In communities of color, one organization is helping to fill the COVID-19 testing gap
“Our patients are immigrants like us,” said Dr. Ramon Tallaj, founder of SOMOS.
In a predominantly Latino neighborhood in the Bronx, New York, doctors working through the non-profit group SOMOS Community Care have spent months on the frontlines of the coronavirus pandemic.
Now, those same doctors are traveling to other cities around the country that have been seeing surges in new COVID-19 cases in an effort to get free testing to communities of color, which have already been hit disproportionately hard by the virus and face scarcities in access to testing as well.
One of these doctors is Dr. Jacqueline Delmont, chief medical officer of SOMOS, who has been working for free operating a pop-up free testing site in Miami Lakes, Florida for the past two weeks.. The doctor, who is originally from Venezuela and has devoted her career to helping fellow immigrants, said “the moment” they arrived, people were lining up as early as 4 a.m. to get tested.

The pandemic has pushed Delmont to use all the skills she’s learned during her career.
“It’s an unprecedented time. … I’ve been able to use my administrative skills, but my clinical skills, the empathy coming from a family with limited resources, understanding that there are definitely differences in the communities in terms of access to information, to medication, to mobile devices, to appropriate internet,” she said.
Dr. Yomaris Peña, a volunteer with SOMOS, said working at one of the organization’s testing sites is “another mission where I’m helping my Hispanic, my Latinos, my African American family … everyone that is underserved.”
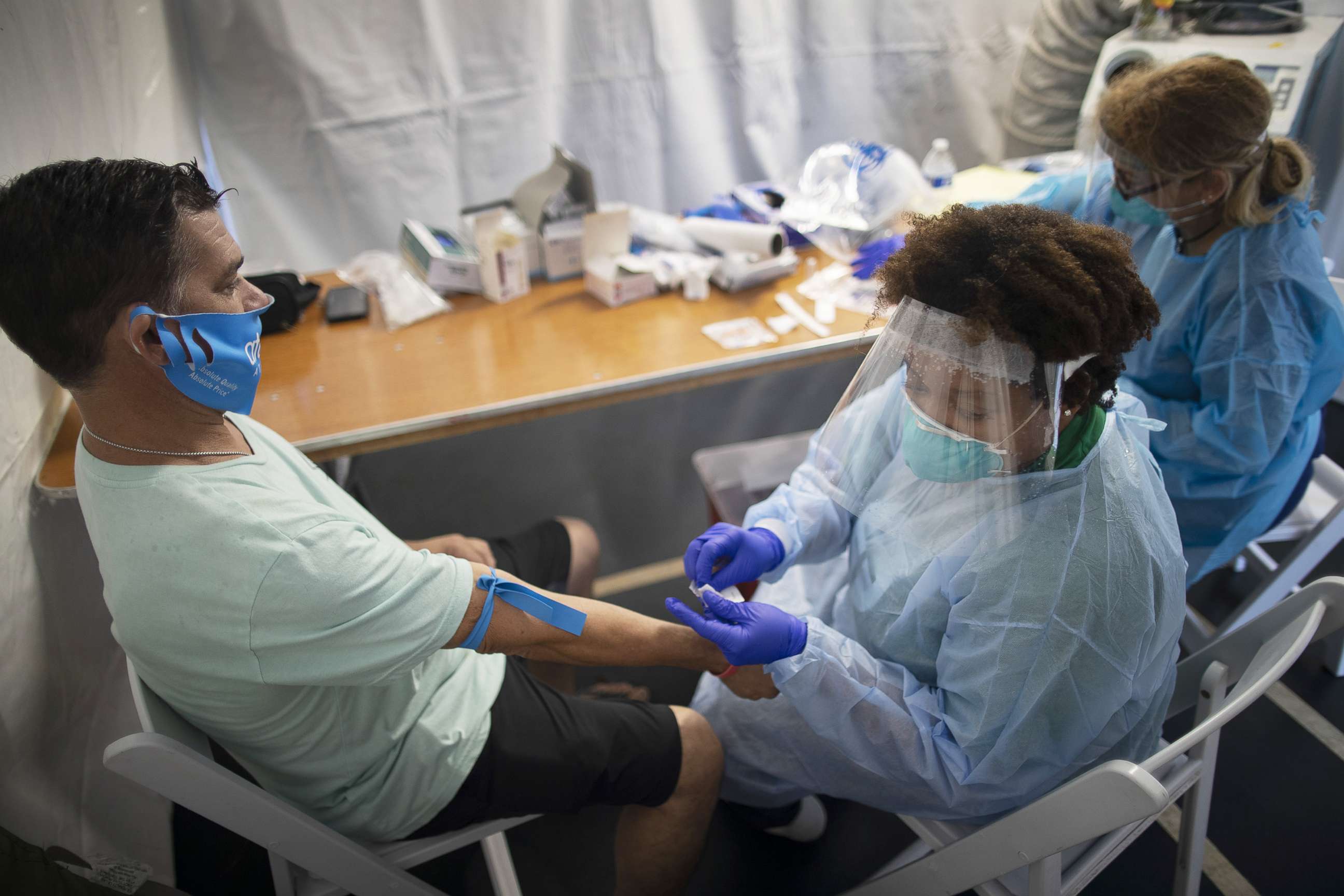
Medical experts have said testing is a key tool in stopping the viral transmission of COVID-19. Yet, an ABC News and FiveThirtyEight review review of U.S. Census data and testing site info throughout the 50 states and the District of Columbia found that in many cities, testing sites in and near predominantly Black and Latino neighborhoods were likely to serve more patients than those in predominantly white neighborhoods. The review also found disparities between richer and poorer neighborhoods, with testing sites scarcer in poorer ones.
It noted “particularly” large disparities in testing access in and around many cities, so called urbanized areas, like San Antonio, Baltimore, Los Angeles and Miami.
“It’s devastating that the communities that need it the most, the communities that have been most affected, the communities that we could have made a greater impact in controlling the pandemic, have not had the access to testing,” Delmont said.

She said it’s “very disheartening” being unable to test many within these communities early because it doesn’t allow them to be proactive in isolating those who become ill. With many people in these communities living with their families -- including elders -- this puts them at risk.
Natalie Choy, 16, recently received a second COVID-19 test two weeks after her first one came back positive. She says her whole family has been sick with the virus, and hopes the second test will give her the all clear.
“My mom, my dad, my little brother and then my two little baby siblings and my grandpa all live with me, and pretty much everyone experienced symptoms, including the babies,” Choy said.

She said it was easier to social distance inside the house when it was just her father who was sick -- he was the first to test positive. Once other people in the family contracted the virus, it became more difficult. “I share a room with my brother, so it wasn’t realistic at all. We really couldn’t do anything at all except wear a mask. We still do.”
The SOMOS testing sites have also helped people who otherwise may not be able to afford testing have access to the service.
“People who can have the money and the things just to be able to pay for every single test, they have much easier access. … That’s fine, but when it’s five, six or seven people, some people simply can’t afford it.”
Delmont pointed out that some families have other obstacles to receiving these services.
“Many patients have lost their insurance. They fear that they’re going to get a bill. Many of them are undocumented,” she said. “We understand that the federal government is not necessarily covering these tests for undocumented [immigrants].”
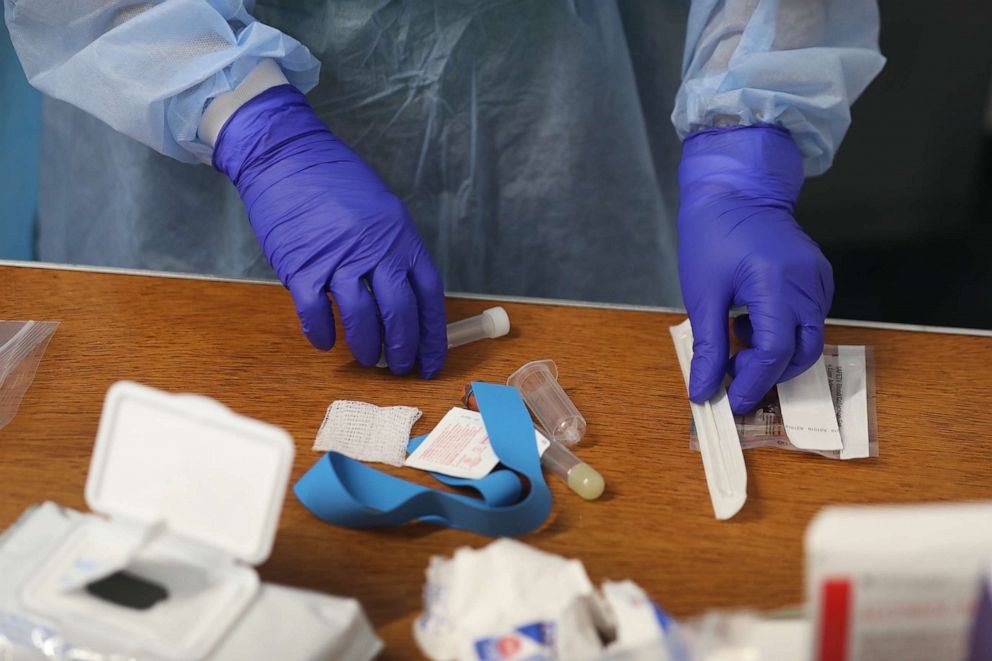
Carmen Guerra, an associate professor of medicine at the Perelman School of Medicine at the University of Pennsylvania, specializes in health disparities. She says that for people who don’t have insurance, “the only other options are to rely on publicly funded means of testing, whether that’s through public health sites in your city or town, or through philanthropic funds.”
SOMOS is one of the organizations around the country that has been there to fill in these gaps. In Houston, Sonia Gomez’s husband had been reluctant to get a test despite their family showing symptoms of the virus.
When they arrived at SOMOS’ Houston site, she said her husband was “very happy that they weren’t asking for any information about … status or papers.”
Gomez said she drove 30 minutes to get to the testing site and that they were taken in quickly by SOMOS doctors -- she said she had tried other places and the wait was about three to four weeks “because the testing sites are very full right now.”

A few days after receiving a test, Gomez tested positive for the virus.
“It was very shocking and scary to know that all of us are tested positive and it’s so dangerous. People are dying. It’s just crazy,” she told ABC News.
SOMOS was founded in 2015 by Dr. Ramon Tallaj after he immigrated to the U.S. from the Dominican Republic in the 1990s, and now has over 2,500 doctors who can speak five languages with their patients.

“Our patients are immigrants like us,” he said. “We speak the same language. We know exactly what’s their problem about housing, money, jobs. Then we had to work with them in any way possible.”
When the pandemic first swept through New York City, the Bronx was the epicenter of the epicenter, and SOMOS was there to help -- the organization partnered with New York State to expand to 28 additional sites. As the organization has expanded its efforts to other cities, Tallaj says SOMOS doctors have conducted close to a quarter million tests.
“From the beginning, we’ve been crying to get testing in our community,” Tallaj said. “But we did it ourselves. We put on the line a lot of money … and we want to continue for our own people.”





