World's 2nd-largest continent Africa sees steep rise in coronavirus cases
Africa is poised to potentially become the next epicenter of the pandemic.
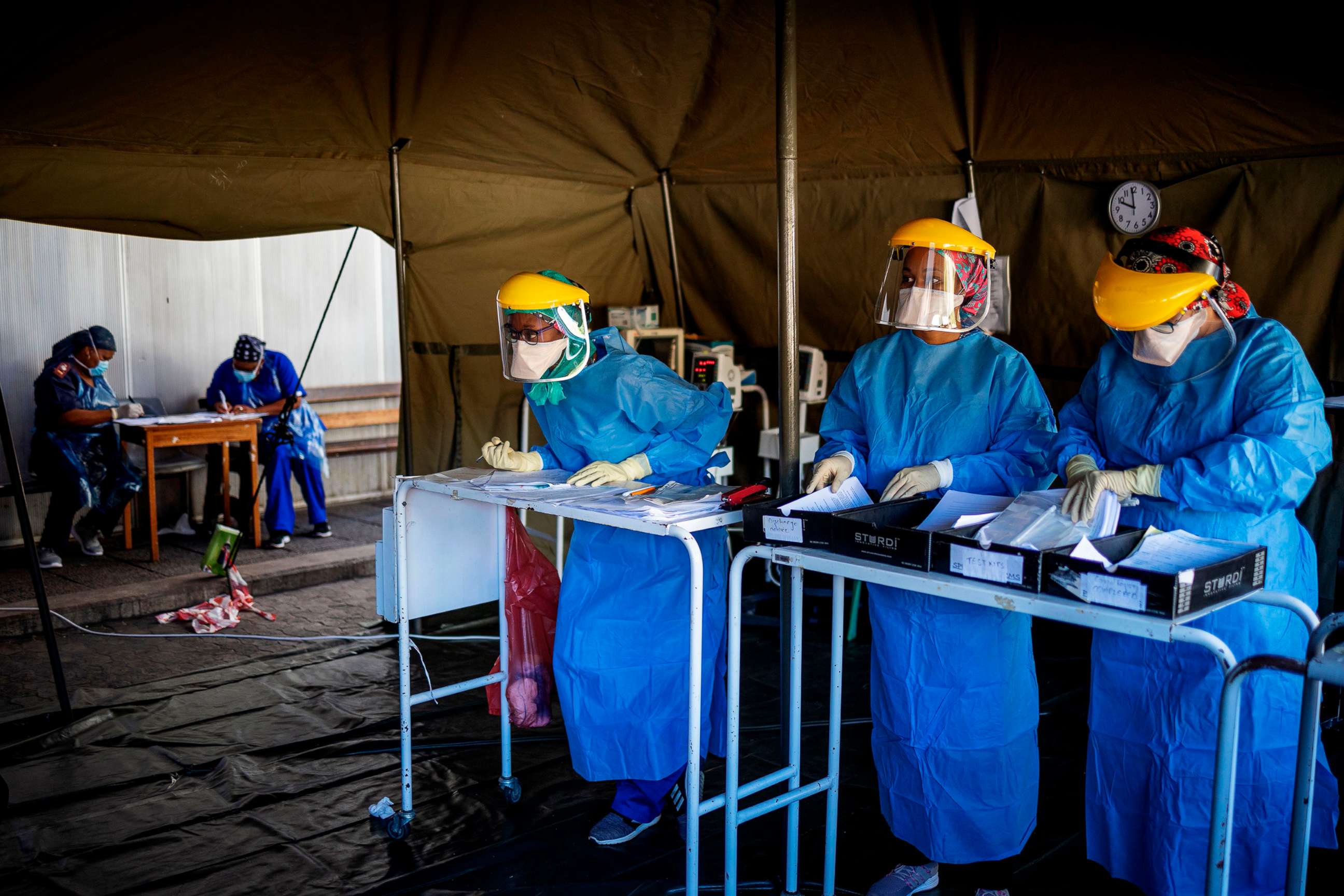
LONDON -- On a recent morning in South Africa's port city of Cape Town, Patsy Oosthuizen was working her volunteer shift in the coronavirus screening tent outside Tygerberg Hospital when a woman who had been waiting in line suddenly broke down in tears before her.
The woman, whose name is not being revealed for privacy reasons, had brought her young child who was severely ill and had to be admitted for treatment straightaway. Due to the infection control measures, the mother wasn't allowed to go with the child and instead had to remain in the screening tent so she could be tested for COVID-19.
Oosthuizen, a 22-year-old South African native and fifth-year medical student at nearby Stellenbosch University, was clad in protective gear from head-to-toe and had to maintain a two-meter distance away from the distressed mother as she took down her information on a clipboard.
"It was very odd because I couldn't even touch her, I couldn't comfort her," Oosthuizen told ABC News in a recent telephone interview. "If she was tested positive, there was a possibility of her not being able to be with the child at that stage. So she had a lot of anxiety surrounding that and she had a lot of questions that no one at the moment could really answer for her. It's really scary for a lot of people because they don't understand necessarily how the disease works."
In the last week alone, there has been a 43% jump in the number of reported COVID-19 cases in Africa, and the World Health Organization (WHO) has warned that the continent of 1.3 billion people is poised to potentially become the next epicenter of the highly infectious and deadly disease.
A global pandemic of the novel coronavirus is affecting virtually every country in the world since it first emerged in China in December. Nearly 3 million people worldwide have been diagnosed with COVID-19, the name given for the disease caused by the new respiratory virus, and over 207,000 have died, according to data compiled by the Center for Systems Science and Engineering at Johns Hopkins University. The actual numbers are believed to be much higher due to testing shortages, many unreported cases and suspicions that some governments are hiding the scope of their nations' outbreaks.
Africa's first diagnosed case of COVID-19 was reported in Egypt on Feb. 13. Now, more than 32,000 cases have been recorded across the world's second-largest continent in nearly all 54 nations. Over 9,000 patients have recovered while at least 1,423 have died, according to the latest data from the Africa Centers for Disease Control and Prevention (CDC).
Tune into ABC at 1 p.m. ET and ABC News Live at 4 p.m. ET every weekday for special coverage of the novel coronavirus with the full ABC News team, including the latest news, context and analysis.
As the number of reported cases in Africa continues to grow, the WHO has warned that more countries on the continent are seeing the virus spread to regions beyond the densely-populated capital cities.
"Tackling cases in rural areas that often lack the resources of urban centers will pose an immense challenge for already strained health systems in Africa," Dr. Matshidiso Moeti, the WHO's regional director for Africa, said in a recent statement.
A recent analysis by the WHO found there are less than 5,000 beds in intensive care units available for COVID-19 patients across 43 African nations, which is about five beds per one million people in the reported countries compared to 4,000 beds per one million people in Europe. There are also fewer than 2,000 functional ventilators in public health services across 41 African nations that reported to WHO.
"There is a critical shortage of treatment facilities for critical cases of COVID-19 in Africa," Moeti said.
An uphill battle for underfunded, understaffed health systems
With more than 4,500 diagnosed cases of COVID-19, South Africa is one of the worst-affected nations on the continent. However, the country's reported death toll remains relatively low -- under 100. The South African government moved early in imposing a nationwide lockdown on March 26, when there were still under 1,000 cases and before a single death had been reported in the country of 57 million people. South Africa is no stranger to infectious diseases, with the highest prevalence of HIV in the world and one of the highest for tuberculosis. Malaria is also endemic in certain parts of the country.
Oosthuizen and another student volunteer, Ingrid Hartmann, both told ABC News that they have yet to see any overflow of COVID-19 patients at Tygerberg Hospital that would strain the facility's resources. Now a designated coronavirus treatment center, it's the largest hospital in the Western Cape province and the second-largest in South Africa. As of Saturday evening, 68 patients were admitted to various hospitals -- both public and private -- across the province, and 26 were in intensive care, according to Western Cape Premier Alan Winde.

Each morning, dozens of people line up at the coronavirus screening tent outside Tygerberg Hospital to see whether they need to be tested. Oosthuizen and Hartmann said as many as 200 people have come through the tent within their four-hour shift so far, during which they each screened around 30 to 40 people.
Oosthuizen and Hartmann are part of a small, tight-knit team of student volunteers and nurses charged with determining whether someone is eligible to be tested for COVID-19, after taking down their information and asking questions about their health as well as any recent travel. On average, Oosthuizen and Hartmann both said they recommend testing for around 90% of the people they see per shift. A separate team of doctors and nurses collect the sample with a nasal swab, which is then taken to the hospital's laboratory for testing.
Hartmann, a 23-year-old South African native and fifth-year medical student at Stellenbosch University, said she isn't aware of any shortage of testing kits at the hospital.
"Our criteria has loosened so we're testing a lot of people," Hartmann told ABC News in a recent telephone interview. "But I think us being able to test a lot of people is probably a sign that we have enough tests for them to be able to do it."

However, Oosthuizen said it takes around "three days or so" for the results to come back because the lab lacks adequate staffing.
"We have quite a big delay from doing the test to getting the results," she told ABC News. "We might have enough tests but we're struggling a bit with the laboratory being quite understaffed at the moment."
Oosthuizen said she doesn't know how many ventilators the hospital has but noted that there is "quite a serious criteria" to judge whether a patient qualifies for one.
Although South Africa has one of the highest national tallies of diagnosed cases on the continent, the bulk of Africa's reported infections is actually at the other end of the vast mainland. With a total of nearly 13,000 cases, North Africa is the hardest-hit region on the continent. The soaring caseloads in Egypt, Algeria and Morocco collectively account for nearly half of all diagnosed cases in Africa.
Algeria has, by far, the highest death toll from COVID-19 of any country in Africa, with at least 425 fatalities. So far, more than 3,300 people in the North African nation have been diagnosed with the disease, according to the latest data from the Africa CDC.

With a struggling economy and a weak health infrastructure, Algeria ranks among the least prepared countries in the world to respond to a health crisis in the 2019 Johns Hopkins Global Health Security Index. Although full lockdowns and other confinement measures remain in effect for some of the country's 47 million people, the Algerian government began gradually lifting restrictions on Friday as the Muslim nation observes the holy fasting month of Ramadan.
Dr. Yasser Benaferi, who works as an orthopedic surgeon at the Ouled Mohammed public hospital in Chlef, northern Algeria, told ABC News that the country's lack of ventilators hasn't posed a problem for his hospital yet because not many COVID-19 patients require ventilation at the moment. But he said there is indeed a "bare minimum" of personal protective equipment and his hospital relies heavily on donations.
"Without these donations, I don't think we would have had enough protective gear," Benaferi told ABC News in a recent telephone conversation.
There is currently no approved treatment for COVID-19, nor a vaccine to protect against the virus. However, Algeria and several other African countries are using hydroxychloroquine to treat patients, despite the lack of scientific evidence that the antimalarial drug is an effective therapy for COVID-19.
A grim outlook
South African President Cyril Ramaphosa, who is also chairman of the African Union, said the WHO has been "instrumental" in supporting African governments with early detection of cases, the training of health workers and in strengthening community surveillance.
"Africa is extremely vulnerable to the ravages of this virus and is in need of every possible support and assistance," Ramaphosa said in a video statement Friday. "For its part, the African Union has established a COVID-19 Response Fund to direct resources to bolster the continent’s response."
So far, African nations have contributed a combined amount of $61 million to the COVID-19 Response Fund and to support the work of the Africa CDC, according to Ramaphosa. Many countries across the continent have also imposed lockdowns and curfews, ordering people to stay home to prevent further spread of the virus.
“All of our efforts should complement each other," he said.

Earlier this month, the World Bank published a report projecting the pandemic would drive sub-Saharan Africa toward its first recession in 25 years. The grim assessment noted that a number of African nations have reacted "quickly and decisively" to curb its rapid transmission, but several factors could hinder the containment and mitigation measures, in particular the region's fragile health systems, poor access to safe water and sanitation facilities, and the large and densely populated urban informal settlements.
The World Bank also warned that the pandemic could spark a food security crisis in Africa due to a potentially substantial decline in agricultural production and food imports.
"The COVID-19 pandemic is testing the limits of societies and economies across the world, and African countries are likely to be hit particularly hard," Hafez Ghanem, the World Bank's vice president for Africa, said in a statement alongside the report's release.
The United States is providing assistance to some African nations but that doesn't include ventilators, personal protective equipment (PPE) and other supplies critically needed on American soil.
"We’ve spent almost a billion dollars that’s gone out the door to Africa thus far, across the continent," a senior U.S. government official told reporters Wednesday during a telephone briefing. "We are also looking at the PPE and the ventilator needs, and we’ll be making those decisions very quickly as a matter of fact."
Lessons learned from previous epidemics
As countries across Africa battle to bring the outbreak under control and public health systems become overwhelmed, the WHO has urged governments to maintain efforts on other health emergencies and preserve progress made against diseases such as malaria or polio. During the 2014-2016 Ebola outbreak in multiple West African nations that killed 11,325 people, a sudden rise in demand for health services lead to significant increases in morbidity and mortality from other diseases, including malaria.
Measles vaccination campaigns in Chad, Ethiopia, Nigeria and South Sudan have already been suspended due to COVID-19, leaving some 21 million children who would have otherwise been immunized now unprotected, according to the WHO.
“I urge all countries to not lose focus on their gains made in health as they adapt to tackle this new threat," Moeti said in a recent statement. “We saw with the Ebola Virus Disease outbreak in West Africa that we lost more people to malaria, for instance, than we lost to the Ebola outbreak. Let us not repeat that with COVID-19."

Although some lessons were learned in West Africa's Ebola outbreak, overall lifestyle habits have not changed and the health systems remain weak, according to Dr. Saya N'Guessan, who leads an epidemiological surveillance project for the International Rescue Committee (IRC) in Abidjan, Cote d'Ivoire.
"We more frequently than not go to (open) markets, and in the markets there is no possibility of regulating, especially with regards to social distancing," N'Guessan told ABC News in a recent telephone interview. "It remains a risk, even for public transport."
"The difference with this pandemic, unlike Ebola, is the speed of spread," she added, "because we do not have enough infrastructure to manage the pandemic."
Africa's porous and fluid land borders make containment measures difficult to implement. There's also misinformation and mistrust surrounding COVID-19, as was the case with Ebola.
"People said to themselves, 'No, this is a disease that Africans cannot contract, it is a virus that does not resist heat,'" N'Guessan recalled. "They had a lot of misconceptions."
Now, some people are afraid to go to hospitals when they are sick because they worry they'll contract the virus there.
"There is this fear, this feeling that exists," Aissatou Balde, the IRC's country director for Cote d'Ivoire, told ABC News in a recent telephone interview. "The mistrust that we saw during Ebola should not be happening during this period, and we have been telling that to the government here."
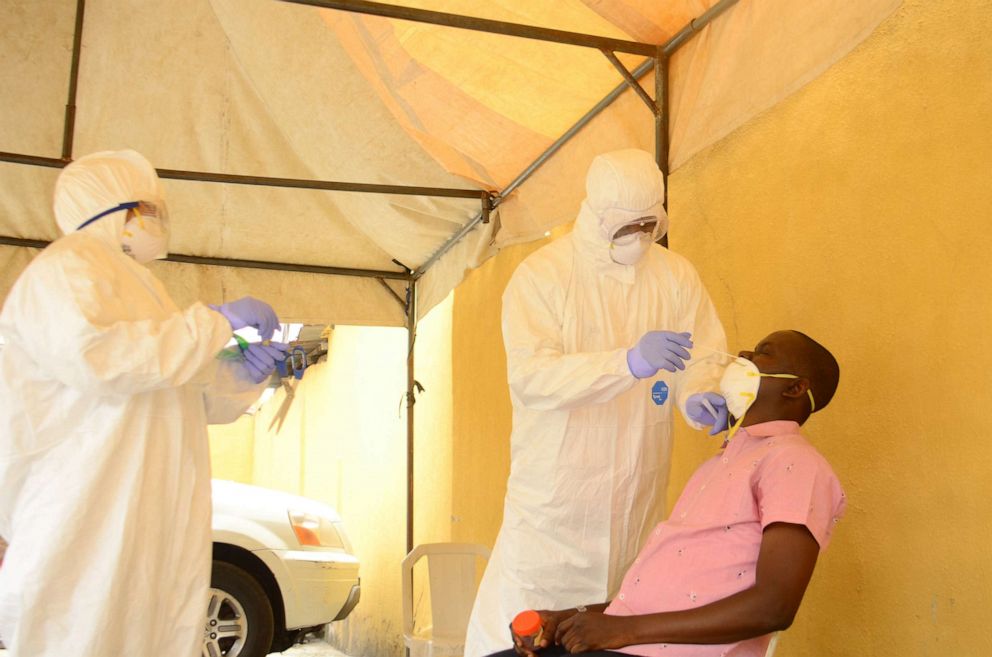
In Nigeria, the main concern is that the country's health system may not be able to cope with an increasing number of COVID-19 cases that might require critical care, according to Dr. Charles Nwosisi, a Lagos-based health specialist for the United Nations Children's Fund and a member of the Lagos State Emergency Operation Center which is coordinating the local coronavirus response.
"As the scale of this outbreak has increased, it has become increasingly challenging to keep up with the human resource and medical commodities needs required for mounting the COVID 19 response," Nwosisi told ABC News in a recent email.
Officials are working to address the shortcomings and identify more COVID-19 treatment sites across Nigeria, which has reported nearly 1,300 cases so far and at least 40 deaths. Lagos, the West African nation's largest city, has already set up a few field hospitals in preparation for the possibility of a surge in infections, according to Nwosisi.
The Nigerian Defense Academy has also developed two types of ventilators as well as a hand soap and a sanitizer that could be quickly reproduced to help stem the shortages in a country with a 195 million-strong population.
"We may not have a perfect system," Nwosisi said, "but health care workers and other individuals have turned up in a big way, despite gaps, to ensure Nigeria overcomes this pandemic."
'A triple emergency'
Meanwhile, the humanitarian community has sounded the alarm over the possibility of the virus striking Africa's most vulnerable populations who live in war-ravaged areas and overcrowded camps.
Last weekend, a Nigerian nurse who was helping treat internally displaced people in his country's conflict-torn Borno state died after contracting the novel coronavirus. Edward Kallon, the U.N. humanitarian coordinator in Nigeria, said officials are working to trace anyone whom the nurse may have been in contact within the northeastern state, where nearly 1.5 million people have been displaced from their homes in recent years due to violence from the Boko Haram insurgency and other conflicts.
"Clearly, the impact of this virus if it were to get into camps is going be devastating," Kate Moger, the International Rescue Committee’s regional vice president of the African Great Lakes, told ABC News in a recent telephone interview.

Moger said many countries within the African Great Lakes region are a definite cause for concern amid the pandemic, particularly the conflict-torn and Ebola-ravaged areas of the Democratic Republic of the Congo, the Central African Republic and its extremely poor infrastructure, Burundi and it's weak health systems, and Tanzania's highly-populated refugee camps.
The eastern Democratic Republic of the Congo has been battling an Ebola outbreak since 2018. It's the first Ebola outbreak to occur in an active conflict zone. It's also one of the largest, deadliest Ebola outbreaks in the world, second only to the 2014-2016 epidemic in West Africa.
"One of the reasons this Ebola outbreak has taken as long as it has to get it under control is the context of conflict and insecurity in which it's appeared," Moger told ABC News.

A new case of Ebola was confirmed in the northeastern city of Beni on April 10, just two days before the country's outbreak was expected to be declared over. Now, the Democratic Republic of the Congo is also faced with the novel coronavirus. More than 450 people there have been diagnosed with COVID-19 and at least 28 have died, according to the latest data from the Africa CDC.
"This is now a triple emergency: vulnerable populations facing ongoing humanitarian crises, the spread of COVID-19 and now again potentially a reemerging Ebola crisis," Moger said.
Earlier this month, the Congolese government imposed a lockdown on the capital, Kinshasa, the eastern city of Goma and a number of other major cities in an effort to slow the spread of the novel coronavirus in a country of 84 million people.
Dr. Deogratious Wonya'rossi, a Congolese public health physician and tropical diseases researcher who has been part of the Ebola response, told ABC News he's in the process of applying to take part in the local coronavirus response. He said his home province of Ituri, which was hard-hit in the country's Ebola outbreak, confirmed its first COVID-19 case on March 27. Yet he said there are still virtually no coronavirus response activities being carried out there.
"The response plan has just been completed, but I don't think that there's means to implement it," Wonya'rossi told ABC News in a recent text message. "Only radio stations are talking about [COVID-19]. Some rare posters, flyers, booklets are distributed."

In neighboring Rwanda, some remain more hopeful about their country's defenses against the new virus. The tiny East African nation of 12 million people has under 200 diagnosed cases of COVID-19 and has yet to report its first death, according to the latest data from the Africa CDC.
A doctor who works at a referral hospital in northern Rwanda told ABC News she and her colleagues have received WHO-certified training to treat COVID-19 patients. But so far, her hospital has transferred all its positive cases to Kanyinya Health Center, a designated coronavirus treatment center on the outskirts of the capital, Kigali.
"We were trained in case it spreads and the number of cases increase enough to increase the number of treatment centers," the doctor, who spoke on condition of anonymity, told ABC News in a recent text message. "But for the moment, we haven't reached there yet."
The doctor said she feels Rwanda is "prepared enough" for the outbreak as her hospital has testing kits at the ready, plenty of masks and empty beds.
"We are all worried as we see what is happening in the world, even in more developed countries with more developed medical technology," she said. "But with the measures taken to control it, like total lockdown and other sanitary measures, we hope that the spread of COVID-19 will be stopped or at least controlled."
ABC News' Halimah Abdullah, James Bwala, Conor Finnegan, Ibtissem Guenfoud and Marie Nelson contributed to this report.
What to know about coronavirus:
- How it started and how to protect yourself: Coronavirus explained
- What to do if you have symptoms: Coronavirus symptoms
- Tracking the spread in the U.S. and worldwide: Coronavirus map






