Battling Breast Cancer at 31
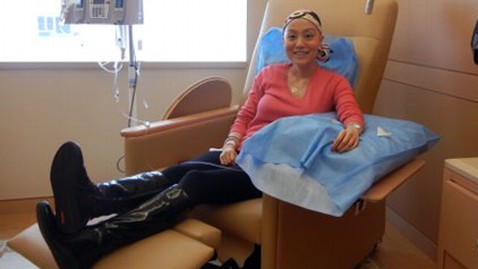
Courtesy of Tomomi Arikawa
Tomomi Arikawa said she always knew she would probably get breast cancer. Her mother, Keiko, had discovered the disease when she was 48, and her grandmother had been diagnosed in her 60s.
But when Arikawa discovered a lump in her breast, she was still shocked. She was only 31 years old.
“I thought, maybe they’d find some calcifications on my mammograms when I was 35 or something,” said Arikawa, who is now 32. “But I never thought I’d have a two-centimeter tumor at 31.”
The ABC News story editor told Good Housekeeping that both she and her mother had tested negative for mutations in the BRCA1 and BRCA2 genes, which give women up to an 80 percent risk of developing breast cancer at some point in their lives. The magazine reported that of the 200,000 U.S. women who get breast cancer each year, fewer than 7 percent are under age 40. And only 5 to 10 percent of new cases are linked to a family history like Arikawa’s.
Her surgeon, Dr. Elisa Port, co-director of the Dubin Breast Center at the Mount Sinai Medical Center in New York City, said although breast cancer patients like Arikawa lack the tell-tale BRCA 1 and 2 mutations, they may have genetic factors leading to breast cancer that simply haven’t been discovered yet.
“Probably in someone like Tomomi, there’s an accumulation of different genetic mutations. We just can’t test for them yet,” Port told Good Housekeeping.
“To be honest, I didn’t worry that I was going to die, because my grandmother and my mom both survived,” Arikawa said. “At that point I wasn’t fearful of death. I just realized I needed to pull it together and make some decisions.”
After talking with her surgeon, Arikawa decided to completely remove her breast with the tumor – a single mastectomy. Some women with extensive family histories of breast cancer decide to have both breasts remove to lower their risk of ever getting the disease. But Arikawa said she wasn’t ready to make that choice.
“I just couldn’t wrap my head around getting a mastectomy on a breast that had nothing wrong with it,” she said. “For me, maybe it was psychological, trying to hang on to some form of normalcy.”
Because she was so young at the time of her diagnosis, Arikawa faced another complication from the disease. The treatments she would receive might wipe out her ability to have children in the future. Arikawa had to decide if she wanted to preserve some of her eggs before her treatment.
“Not only did I have breast cancer at 31, now I have to think about having children,” Arikawa said.
Initially, Arikawa wasn’t sure she wanted to have children, for fear of passing her breast-cancer genes on to a daughter who might get the disease even earlier in life.
“Because I got it at 31, if I had kids, they may get it in their 20s or even younger,” she said. “And the other thing is, fertility preservation is not cheap.”
With the advice of her physician, Dr. Port, Arikawa decided to preserve her eggs, as an “extra insurance policy,” in case she ever decided to have children. Treatments can cost thousands of dollars, but Arikawa got financial help from Fertile Hope, an initiative of the LIVESTRONG foundation. A Fertile Hope spokeswoman said women with a cancer diagnosis who make below $75,000 are eligible for financial assistance with egg and embryo freezing and can receive donated medications to help with the treatment.
Today, Arikawa is back to work as a story editor for ABC’s “20/20.” She said she would encourage other young women with a family history of breast cancer to find a doctor they can trust with whom they can discuss all aspects of the disease.
“It’s someone you can talk to about your body and then feel assured that they’re looking out for your best interest,” she said.