Officials confront challenges to get public to take COVID vaccine
"Vaccines don't save lives, vaccinations do."
With the authorization of a COVID-19 vaccine in record time and plans for a large-scale deployment underway, public health officials now confront a new and complex challenge, how to convince Americans to actually take it.
“Vaccines don't save lives, vaccination does,” said Dr. Richard Besser, CEO of the Robert Wood Johnson Foundation, a former acting director of the Centers for Disease Control and Prevention, and a former ABC News chief medical correspondent. “If no one wants to receive it, we're going to be wearing masks, washing our hands and social distancing for years to come."
The first doses of the Pfizer and BionNTech vaccine are rolling out to injection sites across the crisis-wary nation, after receiving emergency authorization from the Food and Drug Administration Friday night. No vaccine in history has ever been developed so fast. But that speed is also the problem. When it comes to medications, doctors know that people often think “reckless” when they hear “fast.”
“It's a brand-new virus that thrust itself upon society,” Dr. Anthony Fauci, the nation's top infectious disease doctor, told ABC News for the 20/20 special, “THE SHOT: Race for the Vaccine." “So, it's our job to convince the American public what the truth is.”
Diminishing the reluctance won’t be easy, experts say. It’s entangled in decades-old hesitance in taking vaccines, longstanding systemic racial inequity, fears of unknown side effects -- fears abetted in the modern era by conspiracy-minded internet recesses stoking anti-vaccine sentiments, amid a bitter partisan divide in the country.
“The anti-vaxxer movement has gained incredible traction, especially with the advent of the Internet and social media,” Dr. John Brownstein, chief innovation officer at Boston Children’s Hospital, Harvard epidemiology professor and ABC News Contributor.
“The ability to share misinformation has grown exponentially, to the point where we've seen issues with vaccine hesitancy and uptake in communities across this country,” Brownstein said. “It's a real concern.”
Confidence in the vaccine’s safety sharply sank through months of partisan rhetoric about the vaccines’ timeline, even as cases surged. Muddled messaging and politicization of the pandemic exacerbated leeriness about current government’s intentions, health experts told ABC, with promising new treatments and mitigating health measures turned into partisan footballs.
Polls through the fall showed many Americans were reluctant to take a hypothetical vaccine; by mid-September, just over half of U.S. adults (51%) said they would definitely or probably get a vaccine were it available today, according to Pew Research Center -- a 21 percentage point drop from May. As President Donald Trump repeatedly insisted a vaccine could be authorized by Election Day, public health experts, including seven former FDA commissioners, warned that the administration was undermining the agency’s credibility, and that any attempt to “tip the scales” of the vaccine would hurt public trust and could derail progress out of the pandemic.
The head of Operation Warp Speed, Moncef Slaoui, voiced concern Friday over reports the Trump administration had posed an ultimatum to FDA commissioner Stephen Hahn to push authorization through, or risk his job, saying it could open the door “for people to see undue pressure” on the vaccine.
Hahn has disputed claims that he had swayed by any pressure, telling ABC News’ Martha Raddatz on “This Week” that “science and data” would solely influence the vaccine’s rollout.
“We promised the American people that we would do a thorough review of the application,” Hahn said. “And that's what we did.”
There are new indications faith may be on the mend. A new ABC News/Ipsos poll released Monday found that more than 80% of Americans planned to get the vaccine, either when immediately available, or eventually. It signals growing confidence in the vaccine against a virus that has claimed nearly 300,000 lives across the nation.
Vaccinating a critical mass of the U.S. population is essential to make a dent in the pathogen’s spread, infectious disease specialists say, with “herd” immunity reached with around 70% of the population inoculated.
Experts say, there’s work to be done to ensure that happens. As distribution of the first 2.9 million doses kicks into gear, public health experts prepare to parse fact from fiction.
“I think it's okay to be scared,” ABC Chief Medical Correspondent Dr. Jen Ashton said. “It's okay to acknowledge that - it means you've been paying attention. But in medicine and science, we have to go on facts, not fear.”
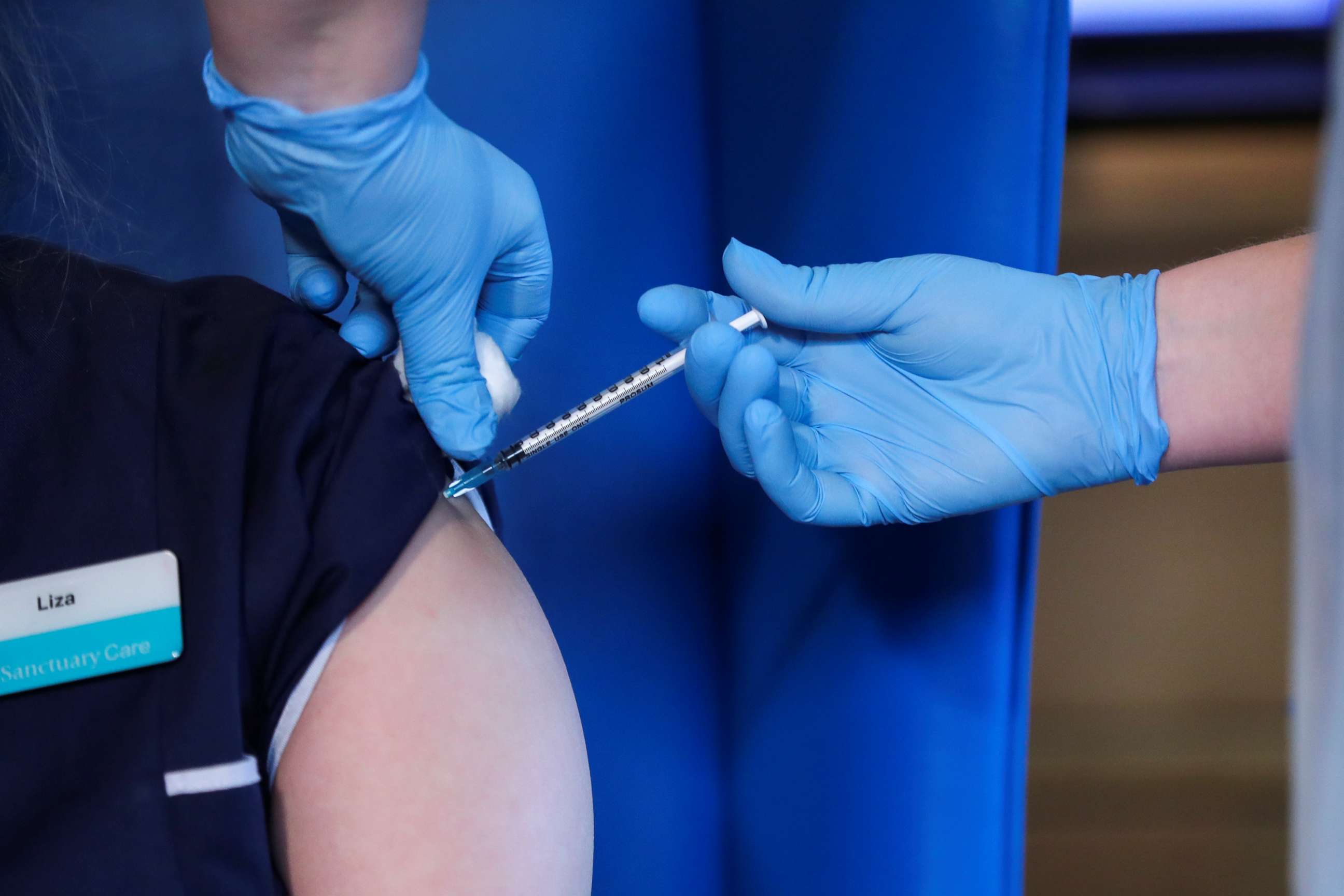
After undergoing rigorous safety trials, the Pfizer vaccine is estimated to be 95% effective. It is the first vaccine that uses the genetic technology mRNA to be authorized in the United States; the Moderna vaccine not far behind, also showing nearly 95% effectiveness. Both are made from molecules that encode the virus’ “spike protein,” priming the immune system when challenged by infection. No vaccine of its kind had ever been used in a mass immunization campaign -- but years of research enabled scientists to develop the vaccines in record time. Once the virus’ sequences were revealed in January, it took just days to create both mRNA vaccine candidates.
With wide distribution and acceptance, “we could crush this outbreak very similar to what we did with smallpox, with polio and with measles,” Fauci said.
Smallpox and polio are among the many diseases that have been largely eradicated in the developed world, thanks to vaccines. But when the smallpox epidemic hit the American colonies in the late 1700s, for example, there was resistance to inoculating against it, too.
“People didn't like that they were about to be injected with a biological product they didn't understand, and that was the birth of anti-vaccine movements,” Dr. Paul Offit, director of the Vaccine Education Center at the Children’s Hospital of Philadelphia, told ABC.
In recent decades, anti-vaccine sentiment has continued to grow, experts say, stoked by misinformation and unfounded apprehension about adverse reactions, and built upon a grisly history of medical experimentation, with members of ethnic and racial minorities treated as guinea pigs.
In the digital era, those fears are compounded by the rise of misinformation online. Social media posts containing vaccine misinformation have increased since the pandemic began, and more likely to coexist alongside less extreme, normalizing content, experts told ABC News.
“A rumor that is unfounded can take hold quickly in a community and spread like wildfire,” Brownstein said.
A study published in 1998 - since discredited and withdrawn - associated the measles, mumps and rubella vaccine with autism. But the concern it sparked among parents lives on.
“It spread through the entire globe and had fundamental impact on immunization practices to the point where we've seen resurgence of infectious diseases that we thought were long controlled,” Brownstein said.
In 2019, the World Health Organization listed vaccine hesitancy as one of the top threats to global health, in a world where certain diseases have been considered antique and assumed eradicated.
Across many communities of color, rampant vaccine skepticism has been built by centuries of suffering painful social inequity and medical mistreatment -- an urgent issue especially now in a population which has borne a disproportionate burden of coronavirus’ ravages.
“This low level of trust stems, at least for the Black community, from a history of trauma and mistreatment and misrepresentation,” Dr. Michelle Williams told ABC, dean of the Harvard T.H. Chan School of Public Health.
Historical examples abound. Among them, the infamous Tuskegee study during the mid-20th century. For 40 years, members of the U.S. Public Health Service studied Black men who already had syphilis, who were not told they were sick, and were not treated, so that the disease could be observed taking its course.
“Inclusion of Black Americans in experimentation and in government practices still holds a lot of individuals' imagination," Williams said. "There's a distrust of the messengers and the institutions that have been bringing forward information about the vaccine.”
To help fight the problem, Williams co-founded the nonprofit COVID Collaborative, which commissioned a September study in partnership with Langer Research, UnidosUS and the NAACP. The poll found widespread hesitancy and resistance in Black and Latino communities about the coronavirus vaccine.
In the survey, 14% of Black people said they trusted that a vaccine will be safe, and 18% trusted that it will be effective in shielding them from the coronavirus. Among Latinos, 34% trusted its safety, and 40% trusted its effectiveness. It also found that knowledge of the Tuskegee study was a negative predictor of vaccine uptake, and emphasized that “effective vaccine uptake efforts must consider the historical trauma and distrust not only with vaccination, but with government efforts writ large.”
The survey was conducted before interim data was released, showing that vaccine candidates had achieved high efficacy and appeared safe; experts say now, trust in vaccine safety is vital to promoting its uptake amongst vulnerable populations -- no mean feat, Williams said.
As part of the vaccine development process, experts said it is also vital to enroll a diverse representation in clinical studies for the vaccine. For some, that means leading by example.
“When I was offered the opportunity to be part of the Pfizer trial I was very determined to be part of it, because I was a person of color,” Dr. Victoria Smith, family physician on the Ochsner Health Board of Directors, based in New Orleans, told ABC News. “Knowing how much distrust there can be for health care from people of color,” Smith said she wanted to contribute to a diverse volunteer pool.
Scientists working on the vaccine have also stepped forward, offering reassurances that their teams of doctors and researchers included people of color -- scientists like Dr. Kizzmekia Corbett, Lead Researcher on Fauci’s team at the National Institute of Allergy & Infectious Diseases, who told ABC News, "the onus of gaining the public's trust lies in the hands of people like me,” she said, in helping to address concerns about the vaccine and demystify the process.
“There's a lot of work that has to be done to ensure that the vaccines that come forward that we trust in them, that we trusted the science was done right,” Besser said after months of whiplashed messaging -- and years of systemic inequality. “A casualty of that approach is trust.”
It comes down to building back that trust through transparency and an independent process, experts say.
“The race to the vaccine will be remembered as one of the greatest achievements in our modern day, but all the science in the world won't make a difference if we can't get this vaccine delivered and into the arms of people,” Brownstein said. “And I think that is still a question that is yet to be answered."
ABC News' Josh Margolin contributed to this report.




