Early mortality rates for coronavirus are likely misleading, experts say
Children and adults have done extremely well in terms of recovery, say doctors.
It's possible that COVID-19 isn’t as fatal as most people think. And stockpiling hand sanitizer and masks could hurt people who are truly at risk: the elderly and those with weak immune systems.
“Kids and adults have done extremely well in terms of recovery so far,” said Dr. Jeremy Faust, an emergency medicine doctor at Brigham and Women’s Hospital in Boston. “It’s so critical that we do not waste resources among the young and healthy and that we really focus on the areas where this might really get out of control.”
Dr. William Schaffner, professor of preventive medicine and infectious diseases at the Vanderbilt University School of Medicine in Nashville, says our understanding of the disease is still developing and the statistics are preliminary.
“They’re all estimates," he said. "What are you counting as a case in your particular country? ... That case definition has varied a lot.”
Tune into ABC News Live at noon ET every weekday for the latest news, context and analysis on the novel coronavirus, with the full ABC News team where we will try to answer your questions about the virus.
While some studies peg the death rate to 3.4%, experts expect to see this rate decrease as the health care system starts finding milder cases.
“What I was able to find by looking at a few other data sources, rather than just the big flashy numbers, was that there’s actually a lot of reason to be reassured that the numbers are a lot lower,” said Faust.
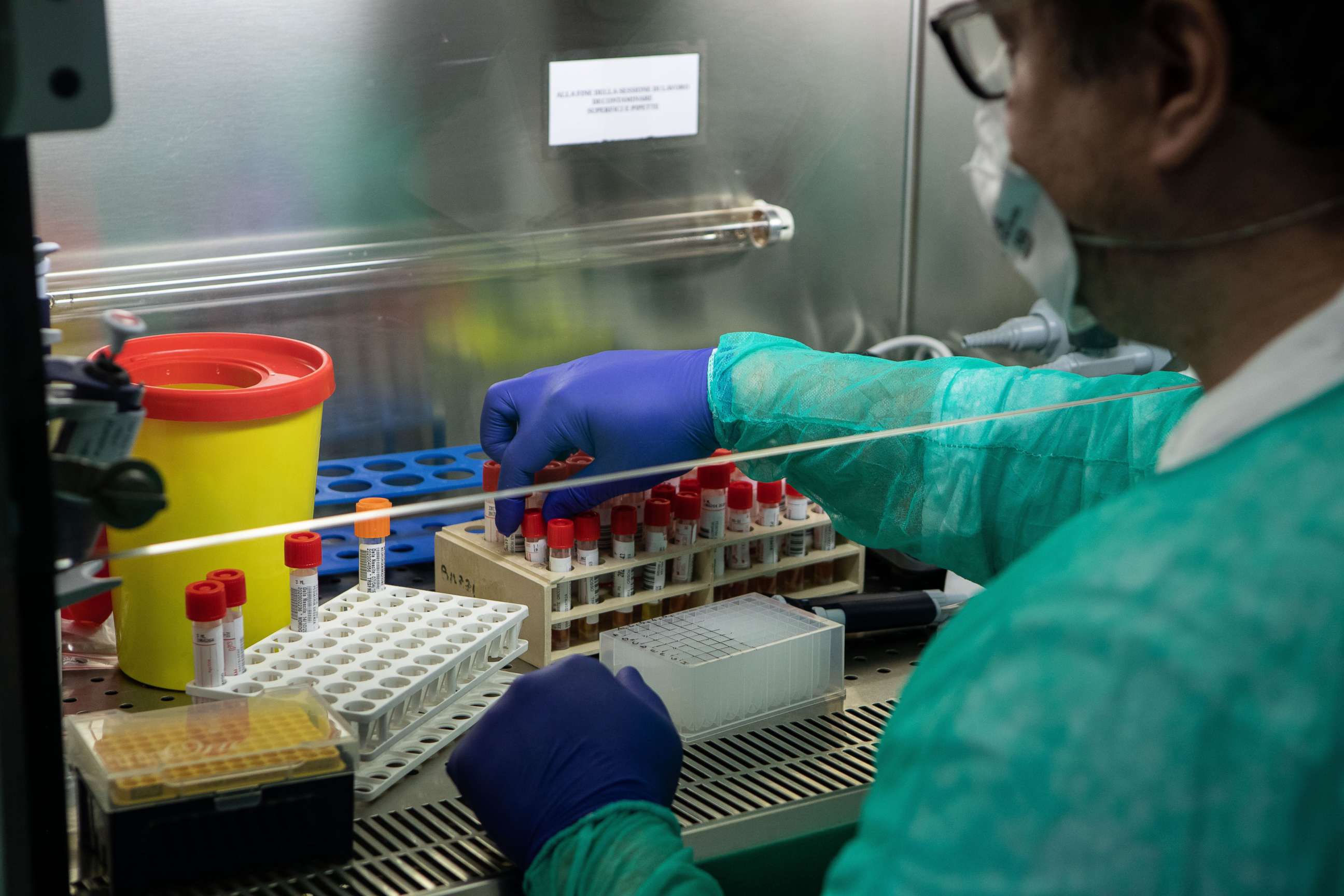
Because only the sickest people are showing up at hospitals, this group is likely over-represented among the full population of people who have COVID-19, according to Faust. Most COVID-19 cases are mild, and many individuals will never even see a health care provider to be tested.
“If you get to people over 70, we’re going to have much higher fatality rates. And I’ve seen some estimates of even as high as 10%, which would be huge for people 70 and older,” said Schaffner. “But remember, those people accumulate a whole lot of underlying illnesses, which adds to their risk. They have heart disease, diabetes, lung disease ... Some of these people, particularly from China, have lived in polluted environments their whole life. Some of the men, especially, have been lifetime smokers. So they are at very increased risk of severe disease.”
The recent quarantine aboard the Diamond Princess cruise ship in Japan might provide a greater insight into the age-specific nature of COVID-19’s mortality rate, according to Faust.
“If you had an outbreak on a cruise ship, and there’s any sign that care was delayed or that people who really should’ve been protected weren’t, then you actually have reason to say ‘Oh, actually, whatever we found on the cruise ship, it’s actually that’s the worst case scenario because they didn’t get treatment on time.’”

Of the 705 passengers who tested positive for the virus on the Diamond Princess, six died -- which is a death rate of less than 1%. All of the patients who died onboard were more than 70 years old.
“In China, about 12% of cases were in the elderly," said Faust. "On the Diamond Princess, four times that many older people had the disease. So again, if you’re trying to figure out what this means for the entire population, it might even mean that the overall fatality rate would be lower."
Right now, death rate estimates vary per country. The best estimates for South Korea put COVID-19's fatality rate at 0.6%, and a recent study released on the death the rate in China -- but outside hard-hit Wuhan -- hovered just above that, at 0.7%.
Right now, the best experts can say is that COVID-19 is probably more deadly that the seasonal flu, but much less deadly than other high profile outbreaks like Ebola, SARS, and MERS, with death rates of 50%, 10%, and 35%, respectively. The Center for Disease Control is planning to set up a national surveillance reporting system in 8 to 12 weeks, which will help to establish a more reliable mortality rate.
“There’s a large epidemic of coronavirus anxiety,” said Schaffner. "I think [people] ought to take a deep breath and spend a little more time planning what to do if the coronavirus really came into their community and they had to undergo what we call social distancing, which is separating themselves from other people. If you do this now when you’re more calm, it works much better when you really have to apply it rather than planning in a more anxious moment later on.”
Priya Amin is a masters degree candidate at Columbia University in Narrative Medicine and a member of the ABC News Medical Unit.




