What we know about coronavirus' long-term effects
Other respiratory disease can teach us about the lingering effects of COVID-19.
In the months since the novel coronavirus exploded into a pandemic, we have heard a range of stories about those who have been stricken by the disease -- the vast majority with mild symptoms, but an increasing number needing to be hospitalized.
But what about those who were reported to have recovered from the illness, which has no inoculation or cure?
While the telltale symptoms of coronavirus, including fever, dry cough and shortness of breath, have been well-publicized, there's been less information about the long-term health of people who contract COVID-19 and recover.
In part, that's because the virus is new. The first cases emerged in Wuhan, China, in December, so even the very first people who contracted COVID-19 and recovered are less than six months out from when they were initially infected.
Still, there are insights we can glean from preliminary data about COVID-19 patients in the United States released by the Centers for Disease Control and Prevention (CDC), and from what we know about the long-term effects of other respiratory diseases, experts say.
What other respiratory diseases can tell us about COVID-19
Roughly 80% of COVID-19 cases reported in China, were considered mild, according to the CDC.
Dr. Shu-Yuan Xiao, a pathology professor at the University of Chicago School of Medicine, stressed that most patients who have mild illness should recover "with no lasting effect."
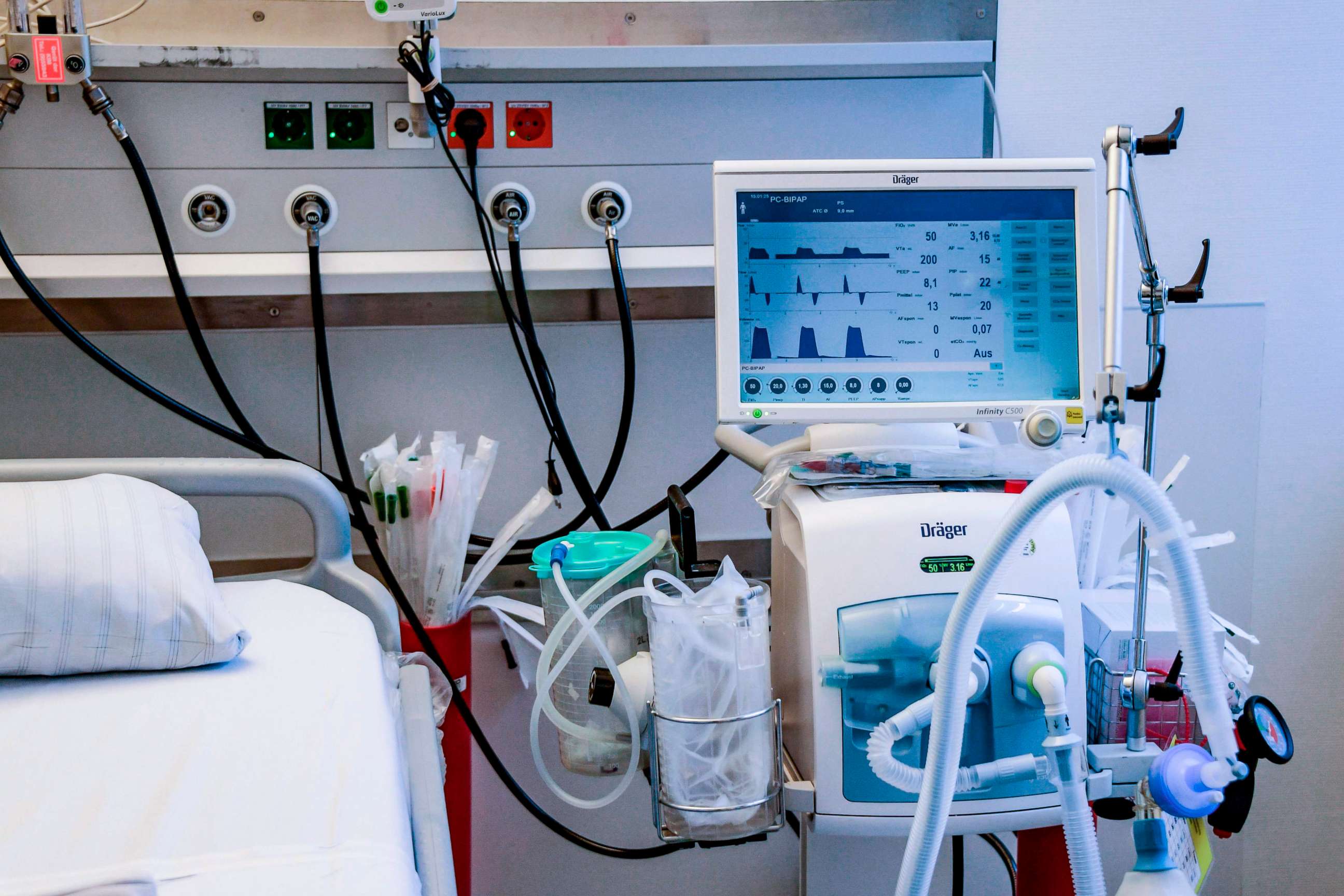
Patients who have a more severe illness but recover without needing to be put on a ventilator should also be free of long-term side effects, he added.
"For the 16-20% of symptomatic patients who eventually need ICU care, it is difficult to predict," he said, referring to the percentage of those hospitalized who will need critical care.
Patients who go into the intensive care unit and need ventilators are more likely to have lung damage and to develop acute respiratory distress syndrome (ARDS), a severe lung condition in which fluid collects in the lungs' air sacs.
"Based on experience from SARS and MERS, some patients may develop lung fibrosis," Xiao said, though he noted that lung fibrosis, which is when lung tissue becomes scarred, has not been observed in the limited studies we have so far about COVID-19.
"In China, some patients eventually needed to be on [an ECMO life-support machine], to temporarily support the patients while they regain lung function," he said. "However, some of them [may] never regain lung function."
According to a study published in the Journal of the American Medical Association published in February that examined 138 patients in Wuhan, China, 10% of those in ICU care were eventually switched to ECMO machines, which remove the blood from the body, oxygenate it and then return it to the body.
While those long-term effects sound frightening, the reality is that lingering health consequences among people who contract severe respiratory diseases are common.
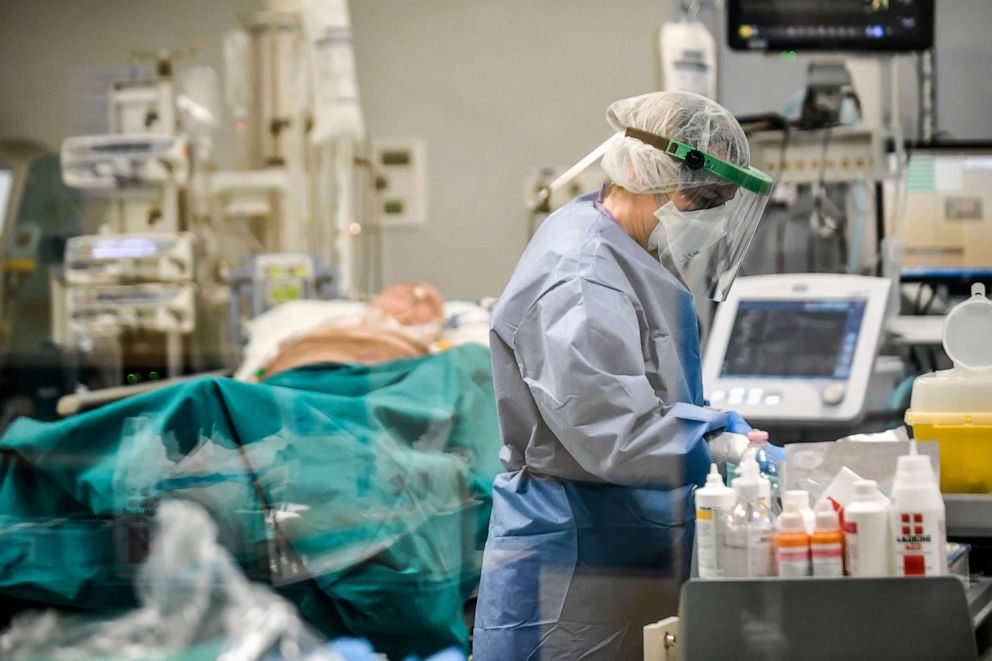
"It's the same general thing that you have with any type of phenomena that's severe enough to land you in the ICU," said Dr. Amesh Adalja, an infectious disease and critical care expert at Johns Hopkins Bloomberg School of Public Health.
"There's a lot in common with what we do for non-COVID respiratory failure that's going to be applicable here," Adalja said.
For people who are put on a mechanical ventilator, it's likely to be several months to a year before they recover full lung function, he explained. Some may never recover that functionality.
"It's not a one-size-fits-all situation," Adalja said. "How much lung tissue was destroyed by the virus? That would translate into having increased shortness of breath."
What to know about Coronavirus:
- How it started and how to protect yourself: Coronavirus explained
- What to do if you have symptoms: Coronavirus symptoms
- Tracking the spread in the US and Worldwide: Coronavirus map
Both Xiao and Adalja emphasized that much more research is needed before we know how recovered COVID-19 patients severe disease fare months or years out.
"I hope there [will] be more autopsies performed on patients who died of the disease, to provide better knowledge," Xiao said. "Currently, we know so little about the spectrum of COVID-19 pathology."
Some COVID-19 patients may also develop heart problems and blood clots
In addition to the potential for COVID-19-related lung damage, preliminary data out of China indicates that patients who contract the disease may also be at risk for heart problems.
A study conducted in Wuhan, China, found that 20% of patients hospitalized with COVID-19 had heart damage, a condition that was associated with a higher risk of in-hospital death.

It's unclear whether those heart problems are caused by the virus itself, since severe illness of any variety can trigger heart problems.
"Someone who's dying from a bad pneumonia will ultimately die because the heart stops," Dr. Robert Bonow, a cardiology professor Northwestern University's Feinberg School of Medicine and editor of JAMA Cardiology, told Kaiser Health News."You can't get enough oxygen into your system and things go haywire."
Increased blood clotting is another growing concern for doctors. In Spain, one of the countries hardest hit by the pandemic, blood clots among COVID-19 patients became so common that doctors began treating everyone with anticoagulation medication.
"In the beginning of the outbreak, we started only giving them medicine to prevent clots. We saw that it wasn't enough," Dr. Cristina Abad, an anesthesiologist at Hospital Clínicos San Carlos in Madrid, told ABC News. "They started having pulmonary embolisms, so we started anticoagulation on everyone."
What we know about severe COVID-19 cases in the US
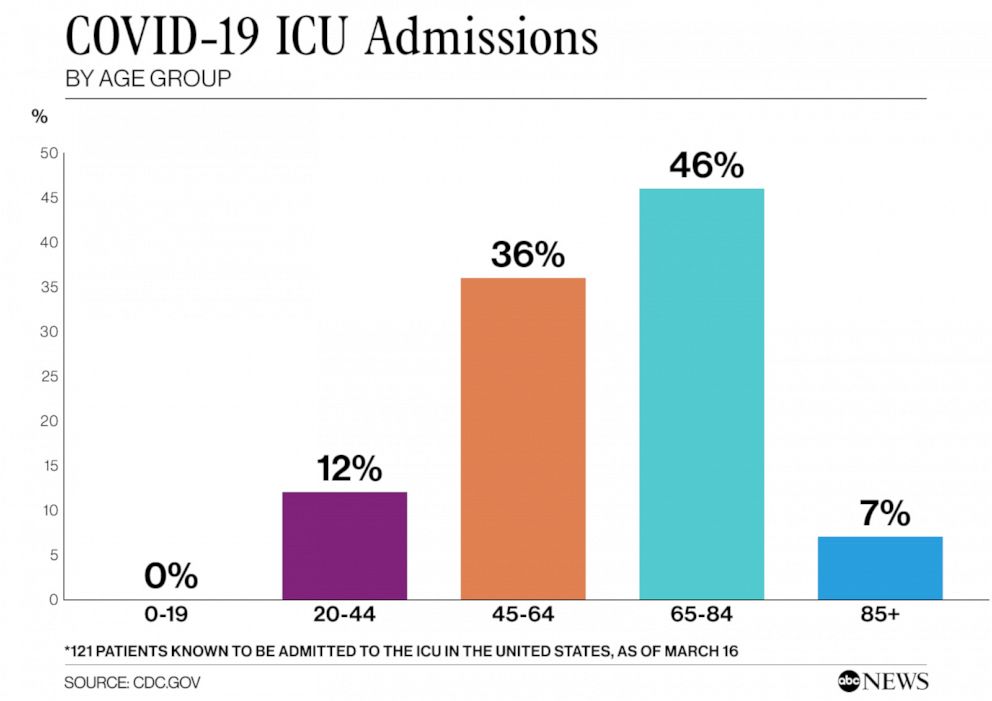
Of the 121 U.S. patients admitted to an intensive care unit for COVID-19 as of March 18, when the epidemic was just starting to accelerate in the U.S., 7% of patients were older than 85, 46% were 65 to 85 years old, 36% were 45 to 64 years old and 12% were 20 to 44 years old. None of the patients in the CDC report, which was published March 18, were younger than 19.
Despite those figures, "severe illness leading to hospitalization, including ICU admission and death, can occur in adults of any age with COVID-19," the report notes.
The long-term effects of being put on a ventilator could become a reality for hundreds of thousands of Americans. The Society of Critical Care Medicine projects that as many as 960,000 Americans may need to be put on ventilators during the course of the outbreak in a worst-case scenario.
That doesn't mean everyone who needs a ventilator will get one.
As it stands, Johns Hopkins Center for Health Security estimates that there are only 160,000 ventilators currently available for patient care, and 8,900 in the national stockpile.
ABC News' Sasha Pezenik and Lily Nedda Dastmalchi, D.O., M.A., an internal medicine resident physician at George Washington University and a contributor to the ABC News Medical Unit, contributed to this report.