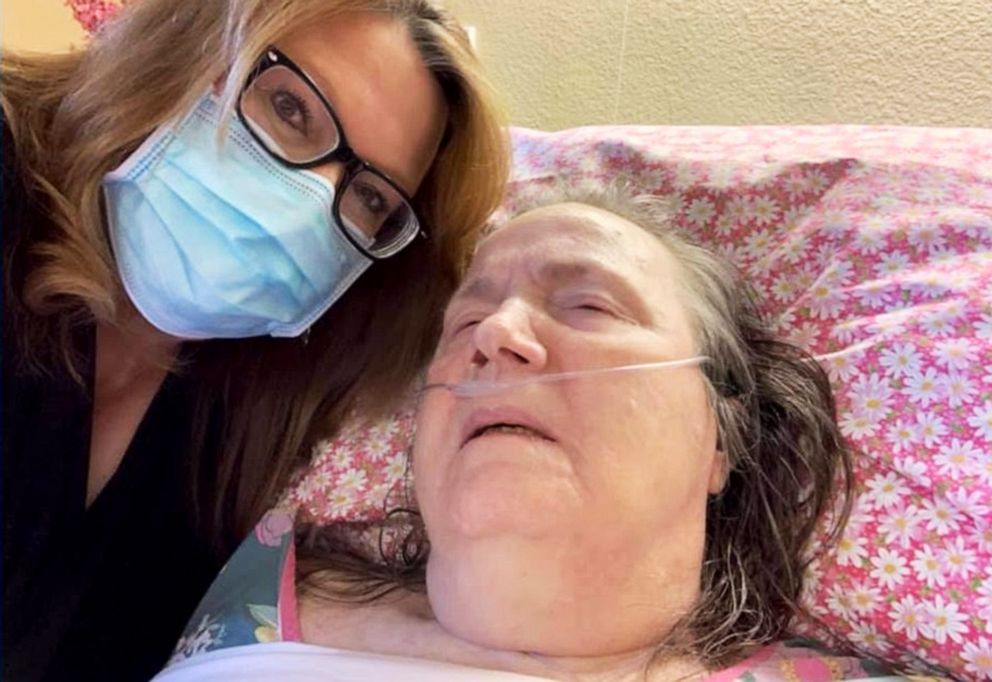
Nichols said she went 202 days without seeing her mother, until Texas started allowing essential caregivers to visit residents who do not have COVID-19 for one hour once a week in September. That would give her enough time to wash her mom's face, apply lotion and trim her nails, she said. Otherwise, she has an Echo device in the room, through which she can talk to and play music for her.
"As essential caregivers, one hour once a week does not allow us to do those caregiving duties we did before being locked out," said Nichols, who normally would visit her mother almost daily to provide care, read to her or spruce up her room with pink -- Martha's favorite color.
Nichols is the founder of the Texas chapter of Caregivers for Compromise, a pandemic-borne national coalition that advocates for the reopening of long-term care facilities, such as through essential caregiver designations, to combat isolation. In addition to Texas, a handful of other states, including Florida, Indiana and Minnesota, have loosened restrictions for essential caregivers.
Nichols is working to improve her state's policy to find ways to provide "safe and reasonable" access. She also guides others in similar situations through any confusion around the new guidelines and to make strides in their state's essential caregiver policies. Though as long as COVID-19 remains a high threat for facilities, they are less inclined to let in additional personnel, she said. Her mother hasn't seen her hospice aids since March, she said.
"The fewer people they can let in the building, the safer they feel they are," Nichols said. "There's some logic to that, but it's really a hard pill to swallow when it's your mom that's not getting the comfort care that you think she's entitled to."
'Isolation was tough on her'
Andrea Goldy in upstate New York is one of over 14,000 members who have found their way to the Caregivers for Compromise Facebook page during the pandemic.
Her mother, Marlene, was very active and social -- always up for a party or Bingo game. After breaking her leg last year, she moved into an assisted care facility. A nursing home stay followed this summer when her health declined. Goldy told ABC News that she loved the medical care her mother received, but the "isolation was tough on her."
"If you don't have a roommate, you stay in a room by yourself," Goldy said. "There's no communal dining. There's no activities. Would anyone want to live like that?"
Normally, Goldy would visit her mother every other day and assist in caregiver duties such as bathing. Due to COVID-19 restrictions, Goldy said she was only able to have a few socially distanced visits outdoors beginning in September. Because her mother was legally blind and hard of hearing, though, those meetings were challenging.
Goldy could visit her mother whenever she was hospitalized, so she would make the 90-minute drive from work to get there in time for the start of visitation hours.
"I would take every opportunity I could to see her," she said. "They weren't fun opportunities, but I took every opportunity I could to be with her."

Marlene was hospitalized one final time, before her death in October from an upper gastrointestinal bleed at the age of 87. Goldy considers herself lucky that was able to be by her mother's side the last seven days of her life.
The New Yorker is pushing state officials to pass emergency legislation before the end of the year that would expand long-term care facility visitation for essential caregivers, like Texas has done.
"I wish that her last year could have been more fulfilling," she said. "I'm going to turn all my negative energy, all my heartache, into a fight to see that other families don't have to go through this."




