A look inside a rural Louisiana hospital on the front lines of a pandemic
"When it starts getting into your local hospital, it becomes real."
This is a Kaiser Health News story.
The folding chairs outside the windows appeared late last month, after the maintenance staff at St. James Parish Hospital labeled each window with a patient room number so families and friends could at least see their loved ones battling COVID-19.
Yet even this small solace the Louisiana rural hospital can offer is tainted for clinical nurse educator Leslie Fisher. She has to remind the family members to take shifts to properly social distance from one another — even when their loved ones could be in their final moments.
The difficult conversations feel unceasingly cruel, she said, but she feels she has an obligation to protect these people, too. All she can do is look them in the eyes and say, “I’m so, so sorry.”
This is the new normal for St. James Parish Hospital, a 25-bed rural hospital about 45 minutes from pandemic hot spot New Orleans. Its county — or parish, as they’re called in Louisiana — of 22,000 residents had confirmed more than 175 cases and six deaths as of Tuesday. That earns it the horror of being one of the hardest-hit counties nationwide for cases per capita, placing its rural hospital that sits just blocks off the east bank of the Mississippi River onto the front lines with a continuous swell of patients.
Previously battered by hurricanes and a flood, the hospital is used to more than its fair share of disasters. But, in the aftermath, they have historically been able to rally help from around the country, CEO Mary Ellen Pratt said by phone.

Now, communities nationwide must fight their own battles, leaving St. James Parish Hospital to make do with limited staffing, testing, personal protective equipment and mechanical gear. Although working with limited resources is something rural hospitals know how to do, Pratt said, this is something entirely different.
Before the pandemic, the hospital housed about eight inpatients a day. Almost overnight, it’s up to 20 inpatients some days, the majority of them with suspected COVID-19. Dozens of positive cases, with many more feared, have passed through its doors.
To add to the challenge of the crush, the patients’ conditions are more severe than those of typical patients, especially for a hospital without an official intensive care unit.
Although the hospital has had two ventilators the staff can use before transferring patients to more advanced facilities, the wait times to transfer patients to other hospitals continue to lengthen. Pratt said she is dismayed at how often she’s had to use the ventilators so far.
“We’re intubating every single day, several patients a day, when we maybe do it on a monthly basis,” she said. “It’s crazy.”
The hospital is planning to bring five more ventilators online in the next few days — three are rentals, one is a converted anesthesia machine, and a staff member drove six hours round trip to pick up one from another rural Louisiana hospital.
The bigger hospitals 45 minutes away continue to be packed with their own COVID-19 patients. If those hospitals begin to deny transfer requests, Pratt and her staff may be forced to make unthinkable decisions about rationing care.
Fisher can hardly speak of the possibility.
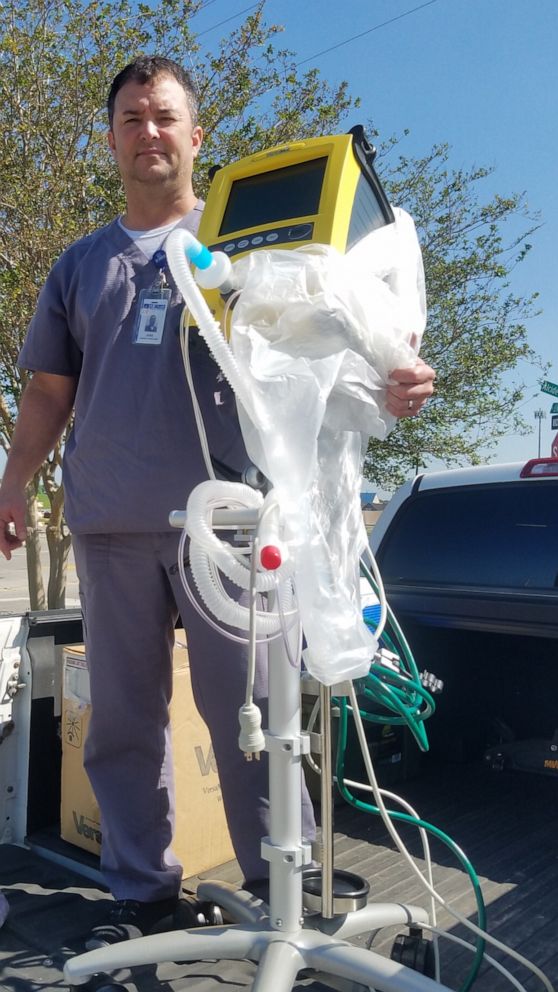
“My biggest fear and the fear of the entire hospital is that we’re going to have to end up choosing who we are going to ventilate,” she said. “I want to ventilate everyone. I want everyone to live.”
An Onslaught Of Patients
Community member Maitland John Faucheux III — who goes by “Spuddy” — didn’t think there was much to this whole coronavirus thing at the beginning of March, which feels like an eternity ago now to him. The 62-year-old owner of Spuddy’s Cajun Cooking, which is about 18 minutes from the hospital, said that in retrospect he was a bit hardheaded about the whole thing.
But then the Rev. Leon Franklin, a 60-year-old Baptist pastor in St. James and a “jolly” customer for years, died at St. James Parish Hospital of COVID-19 in mid-March.
“When it starts getting into your local hospital, it becomes real,” Faucheux said.
The hospital, on the other hand, had been preparing since January. As soon as it had its first suspected case, a patient who arrived on March 13, it activated its emergency operations. As more people of all ages came in complaining of a fever, cough and respiratory symptoms, Pratt ratcheted down the hospital’s five entrances to three. Anyone who enters now is checked for fever. Hospital staff also redesigned the internal layout to offer more separation from COVID-19 cases.

Elective surgeries, therapies, tests and labs — which provided about 80% of the hospital’s revenue — were canceled. Pratt said she’s been too busy dealing with the crush of patients to even think about the implications for the hospital’s bottom line. That’s a real concern because even before the virus struck, many rural hospitals nationwide limped along financially, with more than 120 closing in the past decade.
Typical days in the emergency room start by triaging suspected coronavirus patients by measuring the oxygen saturation of their blood, the hospital’s emergency room medical director Dr. Will Freeman said. For those patients in better shape, hospital staff must spend a fair amount of time convincing them it’s safer to be at home.
Top of mind is how to manage the diminishing amounts of personal protective equipment: Nurses are each given one N95 mask a day and put a protective mask on top of it.
Testing has been another frustration.
“We’re still limited,” Freeman said. “Not every person is getting tested, for darned sure.”
Freeman urged other rural hospitals nationwide to start planning today.
“If you’re one of the fortunate areas that doesn’t have many cases — that doesn’t think it’s coming — it’s going to come,” he said. “One day, it’s going to be there.”
The Underlying Fear
The surrounding community has stepped up — sewing cloth mask protectors and making a big sign outside the hospital that says “HEROES WORK HERE.” Using Facebook, a resident raised thousands of dollars to buy the staff food and snacks.
But the personal toll and sacrifice have been heavy for staff. They’re working all hours of the day, in enhanced roles — techs who normally assist with surgery are working as aides in the COVID-19 unit, Pratt said. Employees are being repurposed to clean rooms for infection control.
Fisher’s face is another marker — she has a bandage across her nose from the constant digging of her goggles into her skin.
Every day, it seems, someone else’s family member or a member of the community needs treatment, Freeman said.
“We take care of all of our patients like they’re our family, because they are our family,” he said.
Which is one of the staff’s greatest concerns: what they’re bringing home. Fisher sent her kids, ages 7 and 11, away to her parents’ house and now FaceTimes her girls each night, which she said is incredibly difficult.
“My child asked me the other day why am I a nurse,” she said. “And my answer was God called me to be one.”
Laurie Webb, the hospital’s cardiopulmonary director and a registered respiratory therapist, started sobbing when talking about her own 4-year-old and 9-month-old. She isn’t able to send them away because of their ages. Her nightly routine involves stripping naked in front of her patio — “it’s pretty humiliating” — putting her clothes in a bag, Lysol-ing her shoes and heading straight for the bathroom.
“I’m completely terrified of what I’m bringing to my children and husband, but I can’t stay away from my family,” she said through tears.
As of Tuesday, 16 of the hospital’s more than 200 employees had tested positive for the coronavirus.
During one call with KHN, Pratt, the CEO, coughed.
“I am feeling OK,” she said. “I’m just tired.”
On her mind, always, is what happens if more and more and more patients keep coming — and the hospital runs out of ventilators.
“I can’t imagine. I don’t want to think about it,” she said. “I pray that we don’t get there.”
Kaiser Health News is a nonprofit news service covering health issues. It is an editorially independent program of the Kaiser Family Foundation, which is not affiliated with Kaiser Permanente.




