Clinical trials for coronavirus vaccine begin at University of Oxford
The British government are "throwing everything" at developing a vaccine.
LONDON -- The first patients have been enrolled in human trials for a coronavirus vaccine at the historic University of Oxford after the U.K.’s Health Secretary said the country would be "throwing everything" behind the project.
The clinical trial will test the effects of possible COVID-19 treatments and the start the process of vaccine evaluation in the university’s first human studies.
"There is an urgent need for reliable evidence on the best care for patients with COVID-19," Peter Horby, Professor of Emerging Infectious Diseases and Global Health, and a chief investigator on the study, said. "Providing possible new treatments through a well-designed clinical trial is the best way to get that evidence. Adults admitted to hospital with COVID-19 should be offered the opportunity to participate in this trial and contribute to improving care for everyone. All patients will receive the standard full medical care, regardless of which treatment group they are placed in."
Earlier this week, the Health Secretary Matt Hancock announced a total of £52.5 million (about $65 million) worth of funding for the project, and another vaccine trial at London’s Imperial University due to begin in June.
"Both of these promising projects are making rapid progress and I've told the scientists leading them we will do everything in our power to support," Hancock said at a Downing Street briefing on Tuesday. "After all, the upside of being the first country in the world to develop a successful vaccine is so huge that I am throwing everything at it."
Although the university has urged caution when it comes to mapping out a firm timeline for when the vaccine -- called ChAdOx1 nCoV-19 -- would be in development, a best-case scenario could see for the vaccine’s efficacy determined by fall 2020. Under normal circumstances, even at high speed, it can take between 12 and 18 months to develop a vaccine.

What to know about Coronavirus:
- How it started and how to protect yourself: Coronavirus explained
- What to do if you have symptoms: Coronavirus symptoms
- Tracking the spread in the US and Worldwide: Coronavirus map

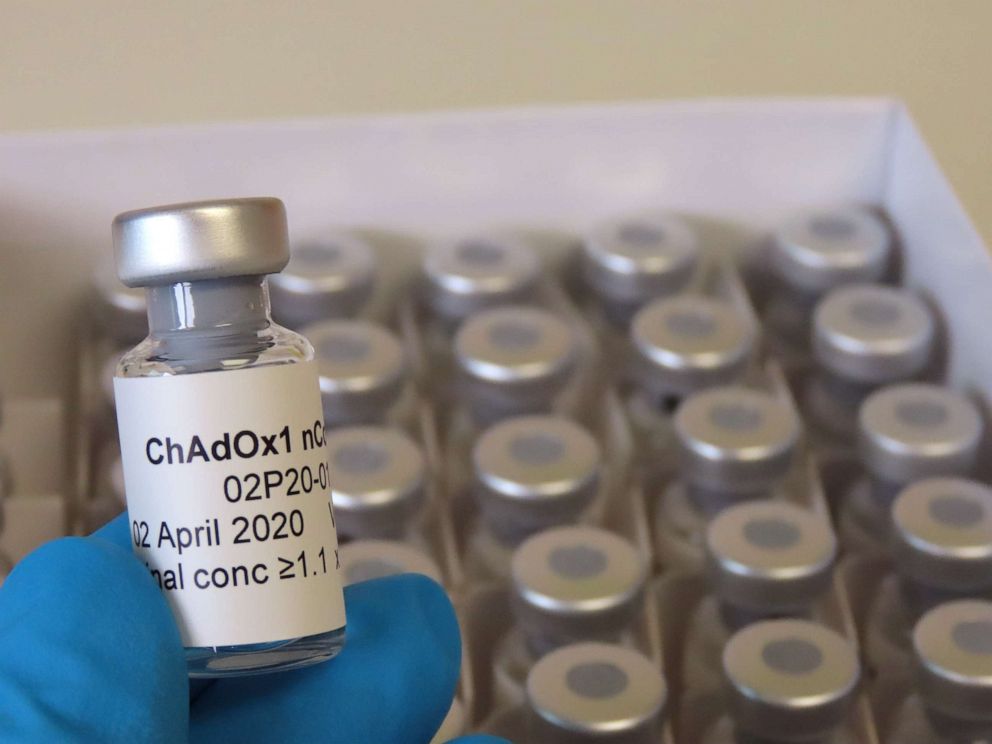
The trial is the result of a collaboration between the university’s Jenner Institute and the Oxford Vaccine Group clinical teams. Work began on developing the vaccine in early January.
Sarah Gilbert, lead researcher of the vaccine development program and a professor of vaccinology at the University of Oxford, noted in a closed press briefing last Friday that Oxford developed the ChAdOx technology as a "platform to make vaccines against lots of different diseases." Last year, they were working on several vaccines including disease X, which was "the name given to an unknown disease that will cause a pandemic in the future."
Her team was putting plans in place to respond quickly, and Gilbert became aware of the outbreak very early in January, designating COVID-19 as disease X.
The Oxford trials currently involve healthy volunteers aged between 18 and 55, but those demographic could be expanded if the trials prove successful. Production of the vaccine is already being scaled up in case the trials are successful for larger trials and future deployment, Dr. Sandy Douglas, who is leading that side of the project, said.
Professor Adrian Hill, director of the Jenner Institute, said that the team had begun "risk manufacturing" with seven manufacturers from across the globe. If the vaccine doesn't work, over 1 million vaccines could be wasted and the money invested lost, he said.
"Starting the clinical trials is the first step in the efforts to find out whether the new vaccine being developed at Oxford University works and could safely play a central role in controlling the pandemic coronavirus that is sweeping the globe," Professor Andrew Pollard, another of the study’s chief investigators, said.
There are more than 80 vaccines currently in development globally, and several therapeutic drugs to treat the novel coronavirus are also in clinical trials, the WHO told ABC News.
"WHO is committed to ensuring that as medicines and vaccines are developed, they are shared equitably with all countries and people," the organization said in a statement to ABC News. Of those vaccine trials, six candidate vaccines are in the clinical evaluation stage, the Oxford University study among them.




