Deeper social issues found in overdose epidemic study
Underlying causes might include broken communities and widespread malaise.
The death toll from drug overdoses in the U.S. is on the rise.
If that seems like a recurring headline, it’s because it is. According to a new study published today in Science, drug overdose deaths have been rising every year from 1979 to 2016 -- long before the mid-1990s surge in opioid prescriptions. Researchers believe that, rather than tied to the popularity of any one particular drug, the increase in overdose deaths could be related to larger societal problems like alienated communities and an increasingly disaffected population.
What did the study find?
After analyzing data from nearly 600,000 deaths attributed to drug overdose from the National Vital Statistics System, researchers saw that the overdoses followed an almost perfectly exponential trajectory over the 38-year period from when the reporting first began in 1979 to 2016. The death rate due to overdoses doubled approximately every 9 years -- by 2016 it was up to one death every 8 minutes.
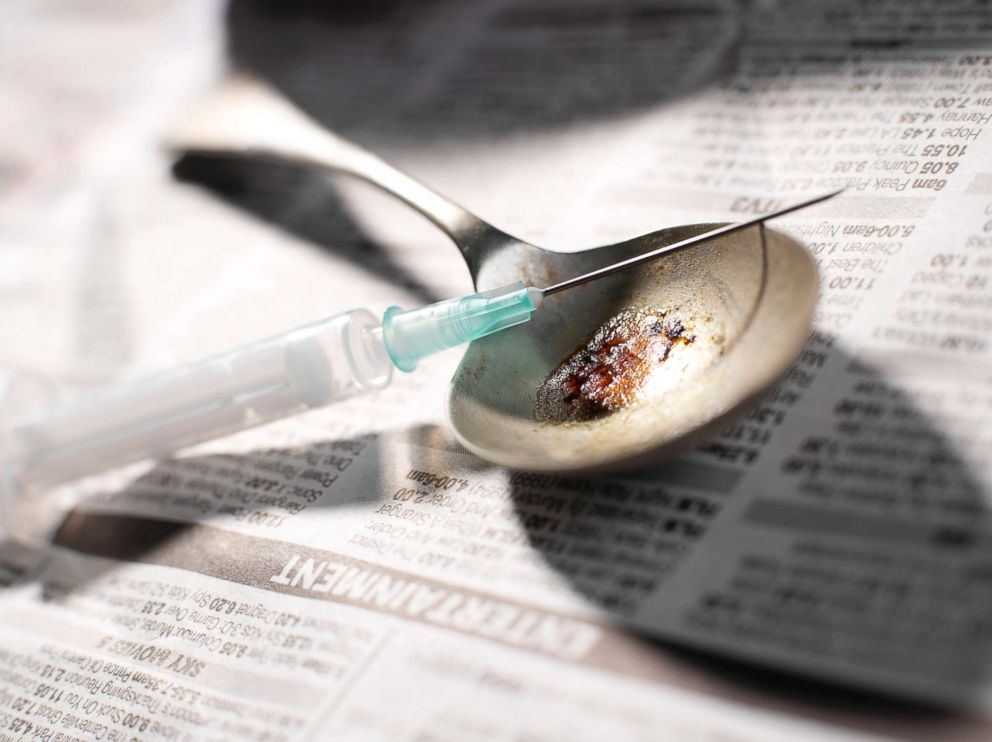
“This smooth, exponential growth pattern caught us by surprise,” Dr. Donald S. Burke, the study’s senior author and dean of the University of Pittsburgh Graduate School of Public Health, said in an interview with ABC News. “It can be hard to grasp what exponential growth really means, but you can think of it as a nuclear explosion: you start with 2 [deaths due to drug overdose], then 4, then 8, then 16, and so on.”
Despite the extraordinarily consistent increase in the overall mortality rate, there was no such predictability when it came to deaths from each particular drug. Cocaine overdose deaths have gone up and down over the last 20 years, the methadone death rate has decreased, and the overdose death rates of prescription opioids, heroin, fentanyl, and methamphetamines have all increased.
For cocaine, the death rate among black men was substantially higher, while heroin caused more deaths in younger white and older black people. Cocaine and heroin more heavily impacted urban centers, and prescription opioids and methamphetamines caused more overdose deaths in rural areas.
Using a technique called heatmapping, the researchers plotted out these overdose patterns across the U.S. Though different drugs tended to dominate in different regions, almost every region nationwide had an overdose “hotspot” for at least one drug.
The research pointed to an unexpected paradox: there has been continuous growth in the overall number of overdose deaths, even while the use of individual drugs seem to rise and fall.
“It implies that there are other forces at work, besides the specific drugs,” Dr. Burke said. “The forces are broader and deeper than we thought, including social determinants of health and technological determinants of health.”
What does this mean for America’s drug epidemic?
The study underlines a concern that the overdose death rate may continue to rise at an even higher rate if underlying issues like drug accessibility and societal malaise aren’t addressed.
“The drugs have become cheaper over the years and their delivery systems have become more efficient… These factors increase drug availability,” Dr. Burke explained. He added that, “people are losing a sense of purpose in their lives and there has been dissolution of communities, making people more susceptible to using drugs—increasing demand.”
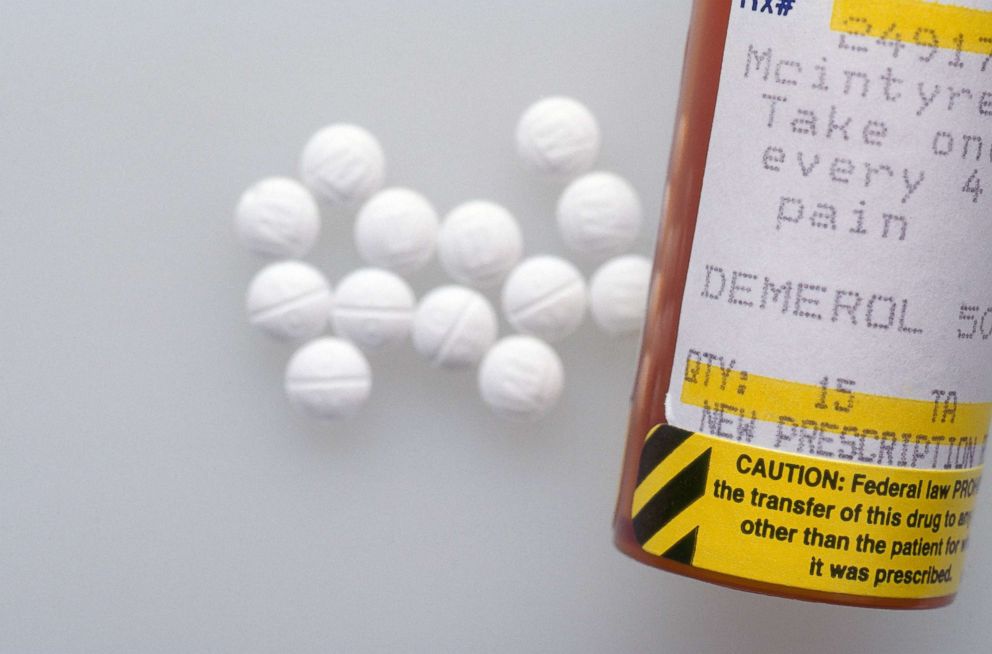
What do the study authors recommend to reverse this trend in drug overdoses?
Dr. Burke said that this new research does not dispute how well public health programs designed to decrease opioid-related deaths work, such as scaling up addiction treatment programs and increasing the public availability of naloxone, a medication that reverses the effect of opioids. “Those programs will undoubtedly make a difference for individuals,” Dr. Burke said.
But the study does suggest that those methods may not be enough to affect the big picture.
“If we solve the [opioid] sub-epidemic, will there be another sub-epidemic that comes on its heels?” said Burke. “If we don’t address the social determinants of health that underlie drug use and addiction, there’s a good possibility that the drug overdoses will start to emerge again.”
Burke stressed that we need to think about questions that lie beyond the parameters of public health as we know it, and have more to do with the broader aspects of our society. “Why don’t people feel a sense of purpose? Why do people not have a sense of community? Why do we appear to be living in an emerging economic caste system in the United States?” said Burke. “These are the issues that need to be addressed. They are in the realms of education, employment, housing… They are not easy problems,” he said.
Dr. Nicky Mehtani is an internal medicine physician at Johns Hopkins Hospital and a part of the ABC News Medical Unit.



