STD cases hit record high for fifth year running, as prevention efforts hit by budget cuts
As funding for state and local health services fall, STDs continue to rise.
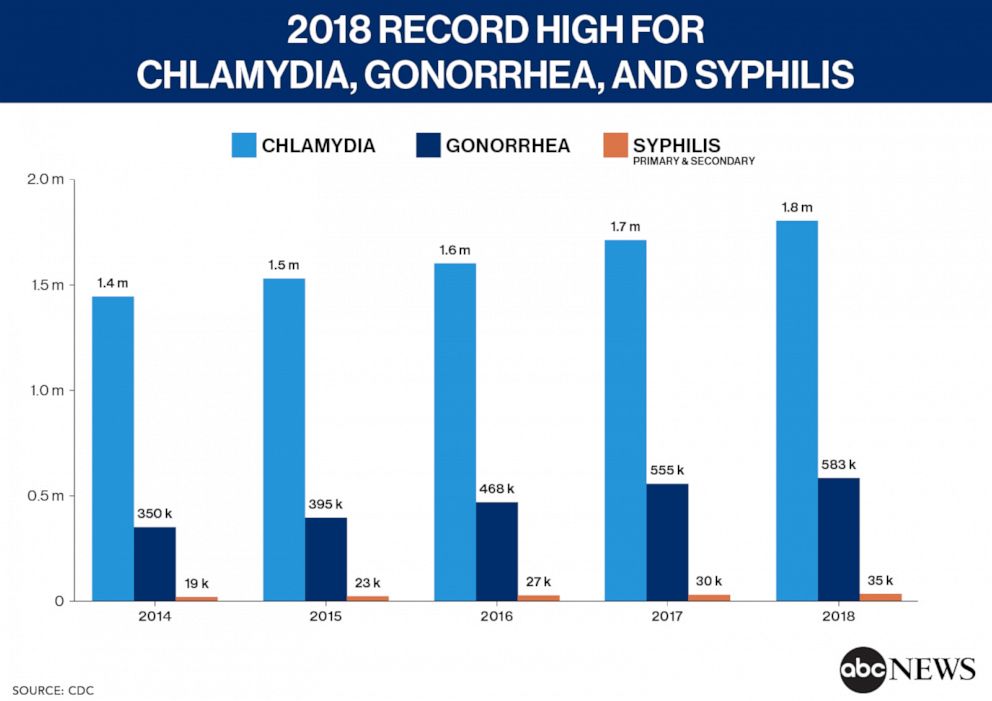
Sexually transmitted infections hit a record high 2.4 million cases in 2018, making it the fifth year in a row that cases of chlamydia, gonorrhea and syphilis have spiked, according to new numbers from the Centers for Disease Control and Prevention.
The agency pointed to the budget cuts that have hit sexually transmitted disease programs in recent years as a driving factor behind the disease spike. Cuts to state and local programs have translated into clinic closures, decreased staffing and ultimately fewer patient screenings and follow-ups.
Over the last five years, chlamydia cases increased 19%, gonorrhea cases increased 63% and syphilis cases increased 71%.
Human papillomavirus virus, which 79 million Americans are infected with, remains the most common sexually transmitted disease.
Most worrying of all was a spike in syphilis transmission from mothers to newborns during pregnancy, which skyrocketed 185% -- to 1,306 cases -- in 2018.
Congenital syphilis, which can lead to miscarriage, stillbirth and severe neurological problems for babies, resulted in 94 newborn deaths last year, a number Dr. Gail Bolan, director of the CDC’s Division of STD Prevention called "startling" in a statement.
The rise in congenital syphilis is especially worrisome because it indicates a breakdown in the health care system, explained Holly Hagan, director of the NYU College of Global Public Health Center for Drug Use and HIV/HCV Infection.
"Where there is good access to regular health care, screening for infectious disease and access to family planning, congenital syphilis should not occur," Hagan added.
Decreased condom use could also be contributing to the increases, experts say, a practice that might be fueled in part by advances in the prevention of HIV transmission.
Pre-exposure prophylaxis, or PrEP, for example, the once-daily pill that prevents HIV transmission, does not offer protection against the spread of other sexually transmitted diseases. In 2016, roughly 80,000 Americans filled prescriptions for the medication.
People on PrEP may take the calculated risk of contracting gonorrhea, chlamydia and syphilis when they have sex without using a condom, because they know those diseases are curable, explained Dr. David Bell, an associate professor of population and family health at Columbia University Irving Medical Center.
"They obviously don't want those infections," he added. "But they do end up taking the risk, to some degree."
The protocol for providers who have patients taking PrEP is to screen those individuals sexually transmitted disease much more frequently than they would otherwise, at least once every three months. There's a possibility that increased screening could be capturing more individuals with sexually transmitted diseases than screenings did when PrEP use was less prevalent.
Bell pointed to the importance of treating chlamydia, gonorrhea and syphilis, in order to decrease their overall prevalence in the U.S. population, particularly in areas of the county with pockets of high STI rates, like parts of the South.
"We have put most of our eggs in the basket around the personal responsibility and personal morality of using condoms. But a major part of prevention should be testing for sexually transmitted infections and curing them," he said. "If we had decreased prevalence our rates wouldn't be going up."

Chlamydia, gonorrhea and syphilis, which can all be treated with antibiotics, can lead to infertility, ectopic pregnancy and increased HIV risk if left untreated. The CDC recommends that boys and girls between the ages of 11 and 12 get vaccinated against HPV, which can lead to cervical, vulvar, vaginal, penile and anal cancers.
Risk factors for sexually transmitted diseases include having unprotected sex, sex with multiple partners and having a previous history of STI infection, according to the Mayo Clinic.
Half of the infections occur in people between the ages of 15 and 24, although men treated for erectile dysfunction medication are also at a higher risk for STIs than the general population.



