On the front line in Belgium, the epicenter of Europe's surging 2nd COVID crisis: Reporter's Notebook
Cases have skyrocketed in Liege, Belgium's third-largest city.
I've just left the intensive care unit of a hospital in Liege, Belgium. It's impossible to know of course, but this is quite possibly the epicenter of Europe's new coronavirus crisis.
The city of about 200,000 residents nestled in eastern Belgium is at around a 41% infection rate, and the hospital is at full capacity. Intensive care unit numbers have tripled in three weeks. Belgium, which had 100 to 200 cases per day throughout June and early July, is now marking north of 10,000. On Oct. 25, it set a daily record with 17,709.
We stood outside one room -- which patients are now forced to share due to overcrowding -- to hear the groans of an elderly man who was just admitted. As doctors and nurses attended to him another ambulance swept up outside the window with another case.
The doctor guiding us on a tour admitted a chilling fact: health workers here (including himself) are now treating patients knowing they themselves have COVID-19.
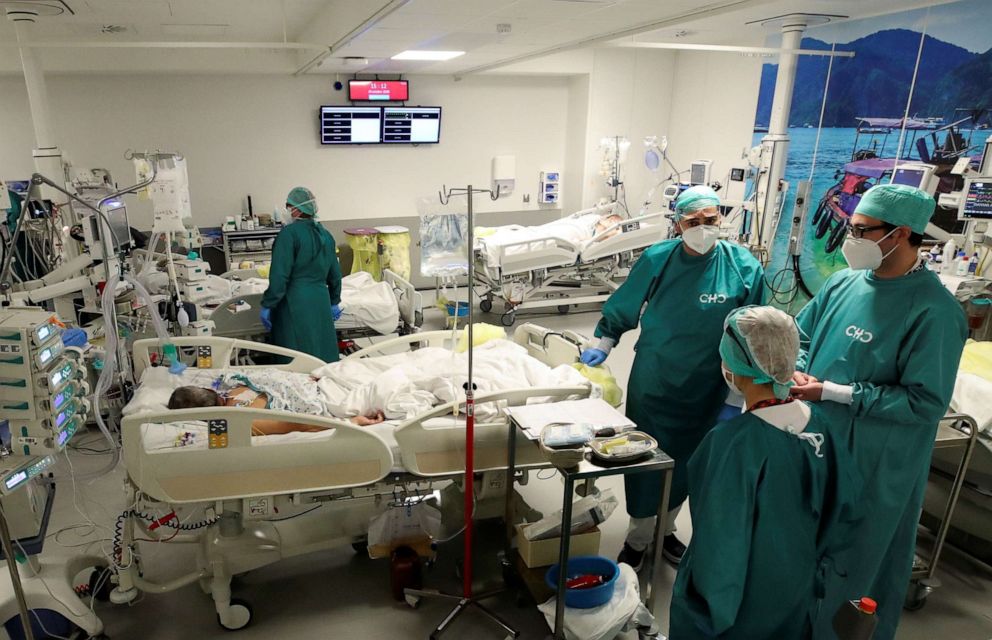
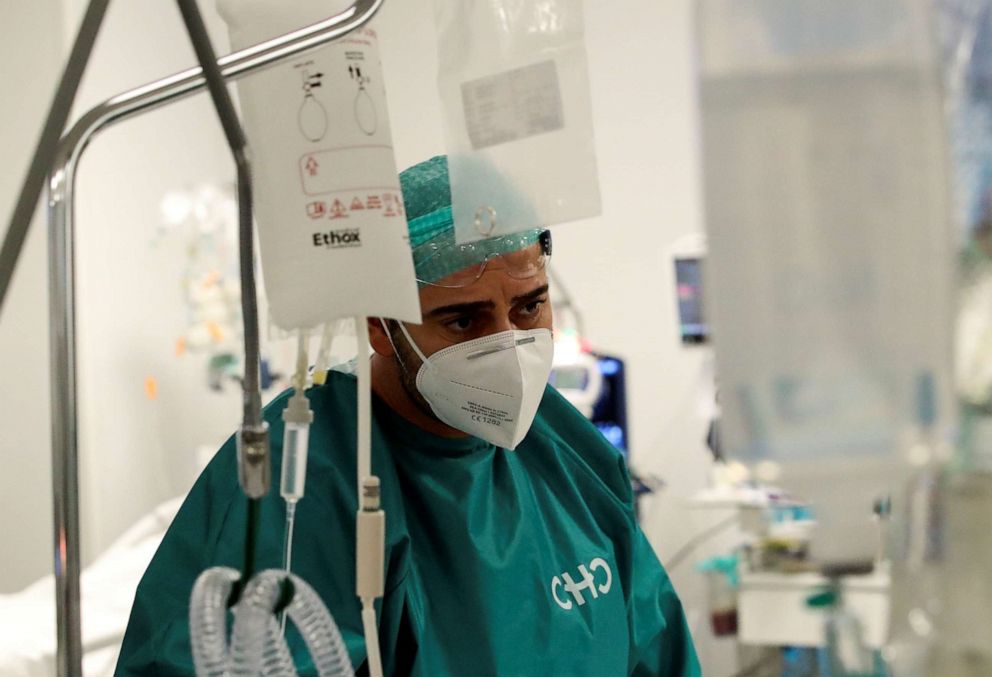
It's an ethical dilemma, but not a choice this doctor could make. He now tests negative, but he said if he and others like him do not continue working, the health system here would go under. The toll on health workers, already exhausted from the first wave, about to be exacerbated by the second.
Why is it so bad? COVID fatigue, he says. Belgium relaxed the measures that had kept the country safe and now are going to pay a price. Lots of testing, yes. But not so much tracing.
But they have learned some important lessons from the first wave.
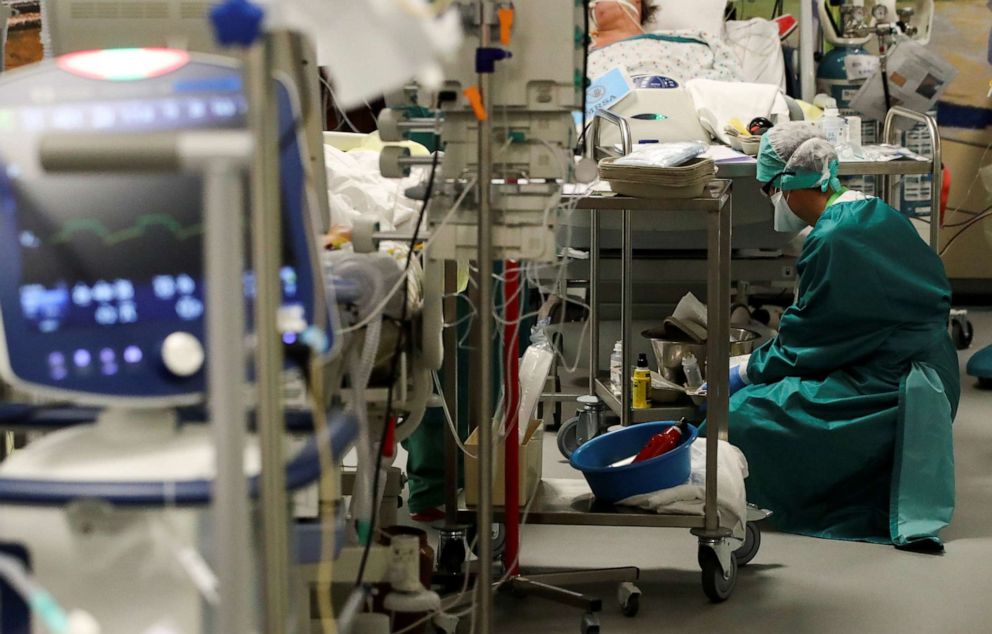

We came across Florent, a 75-year-old man in the ICU who said he wanted to speak to us. Back in March, he would have been ventilated. Now, he has a far less intrusive treatment, and got life saving steroids early on. He may not have survived in March.
Yes, treatment is improving, but the bottom line is that Florent still needed a bed. And at this rate, Belgium is going to run out of them.
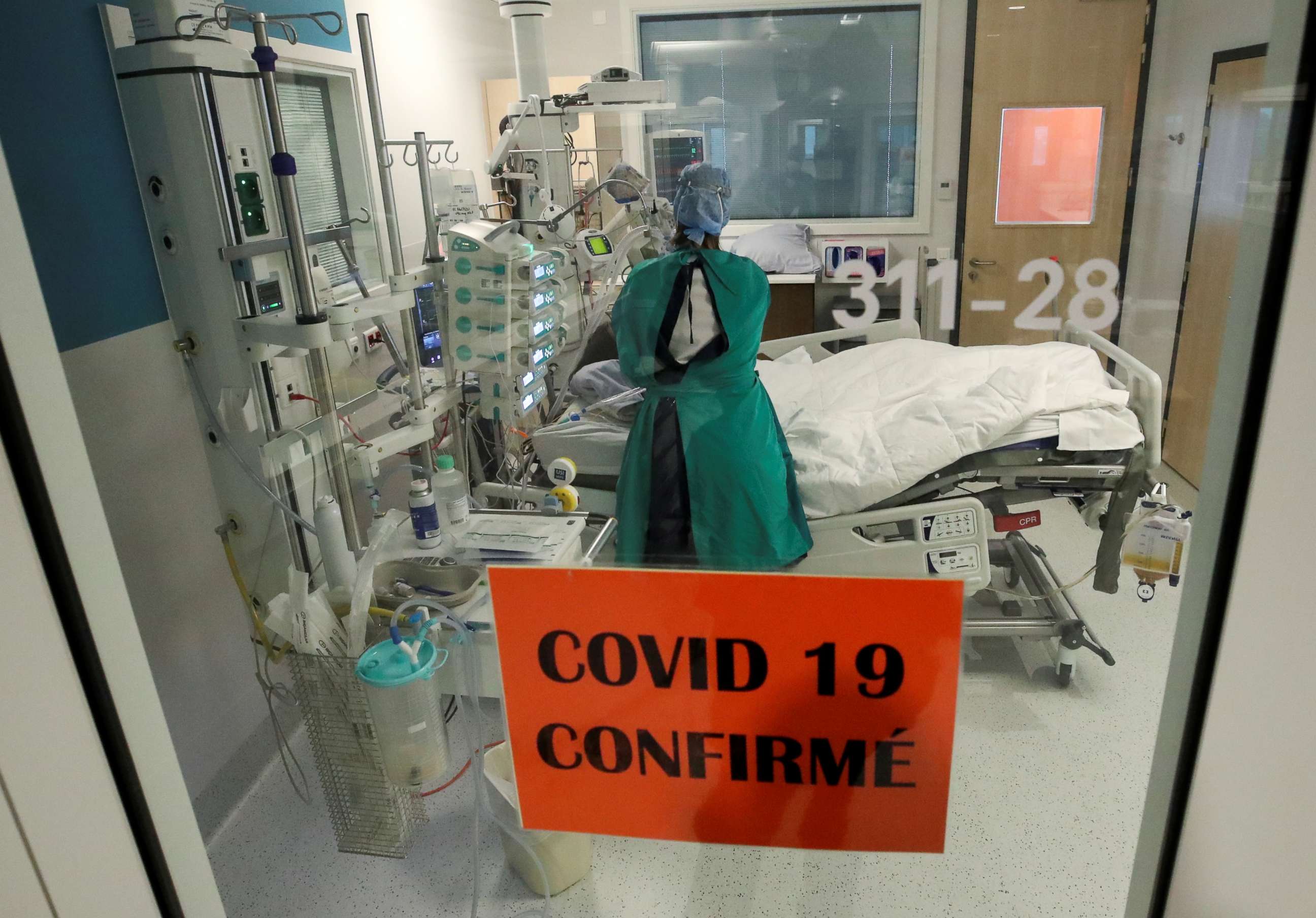
"It's my birthday today," he said, standing up to show us he could.
"What do you wish for?" I asked.
"To go home," he said.




