Inducing hypothermia can help get ICU patients with COVID-19 off ventilators, doctors find
The treatment, sometimes used after cardiac arrest, may be beneficial.
Since the novel coronavirus caught the world's attention in December 2019, doctors have been trying to determine how the virus damages the body -- and trying innovative treatments to stop it in its tracks. Now, they may have found one solution for treating COVID-19 patients in critical condition.
Some of the most serious cases of COVID-19 require long periods of time in the intensive care unit, on ventilators. Out of options, a group of doctors at Northwell Health's North Shore University in Manhasset, New York, took a step back and wondered if they could stop the virus from causing further damage by introducing freezing temperatures.
"We had exhausted all therapies," Dr. Hugh Cassiere, the director of critical care services at Sandra Atlas Bass Heart Hospital at North Shore University, told ABC News. "We wanted to find a solution to be able to rest the lungs and the body, and thought of the process of cooling the body."
Doctors say when patients are critically ill, and require mechanical ventilation, the elevated metabolism can break down the muscles used in breathing, leading to difficulty in patients coming off invasive ventilation. The high levels of carbon dioxide, the low levels of oxygen, and highly acidic blood creates the perfect storm for organs to fail.
While sick in the ICU with COVID-19, a patient's body may look like it is resting, but there may be an increase of energy being used as a result of high fevers, a hyper-inflammatory response, or cytokine storms. This is called the hypermetabolic response.
The premise of targeting the hypermetabolic rate is to prevent the body from using so much energy, such as oxygen, which can cause muscle breakdown and make ill patients weak and frail.
"Lowering the body temperature has been shown to decrease the metabolic rate, which is why we chose to use this therapy," Cassiere told ABC News. He further explained that these lower temperatures slow down the chemical reactions in the body that can potentially turn fatal.
The group introduced the cooling down procedure to four critically ill patients -- who were out of other options are were believed to be close to death -- for 48 hours. They found that therapeutic hypothermia decreased hypermetabolic states caused by COVID-19 and improved lung function in two of the patients who had severe infections with multi-organ failure. The doctors published their experimental results in Metabolism Open, a peer-reviewed, open-access journal that publishes original research.
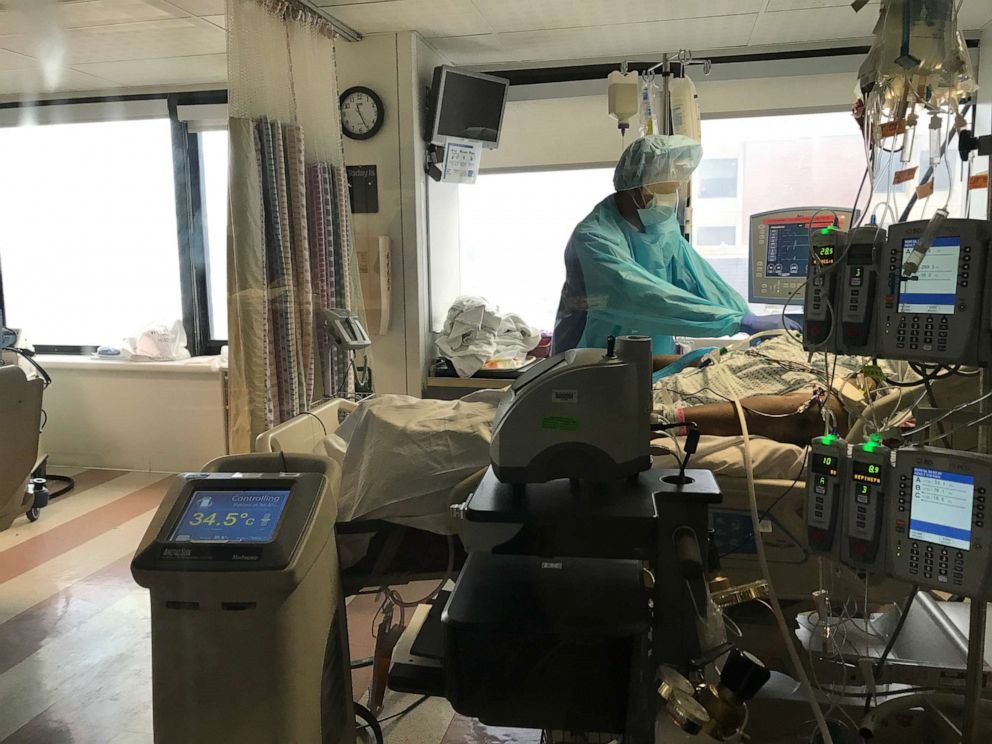
The four critically ill patients were given one more chance to fight the virus with the therapeutic hypothermia. They were cooled to 34.5 degrees Celsius (94.1 degrees Fahrenheit) for 48 hours. All four patients were calculated to have reduced metabolic activity and improved oxygen levels in their blood.
Two of the four patients -- who had exhausted therapies available to them and were thought to have lost the battle against the novel coronavirus -- were successfully taken off mechanical ventilation after the treatment.
"These patients would have died without the hypothermia," Cassiere told ABC News. The team had planned to see if they could get patients off mechanical ventilation, but instead they had better results: survival.
"We were seeing that these patients with COVID-19 were dying from organ dysfunction because they were unable to remove these high levels of carbon dioxide being produced," said Dr. Pey-Jen Yu, a cardiac surgeon and the surgical director of clinical research at Sandra Atlas Bass Heart Hospital at North Shore University Hospital, who was also the lead author of the paper.
The team involved in the paper was seeing other supportive measures, such as extracorporeal membrane oxygenation (ECMO) and mechanical ventilators, fail in supporting lung function and suppressing the high levels of carbon dioxide in patients' blood.
"When you have acid in the bloodstream all the normal body functions start to shut down and severe psychosis leads to multi organ system dysfunction and can lead to death." Cassiere said. "The reason we want to highlight that is because [in] some of our most challenging patients with ventilator management [death] isn't [caused] because of oxygen problems, the carbon dioxide and the acid in the blood are the issue. It's all connected."
Yu said that therapeutic cold temperatures are not new. During cardiac surgeries, she uses therapeutic hypothermia to decrease the metabolic rate to preserve organ vitality. Therapeutic hypothermia is also used after cardiac arrest; studies have shown that dropping the body temperature to 32-36 degrees Celsius for 24 hours helps preserve brain function.
Prior to starting the therapy on these patients, Cassiere informed ABC News that he and his team first found the longest duration of time the human body could tolerate hypothermia. He also said they used 34.5 degrees Celsius as it was the most common temperature used in established protocols, such as for cardiac arrest.
Therapeutic hypothermia doesn't stand without risks, explained Dr. Viren Kaul, a pulmonary critical care specialist at Crouse Health and an assistant professor of medicine at SUNY Upstate Medical University. When cooled, he said, patients have the risk of developing arrhythmias, increased bleeding and electrolyte abnormalities. More concerning are the complications that can occur during the rewarming phase if done too quickly: brain swelling, dangerously high potassium levels and seizures.
Although this paper presents a novel idea to help suppress the damage caused by COVID-19, Kaul warned that improved numbers (regarding metabolic status) do not always translate to survival. The medical community needs to understand what this means for patients and the public.
Despite the uncertainty, Kaul said he is excited to see more research on using hypothermia as a supportive measure for COVID-19. If patients are living after severe SARS-CoV-2 infections, then Kaul would like to know at which point during the infection patients would benefit from therapeutic hypothermia.
Fortunately for Kaul and doctors still on the front lines of the COVID-19 pandemic, Yu and Cassiere's research team was recently approved by the Feinstein Institute to actively enroll patients to further study therapeutic hypothermia and its effects on the coronavirus.
Lily Nedda Dastmalchi, D.O., M.A., is an internal medicine resident physician at The George Washington University and a contributor to the ABC News Medical Unit.




