Tear gas and protesting amid COVID-19: What you should know
Tear gas could increase the spread of the disease.
As protests erupt across the country in the wake of George Floyd's death, police have been using tear gas on those who are protesting.
These images have prompted a renewed discussion over tear gas, as well as concerns that the noxious chemical may accelerate the spread of COVID-19 through vigorous coughing and excess secretions. This is particularly worrisome in black and brown populations who are already at disproportionate risk of sickness and death from this pandemic.
Riot control agents, more commonly referred to as tear gas, is an umbrella term for chemical substances designed to temporarily impair one's ability to function by causing irritation to the eyes, mouth, throat, lungs and skin, according to the Centers for Disease Control and Prevention.
An example of this available to the general public is the ingredient in pepper spray used for personal protection. Law enforcement entities use the compounds chloroacetophenone (CN) and chlorobenzylidenemalononitrile (CS) for crowd control, usually by releasing it into the air as a smoke, vapor or liquid spray.
Because of dangerous health effects, wartime treaties like the Geneva Conventions, and specifically the Geneva Gas Protocol, banned tear gas compounds following the massive damage caused by chemical warfare in World War I. In the United States, it remains available for use on civilians due to the argument that it decreases reliance on more lethal weapons.
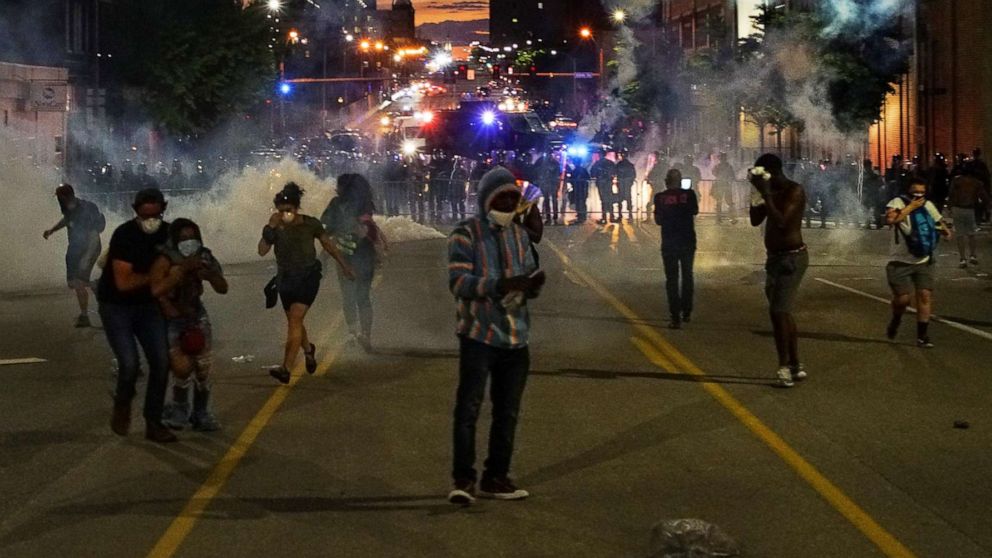
Like most chemical exposures, the impact of tear gas exposure on your body depends on the concentration, duration, location and proximity to source of the exposure.
Immediately, you may develop symptoms such as eye tearing and burning, blurred vision, runny nose, mouth and throat irritation, difficulty swallowing, coughing, chest tightness, difficulty breathing, skin redness and blistering, nausea and vomiting. These typically subside within 15 to 30 minutes following removal from the exposure.
More severe exposure, which occurs particularly with large or repeated doses or in an enclosed space, may result in long-term eye problems (glaucoma, cataracts, scarring, blindness), skin sensitization and chronic breathing problems like asthma. The more rapid effects of severe exposure include fluid build up in the lungs, lung inflammation/infection, respiratory failure and even death.
Those concerned about long-term health impacts should be reassured that, according to the CDC, if you start feeling better within a few hours after you've been exposed, long-term damage is unlikely.
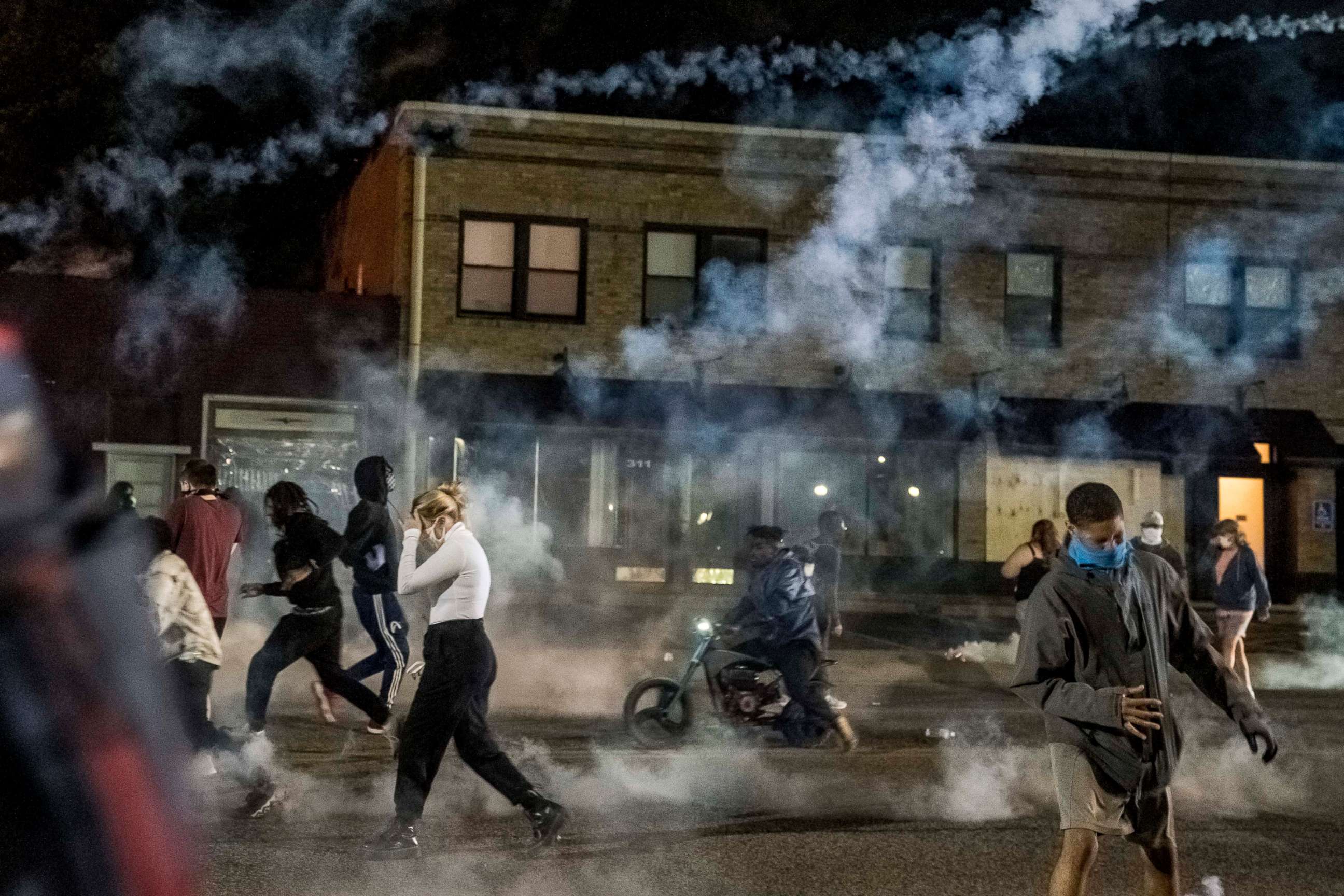
If you've been exposed to tear gas, try to leave the area immediately to get fresh air. If outside, go upwind and to the highest ground possible as the chemicals tend to collect most densely near the ground. Remove your clothing, rapidly wash yourself thoroughly with soap and water and seek medical attention as soon as possible.
If you're experiencing eye irritation, rinse your eyes extensively with water and remove contacts if you have them in. Place all contaminated articles in a sealed bag without touching the contaminated areas and call your local health department for disposal.
As for the links to COVID-19, a list of 1,288 doctors and health professionals signed a letter earlier this week asking for law enforcement not to use tear gas during protests due to an increased risk for spreading the virus.
"These agents are designed for you to cough and expel from the lungs and they can cause lung sickness," Dr. Peter Chin-Hong, an infectious disease specialist with University of California, San Francisco, told ABC News. "We're focused on COVID-19 risks, the biology, but also the coughing, shouting, transmitting the virus more."
Chin-Hong was among those who signed the letter.
"When you have pepper spray or tear gas it increases the risk of not only potentially COVID-19, but also other respiratory viruses," he said.
Jessica Johnson, M.D., is a senior resident in emergency medicine at Stanford University and contributor to the ABC News Medical Unit.




